Back
Nephrology: CKD
Category: Abstract Submission
Nephrology IV: Chronic Kidney Disease
61 - Distribution and determinants of serum N-terminal pro-B-type natriuretic peptide concentrations in children with CKD
Sunday, April 24, 2022
3:30 PM – 6:00 PM US MT
Poster Number: 61
Publication Number: 61.341
Publication Number: 61.341
Alex Kula, Ann & Robert H. Lurie Children's Hospital of Chicago, Chicago, IL, United States; Joseph Flynn, University of Washington School of Medicine, seattle, WA, United States; David Prince, University of Washington School of Medicine, Seattle, WA, United States; Susan L. Furth, Childrens Hospital of Philadelphia, Philadelphia, PA, United States; BRADLEY A. WARADY, CHILDREN'S MERCY KANSAS CITY, KANSAS CITY, MO, United States; Nisha Bansal, University of Washington School of Medicine, Seattle, WA, United States
- AK
Alex Kula, MD, MHS
Assistant Professor of Pediatric Nephrology
Ann & Robert H. Lurie Children's Hospital of Chicago
Chicago, Illinois, United States
Presenting Author(s)
Background:
In adults with chronic kidney disease (CKD), the widely available serum biomarker N-terminal pro-B-type natriuretic peptide (Nt-proBNP) strongly associates with CKD progression, cardiovascular disease (CVD), and death. Levels of Nt-proBNP are considered a surrogate for volume overload and may provide important mechanistic insights on CVD in CKD. Yet, the distribution and determinants of Nt-proBNP are not known in children with CKD.
Objective: The objective of this study was to investigate the distribution and clinical determinants of serum Nt-proBNP levels in a pediatric CKD population.
Design/Methods:
We measured serum Nt-proBNP levels at the baseline visit of participants with available samples enrolled in the Chronic Kidney Disease in Children Cohort (CKiD) study. CKiD enrolled individuals aged 1-18 years with an eGFR of 30-90mL/min/1.73m2. Individuals with a history of kidney transplant, dialysis within past 3 months, or structural heart disease were excluded. Nt-proBNP levels were measured via the chemiluminescent microparticle immunoassay (Vista PBNP, Siemens). Collection of echocardiographic, laboratory, and clinical measurements were protocolized. Systolic blood pressure (SBP) percentiles were defined using age, gender, and height normalized data from 2017 AAP hypertension guidelines. Descriptive statistics and multivariable linear regression models were used to determine the distribution and determinants of Nt-proBNP.
Results: At the baseline visit, 512 CKiD participants had available samples. Participants had a mean ±SD age of 12 ±4years, 40% were female, and mean eGFR was 56 ±21mL/min/1.73m2. The distribution of Nt-proBNP was skewed (Figure 1). Median (IQR) of Nt-proBNP was 73 (35, 151) pg/ml. Levels of log-transformed Nt-proBNP were inversely related to eGFR and age (Figure 2). There was no correlation of Nt-proBNP with urine protein to creatinine ratio. In adjusted models, older age, male sex, and higher eGFR were significantly associated with lower Nt-proBNP (Table 1). Higher SBP percentile was significantly associated with higher Nt-proBNP (Fold difference in Nt-proBNP [95% CI] per +10 SBP percentile: 1.03 [1.00, 1.06]). Left ventricular mass index was not associated with Nt-proBNP levels. Conclusion(s):
In a well characterized cohort of children and adolescents with CKD, lower eGFR, younger age, and higher SBP are significantly associated with higher Nt-proBNP. These results lay the foundation for future investigation of the utility of Nt-proBNP as a biomarker of CVD in pediatric CKD.
