Back
Neonatal Clinical Trials
Category: Abstract Submission
Neonatal Clinical Trials I
426 - Non-Surgical Periodontal Disease Treatment during Pregnancy Improves Toddlers’ Autism Risk Scores
Saturday, April 23, 2022
3:30 PM – 6:00 PM US MT
Poster Number: 426
Publication Number: 426.223
Publication Number: 426.223
Gregory C. Valentine, University of Washington, Tacoma, WA, United States; Kim Boggess, UNC Chapel Hill, Chapel Hill, NC, United States; Kamaira Philips, University of North Carolina at Chapel Hill School of Medicine, Chapel Hill, NC, United States; Carl L. Bose, University of North Carolina at Chapel Hill School of Medicine, Pittsboro, NC, United States; Kevin L. Moss, Unc school of dentistry, Chapel hill, NC, United States; Julie Marchesan, University of North Carolina at Chapel Hill, Chapel Hill, NC, United States; Michael O’Shea, University of North Carolina at Chapel Hill School of Medicine, Chapel Hill, NC, United States; Myriam Peralta-Carcelen, University of Alabama at Birmingham, Birmingham, AL, United States; James D. Beck, University of North Carolina, Chapel Hill, NC, United States

Gregory C. Valentine, MD, MED, FAAP
Assistant Professor of Pediatrics, Division of Neonatology
University of Washington
Tacoma, Washington, United States
Presenting Author(s)
Background: Maternal periodontitis causes localized and systemic inflammation. Fetal exposure to maternal infection and inflammation has been associated with development of autism spectrum disorder (ASD). Treatment for periodontitis consists of non-surgical therapy to reduce dental plaque and diminish this infectious and inflammatory burden.
Objective: We sought to determine whether non-surgical periodontal therapy performed in the mid-trimester of pregnancy (intervention) compared to after pregnancy (control) is associated with reduced risk of ASD, as indicated by a screening test, the Modified Checklist for Autism in Toddlers (MCHAT).
Design/Methods: We performed a prospective, follow-up study of the offspring of women enrolled in the Maternal Oral Therapy to Reduce Obstetric Risk (MOTOR) randomized controlled trial. We determined risk of ASD by administering the M-CHAT in toddlers at 2 years of age (+ 2 months). M-CHAT failure was defined as ≥ 2 critical items or ≥3 total items failed. We measured interleukin-6 (IL-6) in cord blood. Mothers had additional IL-6 assessments at enrollment and 48-72 hours after delivery. All examiners were blinded to treatment assignment. Treatment effect was described as the risk of a failed M-CHAT among those in the intervention group relative to the risk among controls.
Results: We evaluated 306 2-year-olds. There were no baseline maternal or neonatal demographic differences based on treatment group (Table 1), but more toddlers who failed the M-CHAT than those who passed were born to self-described Caucasian mothers (78% vs 51%, p=0.008). Toddlers of women in the intervention group had a significantly decreased risk of M-CHAT failure (adjusted RR=0.53, 95% CI 0.29-0.99; Table 2). Mean IL-6 in cord blood and maternal IL-6 change from baseline was higher among offspring who failed the M-CHAT compared to those who passed (new Table 3; p=0.001 and 0.03, respectively).Conclusion(s): Treating periodontal disease during pregnancy was associated with a reduced risk of ASD, as measured by the M-CHAT. Reduction in an inflammatory marker (IL-6) is associated with lower risk of failing the M-CHAT. Considering that autism etiology implicates genetic and intrauterine exposures, antepartum periodontal treatment to reduce fetal exposure to maternal infection and inflammation may help prevent development of ASD.
