Back
Medical Education: Resident
Category: Abstract Submission
Medical Education 9 - Medical Education: Resident II
242 - CDEC: A Novel Critical Care De-Escalation Curriculum for Pediatric Trainees
Sunday, April 24, 2022
3:30 PM – 6:00 PM US MT
Poster Number: 242
Publication Number: 242.333
Publication Number: 242.333
Eleanor A. Sharp, UPMC Childrens Hospital of Pittsburgh, PITTSBURGH, PA, United States; Catherine Polak, UPMC Childrens Hospital of Pittsburgh, Pittsburgh, PA, United States; Lauren Alessi, Helen DeVos Children's Hospital, Rockford, MI, United States; Matthew Valente, UPMC Childrens Hospital of Pittsburgh, Pittsburgh, PA, United States; Li Wang, University of Pittsburgh CTSI, Pittsburgh, PA, United States; Jessica Garrison, PHM, Allison Park, PA, United States

Eleanor A. Sharp, MD
Fellow, Pediatric Hospital Medicine
UPMC Children's Hospital of Pittsburgh
PITTSBURGH, Pennsylvania, United States
Presenting Author(s)
Background: Caring for patients transferred from the Pediatric Intensive Care Unit (PICU) to the acute care floor is challenging due to patient, provider, and systems-level factors. Additionally, concepts necessary for comprehensive care de-escalation are often absent from medical school curricula and many residents lack experience with these unique issues.
Objective: We performed a needs assessment and designed a Critical Care De-Escalation Curriculum (CDEC) to address educational gaps and improve transitions of care.
Design/Methods: Attitudes, experiences, and comfort were assessed via anonymous surveys. Baseline surveys were distributed to all pediatric residents (n=121) in January 2021. The CDEC didactic series was held February – March 2021 (Figure 1). Follow-up surveys were distributed in June 2021. Exploratory surveys were distributed to the rising intern class (n=40) in July 2021. Unique identifiers linked survey responses and paired-samples t-tests evaluated for significant changes over time.
Results: 75% (91/121) and 55% (66/121) of residents responded to our baseline and follow-up survey, respectively. 68% (45/66) of respondents reported attending at least one CDEC session; of these, 98% (44/45) agreed or strongly agreed that the session(s) were helpful and 98% (44/45) felt the session(s) had changed their approach to PICU transfers. Residents reported significantly increased comfort with tasks necessary for care de-escalation, including: perform a chart review of relevant clinical data (p=0.006), identify a patient’s active issues (p=0.002), identify medication changes (p < 0.001), develop a plan of care (p < 0.001), determine antibiotic plan based on culture results (p=0.016), wean medications to avoid withdrawal (p < 0.001), manage feeding difficulties (p < 0.001), order pulmonary therapies (p < 0.001), and address barriers to discharge (p < 0.001) (Figure 2). Free text responses were overwhelmingly positive (Figure 3). Of the 36 rising interns (90% response rate), none reported prior education or experience with care de-escalation.Conclusion(s): Education surrounding pediatric critical care de-escalation is needed. As a result of our curriculum, pediatric residents reported increased comfort with tasks related to care de-escalation and ability to develop a care plan for patients transferred from the PICU to the floor.
Figure 1: Timeline of needs assessment, CDEC didactic sessions, and follow-up survey distribution.jpg) After identifying topics that residents felt uncomfortable with and/or required additional experience, we developed our Critical Care De-Escalation Curriculum using evidence-based materials focused on commonly encountered situations for pediatric patients transferred from the intensive care setting to the acute care floor. Four interactive didactic sessions covering seven high-yield topics (Access, Feeds, Microbiology, Respiratory, Medication Weans, Discharge Planning, and Overview by Systems) were held February – March 2021 for all pediatric residents.
After identifying topics that residents felt uncomfortable with and/or required additional experience, we developed our Critical Care De-Escalation Curriculum using evidence-based materials focused on commonly encountered situations for pediatric patients transferred from the intensive care setting to the acute care floor. Four interactive didactic sessions covering seven high-yield topics (Access, Feeds, Microbiology, Respiratory, Medication Weans, Discharge Planning, and Overview by Systems) were held February – March 2021 for all pediatric residents.