Table 1: Cross-sectional associations between baseline characteristics and levels of Nt-proBNP in children and adolescents with CKD enrolled in the Chronic Kidney Disease in Children (CKiD) study (n=512).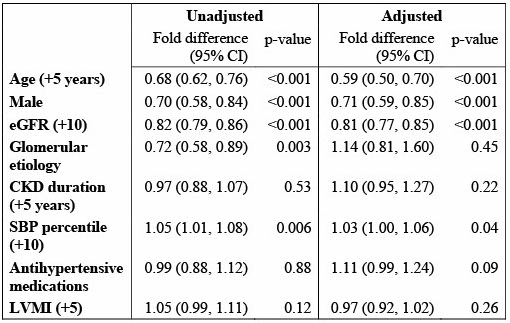 CKD: chronic kidney disease, eGFR: estimated glomerular filtration rate using serum creatinine, SBP: systolic blood pressure, LVMI: left ventricular mass index
CKD: chronic kidney disease, eGFR: estimated glomerular filtration rate using serum creatinine, SBP: systolic blood pressure, LVMI: left ventricular mass index
Figure 1: Distribution of serum levels of Nt-proBNP, before (A) and after (B) log-transformation, in children and adolescents with CKD enrolled in the Chronic Kidney Disease in Children (CKiD) study.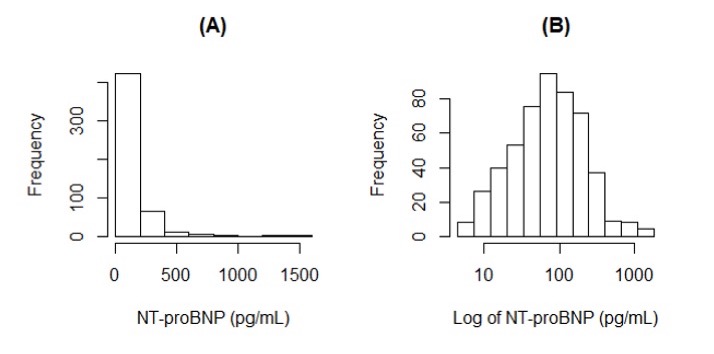
In adults with chronic kidney disease (CKD), the widely available serum biomarker N-terminal pro-B-type natriuretic peptide (Nt-proBNP) strongly associates with CKD progression, cardiovascular disease (CVD), and death. Levels of Nt-proBNP are considered a surrogate for volume overload and may provide important mechanistic insights on CVD in CKD. Yet, the distribution and determinants of Nt-proBNP are not known in children with CKD.
Objective: The objective of this study was to investigate the distribution and clinical determinants of serum Nt-proBNP levels in a pediatric CKD population.
Design/Methods:
We measured serum Nt-proBNP levels at the baseline visit of participants with available samples enrolled in the Chronic Kidney Disease in Children Cohort (CKiD) study. CKiD enrolled individuals aged 1-18 years with an eGFR of 30-90mL/min/1.73m2. Individuals with a history of kidney transplant, dialysis within past 3 months, or structural heart disease were excluded. Nt-proBNP levels were measured via the chemiluminescent microparticle immunoassay (Vista PBNP, Siemens). Collection of echocardiographic, laboratory, and clinical measurements were protocolized. Systolic blood pressure (SBP) percentiles were defined using age, gender, and height normalized data from 2017 AAP hypertension guidelines. Descriptive statistics and multivariable linear regression models were used to determine the distribution and determinants of Nt-proBNP.
Results: At the baseline visit, 512 CKiD participants had available samples. Participants had a mean ±SD age of 12 ±4years, 40% were female, and mean eGFR was 56 ±21mL/min/1.73m2. The distribution of Nt-proBNP was skewed (Figure 1). Median (IQR) of Nt-proBNP was 73 (35, 151) pg/ml. Levels of log-transformed Nt-proBNP were inversely related to eGFR and age (Figure 2). There was no correlation of Nt-proBNP with urine protein to creatinine ratio. In adjusted models, older age, male sex, and higher eGFR were significantly associated with lower Nt-proBNP (Table 1). Higher SBP percentile was significantly associated with higher Nt-proBNP (Fold difference in Nt-proBNP [95% CI] per +10 SBP percentile: 1.03 [1.00, 1.06]). Left ventricular mass index was not associated with Nt-proBNP levels. Conclusion(s):
In a well characterized cohort of children and adolescents with CKD, lower eGFR, younger age, and higher SBP are significantly associated with higher Nt-proBNP. These results lay the foundation for future investigation of the utility of Nt-proBNP as a biomarker of CVD in pediatric CKD.
Table 1: Cross-sectional associations between baseline characteristics and levels of Nt-proBNP in children and adolescents with CKD enrolled in the Chronic Kidney Disease in Children (CKiD) study (n=512).
 CKD: chronic kidney disease, eGFR: estimated glomerular filtration rate using serum creatinine, SBP: systolic blood pressure, LVMI: left ventricular mass index
CKD: chronic kidney disease, eGFR: estimated glomerular filtration rate using serum creatinine, SBP: systolic blood pressure, LVMI: left ventricular mass indexFigure 1: Distribution of serum levels of Nt-proBNP, before (A) and after (B) log-transformation, in children and adolescents with CKD enrolled in the Chronic Kidney Disease in Children (CKiD) study.

