Back
Infectious Diseases
Category: Abstract Submission
Infectious Diseases: Bacteria & Antimicrobials
301 - Health Disparities in Antibiotic Choice in Pediatric Urgent Cares Centers
Friday, April 22, 2022
6:15 PM – 8:45 PM US MT
Poster Number: 301
Publication Number: 301.114
Publication Number: 301.114
Amanda Nedved, Children's Mercy, Lenexa, KS, United States; Ann Wirtz, Children's Mercy Hospitals and Clinics, Kansas City, MO, United States; Elizabeth A. Monsees, Children's Mercy Hospitals and Clinics, Kansas City, MO, United States; Brian R. Lee, Children's Mercy Hospitals and Clinics, Kansas City, MO, United States; Rana E. El Feghaly, Children’s Mercy Kansas City, UMKC, Kansas City, MO, United States
- AN
Amanda Nedved, MD
Pediatric Urgent Care Physician
Children's Mercy
UMKC School of Medicine | KU School of Medicine
Lenexa, Kansas, United States
Presenting Author(s)
Background: Socioeconomic differences in pediatric patients who receive unnecessary antibiotics for viral infections have been reported in acute and ambulatory settings. Given that pediatric urgent care (PUC) centers have a high rate of inappropriate antibiotic prescribing, there is opportunity to examine health disparities observed in choice of antibiotic prescribed for common pediatric infections.
Objective: To determine if there are health disparities in the rate of PUC clinicians prescribing recommended first-line antibiotic agent for common pediatric infections
Design/Methods: We reviewed all encounters at 3 freestanding PUC centers within our organization for patients >60 days and < 18 years with a diagnosis of acute otitis media (AOM), group A streptococcal (GAS) pharyngitis, community acquired pneumonia (CAP), urinary tract infection (UTI), cellulitis, abscess, and animal bites who were prescribed systemic antibiotics between August 2018 and December 2020. We excluded patients who were transferred, admitted, or had a concomitant diagnosis that required systemic antibiotics. Antibiotic prescription data was evaluated for use of first-line agent per condition as recommended per national guidelines. Multivariable regression was performed to stratify by diagnosis to determine the odds ratio of appropriate antibiotic agent by race/ethnicity, language, and insurance type as documented in the electronic medical record.
Results: Hispanic and black, non-Hispanic patients received first-line antibiotic prescriptions for all conditions more frequently compared to white, non-Hispanic patients. After variable adjustment, white, non-Hispanic patients and those with commercial insurance were less likely to receive the recommended first line treatment for AOM compared to other races and insurance types, respectively (Table 1). Black non-Hispanic patients were more likely to receive recommended first-line treatment compared to white non-Hispanic patients for pneumonia (OR 1.86 [1.26, 2.82]) and GAS pharyngitis (OR 1.92 [1.36, 2.79]). After