Figure 2: Resident comfort caring for patients transferred from the PICU before and after CDEC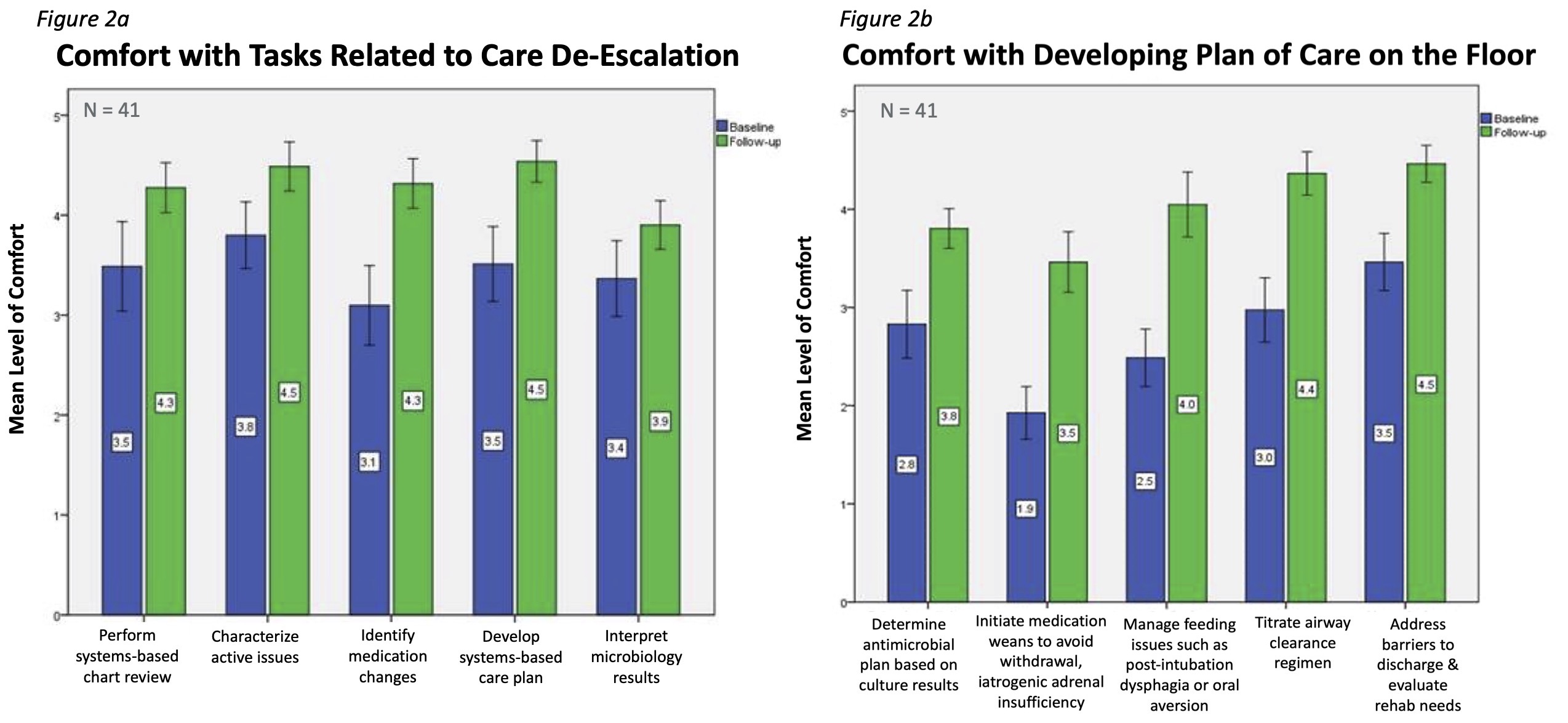 Figure 2a & 2b: Residents were asked to rate level of comfort using a Likert-scale, with 1 indicating “extremely uncomfortable” and 5 indicating, “extremely comfortable”. Level of comfort significantly increased in all domains after initiation of the noon conference curriculum. Additionally, 97.6% of respondents (n=40) somewhat or strongly agreed that the CDEC sessions had changed their approach to PICU transfers.