Table 1: Toddler and Maternal Demographics by Treatment Group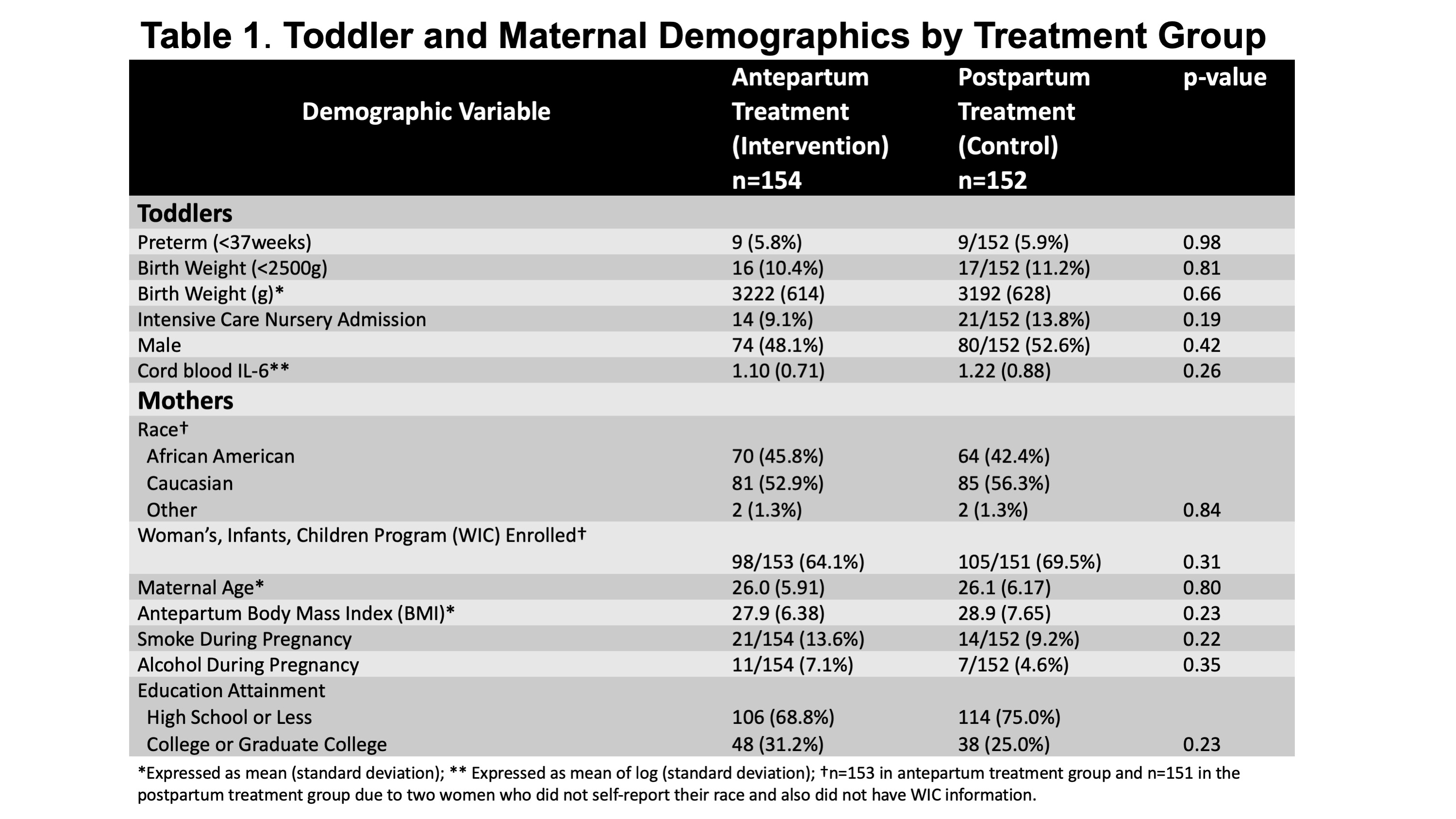
Table 2: M-CHAT Outcomes by Treatment Group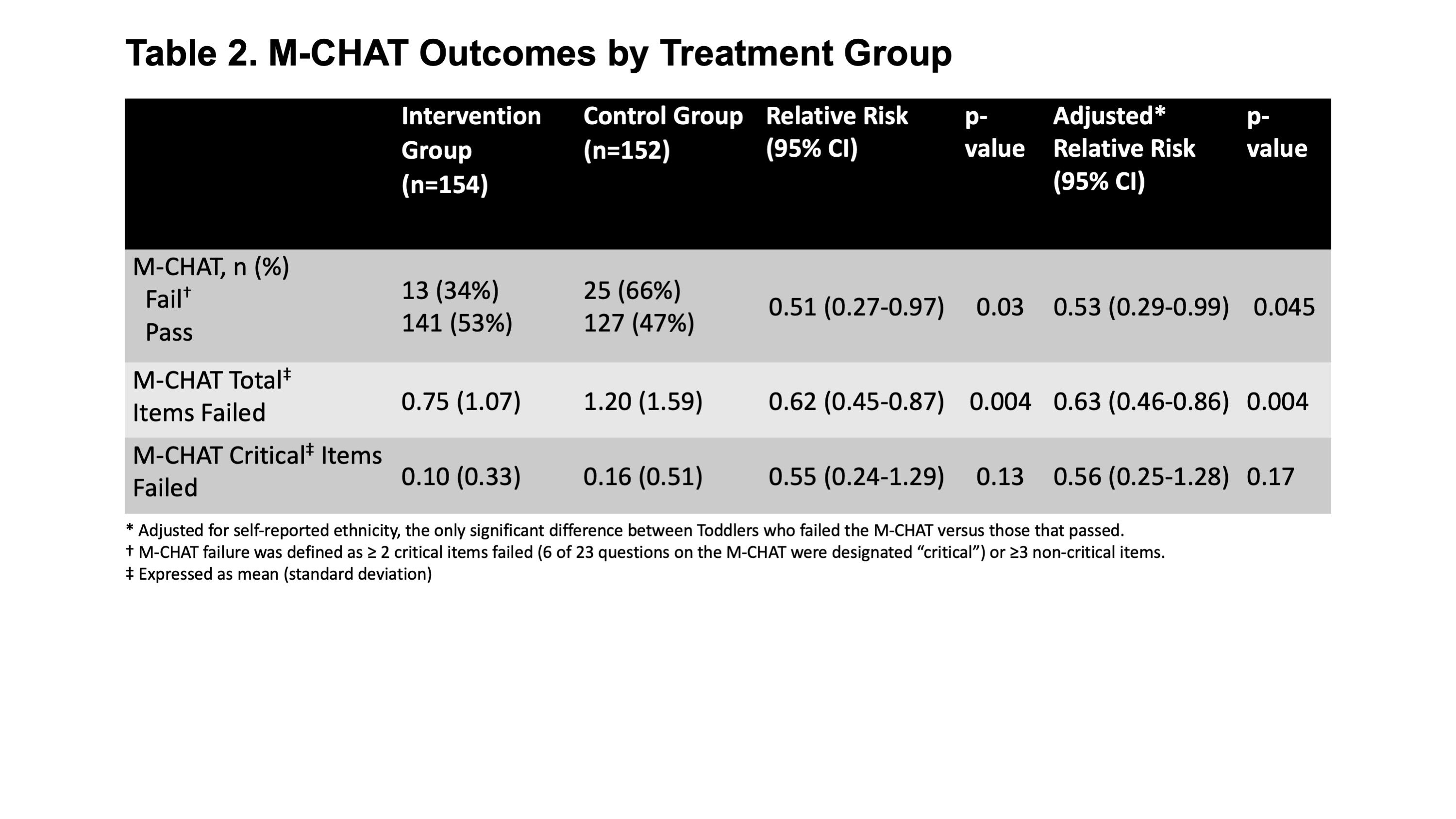
Objective: We sought to determine whether non-surgical periodontal therapy performed in the mid-trimester of pregnancy (intervention) compared to after pregnancy (control) is associated with reduced risk of ASD, as indicated by a screening test, the Modified Checklist for Autism in Toddlers (MCHAT).
Design/Methods: We performed a prospective, follow-up study of the offspring of women enrolled in the Maternal Oral Therapy to Reduce Obstetric Risk (MOTOR) randomized controlled trial. We determined risk of ASD by administering the M-CHAT in toddlers at 2 years of age (+ 2 months). M-CHAT failure was defined as ≥ 2 critical items or ≥3 total items failed. We measured interleukin-6 (IL-6) in cord blood. Mothers had additional IL-6 assessments at enrollment and 48-72 hours after delivery. All examiners were blinded to treatment assignment. Treatment effect was described as the risk of a failed M-CHAT among those in the intervention group relative to the risk among controls.
Results: We evaluated 306 2-year-olds. There were no baseline maternal or neonatal demographic differences based on treatment group (Table 1), but more toddlers who failed the M-CHAT than those who passed were born to self-described Caucasian mothers (78% vs 51%, p=0.008). Toddlers of women in the intervention group had a significantly decreased risk of M-CHAT failure (adjusted RR=0.53, 95% CI 0.29-0.99; Table 2). Mean IL-6 in cord blood and maternal IL-6 change from baseline was higher among offspring who failed the M-CHAT compared to those who passed (new Table 3; p=0.001 and 0.03, respectively).Conclusion(s): Treating periodontal disease during pregnancy was associated with a reduced risk of ASD, as measured by the M-CHAT. Reduction in an inflammatory marker (IL-6) is associated with lower risk of failing the M-CHAT. Considering that autism etiology implicates genetic and intrauterine exposures, antepartum periodontal treatment to reduce fetal exposure to maternal infection and inflammation may help prevent development of ASD.
Table 1: Toddler and Maternal Demographics by Treatment Group

Table 2: M-CHAT Outcomes by Treatment Group