adjusting for other variables, we did not identify differences in prescribing behaviors based on language.Conclusion(s): Despite national guidelines that recommend antibiotic agent based on presenting condition we identified prescriptions for first-line treatment in select pediatric infections in the PUC setting varies by socioeconomic characteristics. When developing antibiotic stewardship initiatives, it is important to understanding how implicit biases may influence prescribing behaviors.
Table 1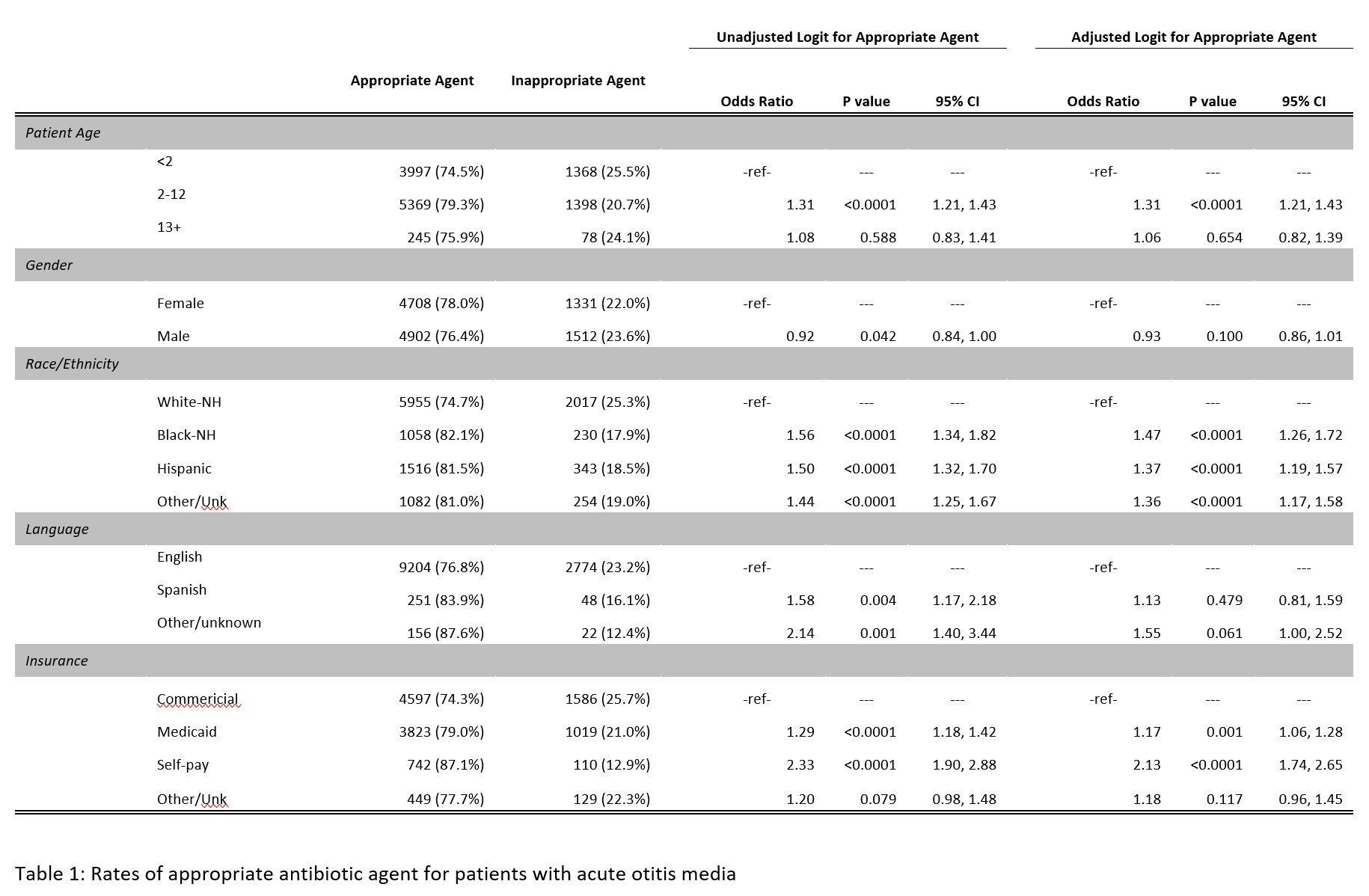 Rates of appropriate antibiotic agent for acute otitis media
Rates of appropriate antibiotic agent for acute otitis media
Objective: To determine if there are health disparities in the rate of PUC clinicians prescribing recommended first-line antibiotic agent for common pediatric infections
Design/Methods: We reviewed all encounters at 3 freestanding PUC centers within our organization for patients >60 days and < 18 years with a diagnosis of acute otitis media (AOM), group A streptococcal (GAS) pharyngitis, community acquired pneumonia (CAP), urinary tract infection (UTI), cellulitis, abscess, and animal bites who were prescribed systemic antibiotics between August 2018 and December 2020. We excluded patients who were transferred, admitted, or had a concomitant diagnosis that required systemic antibiotics. Antibiotic prescription data was evaluated for use of first-line agent per condition as recommended per national guidelines. Multivariable regression was performed to stratify by diagnosis to determine the odds ratio of appropriate antibiotic agent by race/ethnicity, language, and insurance type as documented in the electronic medical record.
Results: Hispanic and black, non-Hispanic patients received first-line antibiotic prescriptions for all conditions more frequently compared to white, non-Hispanic patients. After variable adjustment, white, non-Hispanic patients and those with commercial insurance were less likely to receive the recommended first line treatment for AOM compared to other races and insurance types, respectively (Table 1). Black non-Hispanic patients were more likely to receive recommended first-line treatment compared to white non-Hispanic patients for pneumonia (OR 1.86 [1.26, 2.82]) and GAS pharyngitis (OR 1.92 [1.36, 2.79]). After adjusting for other variables, we did not identify differences in prescribing behaviors based on language.Conclusion(s): Despite national guidelines that recommend antibiotic agent based on presenting condition we identified prescriptions for first-line treatment in select pediatric infections in the PUC setting varies by socioeconomic characteristics. When developing antibiotic stewardship initiatives, it is important to understanding how implicit biases may influence prescribing behaviors.
Table 1
 Rates of appropriate antibiotic agent for acute otitis media
Rates of appropriate antibiotic agent for acute otitis media