Back
Nephrology: CKD
Category: Abstract Submission
Nephrology IV: Chronic Kidney Disease
69 - Nocturnal Dipping and Kidney Function Decline in the Chronic Kidney Disease in Children Cohort
Sunday, April 24, 2022
3:30 PM – 6:00 PM US MT
Poster Number: 69
Publication Number: 69.341
Publication Number: 69.341
Christine Bakhoum, Yale University, New Haven, CT, United States; Manali Phadke, Yale School of Medicine, New Haven, CT, United States; Yanhong Deng, Yale School of Medicine, New Haven, CT, United States; Joshua Samuels, McGovern Medical School at UTHealth, Houston, TX, United States; Pranav Garimella, University of California, San Diego School of Medicine, La Jolla, CA, United States; Susan Furth, Childrens Hospital of Philadelphia, Philadelphia, PA, United States; Joachim H. Ix, University of California, San Diego School of Medicine, San Diego, CA, United States

Christine Bakhoum, MD, MAS
Assistant Professor
Yale University
New Haven, Connecticut, United States
Presenting Author(s)
Background: Normally blood pressure declines by at least 10% from daytime to nighttime. In adults, blunted nocturnal dipping has been associated with more rapid decline in kidney function, independent of 24-hour blood pressure. Absence of dipping is prevalent in children with chronic kidney disease (CKD).
Objective: Our objective was to determine if nocturnal blood pressure dipping is associated with progression to end-stage kidney disease and proteinuria in children with CKD.
Design/Methods: In the CKD in Children (CKiD) Cohort, Cox proportional hazards models were used to evaluate the relationship between baseline nocturnal dipping (≥ 10% decline in systolic and diastolic blood pressure from day to night) and progression to end-stage kidney disease (ESKD). Linear mixed effects models were used to evaluate the relationship between dipping and changes in iohexol glomerular filtration rate (iGFR) and urine protein to creatinine ratio (log-UPCR, mg/mg) over time.
