Back
Health Services Research
Category: Abstract Submission
Health Services Research I
193 - Healthcare Utilization and Costs Among a Statewide Cohort of Young Adults by Foster Care Emancipation Status
Sunday, April 24, 2022
3:30 PM – 6:00 PM US MT
Poster Number: 193
Publication Number: 193.319
Publication Number: 193.319
James G. Kaferly, University of Colorado School of Medicine, Denver, CO, United States; Carter Sevick, University of Colorado, Denver, Aurora, CO, United States; Susan R. Mathieu, Farley Health Policy Center, Denver, CO, United States; Rebecca Orsi, Kempe Center for the Prevention and Treatment of Child Abuse and Neglect, Aurora, CO, United States; Musheng :. Alishahi, University of Colorado School of Medicine, Aurora, CO, United States; Mark Gritz, University of Colorado School of Medicine, Aurora, CO, United States

James G. Kaferly, III, MD
Pediatrician
Denver Health
University of Colorado School of Medicine
Denver, Colorado, United States
Presenting Author(s)
Background:
Twenty thousand young adults emancipate from foster care (EFC), annually, with worse health compared to non-foster care peers (NFCP) and increased health disparities as they transition to adult healthcare. Better understanding healthcare utilization and costs among EFC can inform policy, practice and transition interventions but are understudied.
Objective: To describe healthcare utilization and cost trends among matched cohorts of Medicaid-eligible EFC and NFCP young adults.
Design/Methods: The historical, observational study used child welfare, administrative and medical and behavioral health (BH) claims data for all young adults in Colorado from 2014 to 2021. We excluded those without Medicaid-eligibility in the month of and month following emancipation/reference. Matching criteria included gender, age within six months, income relative to the Federal Poverty Limit (FPL), Medicaid-eligibility pattern in the 12 months before emancipation and, using the Pediatric Medical Complexity Algorithm, version 3.0 (PMCA), the presence or absence of chronic physical and/or BH conditions. Summary data are presented.
Results: We identified 1,668 young adults for each cohort (Table 1). In the 12 months prior to the emancipation/reference month, two-thirds of EFC utilized healthcare services with higher PMPM visit averages for primary care (0.35), BH (0.45) and emergency care (0.11) and costs ($789) than the NFCP (Table 2). Among the NFCP cohort, half accessed healthcare services with fewer PMPM averaged visits in primary care (0.30), BH (0.27) and emergency (0.07) and lower costs ($709). In the 12months following the emancipation/reference month, EPC utilization reduced by nearly half (66.2% to 38.6%) while NFCP utilization reduced by one-tenth (50.0% to 45.1%). Averaged EFC encounters reduced by one third for primary care (0.21) and more than half for BH (0.19) while emergency encounters (0.12) and PMPM costs (+$199) increased in the 4 quarters after emancipation/reference month. Observed changes in NFCP utilization and cost increase were less drastic (PC 0.27; BH 0.13; ED 0.06; and +$93). Costs were highest for young adults with concurrent chronic physical and BH conditions: EFC pre-emancipation $1,240; EFC post-emancipation $1,722; NFCP pre-reference $1,322; and NFCP post-emancipation $1,489 (Figure 1).Conclusion(s): Emancipation is a critical event for EFC health with fewer services but at higher costs. Healthcare and child welfare systems must partner with EFC to identify barriers and opportunities promote successful transitions.
Table 1: Sample Characteristics of Young Adults Emancipating from Foster Care (EFC) and Non-Foster Care Peers (NFCP)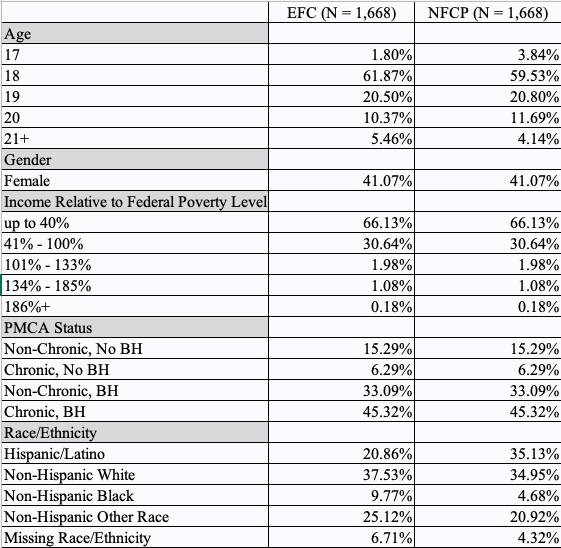
Table 2: 12 Month Averaged Utillization, Behavioral Health (BH), Primary Care (PC) and Emergency (ED) Visits and Costs for Matched EPC and NFCP Cohorts by Quarter Relative to Emancipation/Reference Month.png)
Twenty thousand young adults emancipate from foster care (EFC), annually, with worse health compared to non-foster care peers (NFCP) and increased health disparities as they transition to adult healthcare. Better understanding healthcare utilization and costs among EFC can inform policy, practice and transition interventions but are understudied.
Objective: To describe healthcare utilization and cost trends among matched cohorts of Medicaid-eligible EFC and NFCP young adults.
Design/Methods: The historical, observational study used child welfare, administrative and medical and behavioral health (BH) claims data for all young adults in Colorado from 2014 to 2021. We excluded those without Medicaid-eligibility in the month of and month following emancipation/reference. Matching criteria included gender, age within six months, income relative to the Federal Poverty Limit (FPL), Medicaid-eligibility pattern in the 12 months before emancipation and, using the Pediatric Medical Complexity Algorithm, version 3.0 (PMCA), the presence or absence of chronic physical and/or BH conditions. Summary data are presented.
Results: We identified 1,668 young adults for each cohort (Table 1). In the 12 months prior to the emancipation/reference month, two-thirds of EFC utilized healthcare services with higher PMPM visit averages for primary care (0.35), BH (0.45) and emergency care (0.11) and costs ($789) than the NFCP (Table 2). Among the NFCP cohort, half accessed healthcare services with fewer PMPM averaged visits in primary care (0.30), BH (0.27) and emergency (0.07) and lower costs ($709). In the 12months following the emancipation/reference month, EPC utilization reduced by nearly half (66.2% to 38.6%) while NFCP utilization reduced by one-tenth (50.0% to 45.1%). Averaged EFC encounters reduced by one third for primary care (0.21) and more than half for BH (0.19) while emergency encounters (0.12) and PMPM costs (+$199) increased in the 4 quarters after emancipation/reference month. Observed changes in NFCP utilization and cost increase were less drastic (PC 0.27; BH 0.13; ED 0.06; and +$93). Costs were highest for young adults with concurrent chronic physical and BH conditions: EFC pre-emancipation $1,240; EFC post-emancipation $1,722; NFCP pre-reference $1,322; and NFCP post-emancipation $1,489 (Figure 1).Conclusion(s): Emancipation is a critical event for EFC health with fewer services but at higher costs. Healthcare and child welfare systems must partner with EFC to identify barriers and opportunities promote successful transitions.
Table 1: Sample Characteristics of Young Adults Emancipating from Foster Care (EFC) and Non-Foster Care Peers (NFCP)

Table 2: 12 Month Averaged Utillization, Behavioral Health (BH), Primary Care (PC) and Emergency (ED) Visits and Costs for Matched EPC and NFCP Cohorts by Quarter Relative to Emancipation/Reference Month
.png)