Figure 2a & 2b: Residents were asked to rate level of comfort using a Likert-scale, with 1 indicating “extremely uncomfortable” and 5 indicating, “extremely comfortable”. Level of comfort significantly increased in all domains after initiation of the noon conference curriculum. Additionally, 97.6% of respondents (n=40) somewhat or strongly agreed that the CDEC sessions had changed their approach to PICU transfers.
Objective: We performed a needs assessment and designed a Critical Care De-Escalation Curriculum (CDEC) to address educational gaps and improve transitions of care.
Design/Methods: Attitudes, experiences, and comfort were assessed via anonymous surveys. Baseline surveys were distributed to all pediatric residents (n=121) in January 2021. The CDEC didactic series was held February – March 2021 (Figure 1). Follow-up surveys were distributed in June 2021. Exploratory surveys were distributed to the rising intern class (n=40) in July 2021. Unique identifiers linked survey responses and paired-samples t-tests evaluated for significant changes over time.
Results: 75% (91/121) and 55% (66/121) of residents responded to our baseline and follow-up survey, respectively. 68% (45/66) of respondents reported attending at least one CDEC session; of these, 98% (44/45) agreed or strongly agreed that the session(s) were helpful and 98% (44/45) felt the session(s) had changed their approach to PICU transfers. Residents reported significantly increased comfort with tasks necessary for care de-escalation, including: perform a chart review of relevant clinical data (p=0.006), identify a patient’s active issues (p=0.002), identify medication changes (p < 0.001), develop a plan of care (p < 0.001), determine antibiotic plan based on culture results (p=0.016), wean medications to avoid withdrawal (p < 0.001), manage feeding difficulties (p < 0.001), order pulmonary therapies (p < 0.001), and address barriers to discharge (p < 0.001) (Figure 2). Free text responses were overwhelmingly positive (Figure 3). Of the 36 rising interns (90% response rate), none reported prior education or experience with care de-escalation.Conclusion(s): Education surrounding pediatric critical care de-escalation is needed. As a result of our curriculum, pediatric residents reported increased comfort with tasks related to care de-escalation and ability to develop a care plan for patients transferred from the PICU to the floor.
Figure 1: Timeline of needs assessment, CDEC didactic sessions, and follow-up survey distribution
.jpg) After identifying topics that residents felt uncomfortable with and/or required additional experience, we developed our Critical Care De-Escalation Curriculum using evidence-based materials focused on commonly encountered situations for pediatric patients transferred from the intensive care setting to the acute care floor. Four interactive didactic sessions covering seven high-yield topics (Access, Feeds, Microbiology, Respiratory, Medication Weans, Discharge Planning, and Overview by Systems) were held February – March 2021 for all pediatric residents.
After identifying topics that residents felt uncomfortable with and/or required additional experience, we developed our Critical Care De-Escalation Curriculum using evidence-based materials focused on commonly encountered situations for pediatric patients transferred from the intensive care setting to the acute care floor. Four interactive didactic sessions covering seven high-yield topics (Access, Feeds, Microbiology, Respiratory, Medication Weans, Discharge Planning, and Overview by Systems) were held February – March 2021 for all pediatric residents.Figure 2: Resident comfort caring for patients transferred from the PICU before and after CDEC
 Figure 2a & 2b: Residents were asked to rate level of comfort using a Likert-scale, with 1 indicating “extremely uncomfortable” and 5 indicating, “extremely comfortable”. Level of comfort significantly increased in all domains after initiation of the noon conference curriculum. Additionally, 97.6% of respondents (n=40) somewhat or strongly agreed that the CDEC sessions had changed their approach to PICU transfers.
Figure 2a & 2b: Residents were asked to rate level of comfort using a Likert-scale, with 1 indicating “extremely uncomfortable” and 5 indicating, “extremely comfortable”. Level of comfort significantly increased in all domains after initiation of the noon conference curriculum. Additionally, 97.6% of respondents (n=40) somewhat or strongly agreed that the CDEC sessions had changed their approach to PICU transfers.