Results: Among 620 participants, the mean age was 11 (± 4) years, mean iGFR was 52 (± 22) ml/min/1.73m2, and 40% were non-dippers at baseline. There were 169 ESKD events during 2.9 years (median) follow-up. Dipping status was not significantly associated with ESKD in either those with (HR 1.21 95% CI (0.53, 2.77)) or without glomerular disease (HR 1.07 95% CI (0.73, 1.59), Figure 1). Baseline dipping status was not associated with longitudinal change in iGFR (p = 0.97) or log(UPCR) (p =0.80). The effect of baseline dipping status on longitudinal change in iGFR and log(UPCR) did not vary significantly with time (interaction p-values = 0.31 and 0.35, respectively).Conclusion(s): Nocturnal dipping is not associated with ESKD, iGFR decline, or change in proteinuria in children within the CKiD cohort.
Figure 1. ESKD-free survival by dipping status in participants with non-glomerular CKD (1a) and glomerular CKD (1b).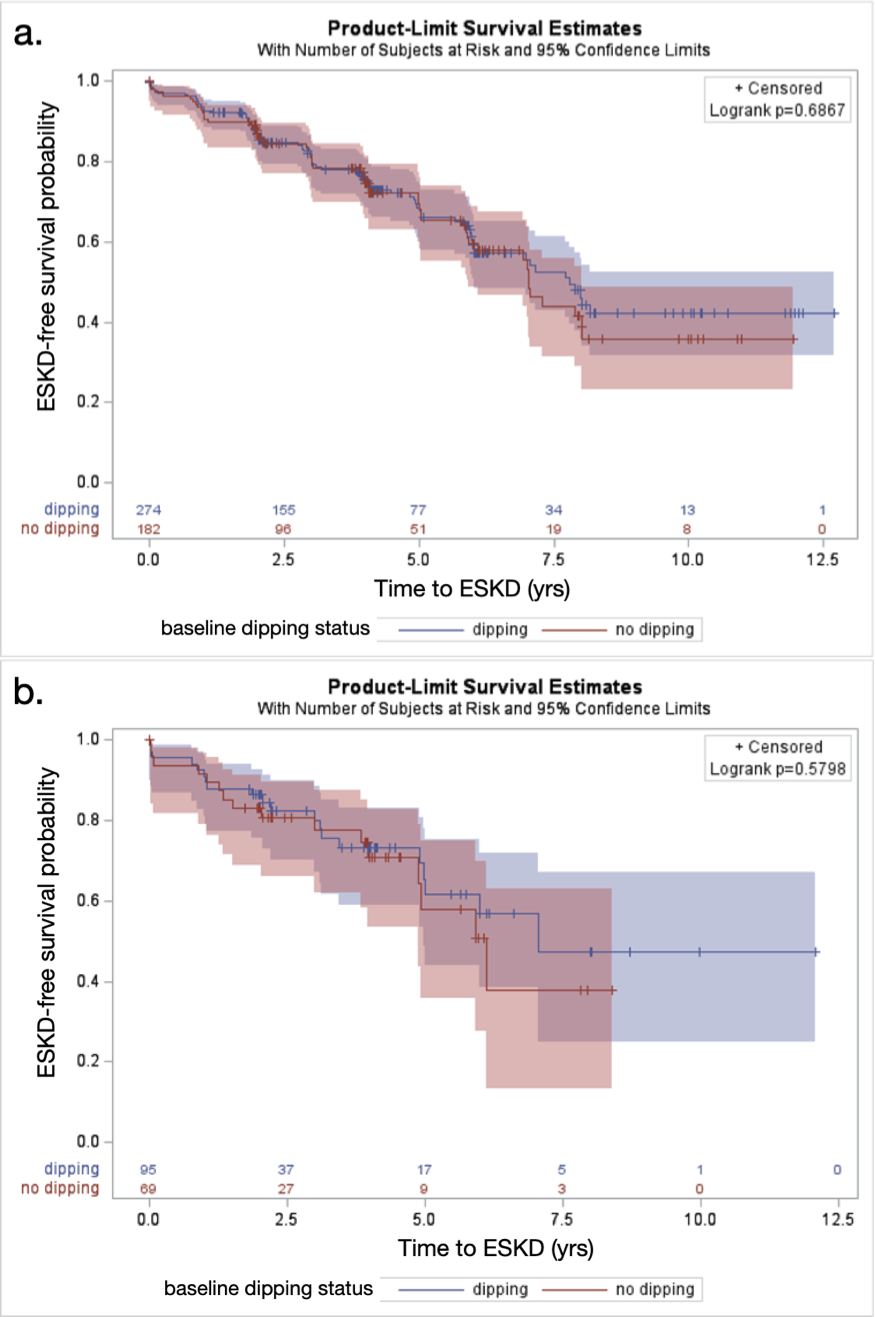
Objective: Our objective was to determine if nocturnal blood pressure dipping is associated with progression to end-stage kidney disease and proteinuria in children with CKD.
Design/Methods: In the CKD in Children (CKiD) Cohort, Cox proportional hazards models were used to evaluate the relationship between baseline nocturnal dipping (≥ 10% decline in systolic and diastolic blood pressure from day to night) and progression to end-stage kidney disease (ESKD). Linear mixed effects models were used to evaluate the relationship between dipping and changes in iohexol glomerular filtration rate (iGFR) and urine protein to creatinine ratio (log-UPCR, mg/mg) over time.
Results: Among 620 participants, the mean age was 11 (± 4) years, mean iGFR was 52 (± 22) ml/min/1.73m2, and 40% were non-dippers at baseline. There were 169 ESKD events during 2.9 years (median) follow-up. Dipping status was not significantly associated with ESKD in either those with (HR 1.21 95% CI (0.53, 2.77)) or without glomerular disease (HR 1.07 95% CI (0.73, 1.59), Figure 1). Baseline dipping status was not associated with longitudinal change in iGFR (p = 0.97) or log(UPCR) (p =0.80). The effect of baseline dipping status on longitudinal change in iGFR and log(UPCR) did not vary significantly with time (interaction p-values = 0.31 and 0.35, respectively).Conclusion(s): Nocturnal dipping is not associated with ESKD, iGFR decline, or change in proteinuria in children within the CKiD cohort.
Figure 1. ESKD-free survival by dipping status in participants with non-glomerular CKD (1a) and glomerular CKD (1b).

