Back
Children with Chronic Conditions
Category: Abstract Submission
Children with Chronic Conditions II
154 - Respiratory Culture Growth and 3-Year Lung Health Outcomes in Children with BPD and Tracheostomies
Sunday, April 24, 2022
3:30 PM – 6:00 PM US MT
Poster Number: 154
Publication Number: 154.305
Publication Number: 154.305
Rebecca Steuart, Medical College of Wisconsin, Milwaukee, WI, United States; Abigail E. Woolums, Cincinnati Children's Hospital Medical Center, Cincinnati, OH, United States; Dan Benscoter, Cincinnati Children's Hospital Medical Center, Cincinnati, OH, United States; Samir S. Shah, Journal of Hospital Medicine, Cincinnati, OH, United States; Joanna Thomson, Cincinnati Children's Hospital Medical Center, Cincinnati, OH, United States

Rebecca Steuart, MD MS
Assistant Professor of Pediatrics, Complex Care Program
Medical College of Wisconsin
Milwaukee, Wisconsin, United States
Presenting Author(s)
Background: Certain bacteria, when isolated on respiratory cultures, have been associated with worse short-term outcomes in children with bronchopulmonary dysplasia (BPD) and tracheostomies. It is unknown if these pathogenic bacteria influence respiratory support outcomes in the longer term.
Objective: To determine if respiratory culture growth of pathogenic organisms is associated with ongoing need for respiratory support 3 years post-tracheostomy placement in children with BPD and tracheostomies.
Design/Methods: This single center, retrospective cohort study included respiratory culture results of children with BPD and new tracheostomies who had >1 respiratory culture obtained in the 3 years (i.e., 36 months) post-tracheostomy placement between 2010-2018. The primary exposure was growth of a pathogen on respiratory culture, defined a priori as an organism not expected in oropharyngeal flora, including: Pseudomonas aeruginosa, Staphylococcus aureus, and Klebsiella pneumoniae. The primary outcome was the alive child’s continued use of respiratory support (oxygen, positive pressure) at 3 years post-tracheostomy placement; secondary outcomes were decannulation and death at 3 years post-placement. Mixed-effects logistic regression models controlling for patient- and culture-level covariates and within-patient clustering were used to examine the relationship between respiratory culture growth and outcomes.
Results: Among the 2,103 respiratory cultures obtained from 182 children, 297 (14.2%) had isolation of pathogenic respiratory organisms (Table 1), most frequently P. aeruginosa (Table 2). Compared with negative cultures, cultures with pathogens were more likely in children with 4+ complex chronic conditions and newer tracheostomies, but less likely in children with chronic ventilator use. In adjusted analysis, pathogenic organism growth was not associated with ongoing use of respiratory support at 3 years post-tracheostomy (adjusted odds ratio 1.14, [95% confidence interval 0.22 – 6.00], Table 3) or death (aOR 1.39, [95% CI 0.14-13.99]), but pathogen growth was associated with failure to decannulate by 3 years (aOR 0.531, [95% CI 0.530-0.532]). No differences in respiratory support, decannulation, or mortality outcomes were identified for cultures with P. aeruginosa or recurrent P. aeruginosa growth specifically in unadjusted analysis.Conclusion(s): Among children with BPD and tracheostomies, respiratory culture growth of pathogenic organisms is associated with failure to decannulate by 3 years post-tracheostomy, but does not predict continued need for respiratory support or mortality.
Table 1. Respiratory culture cohort clinical characteristics..jpg)
Table 2. Respiratory culture characteristics.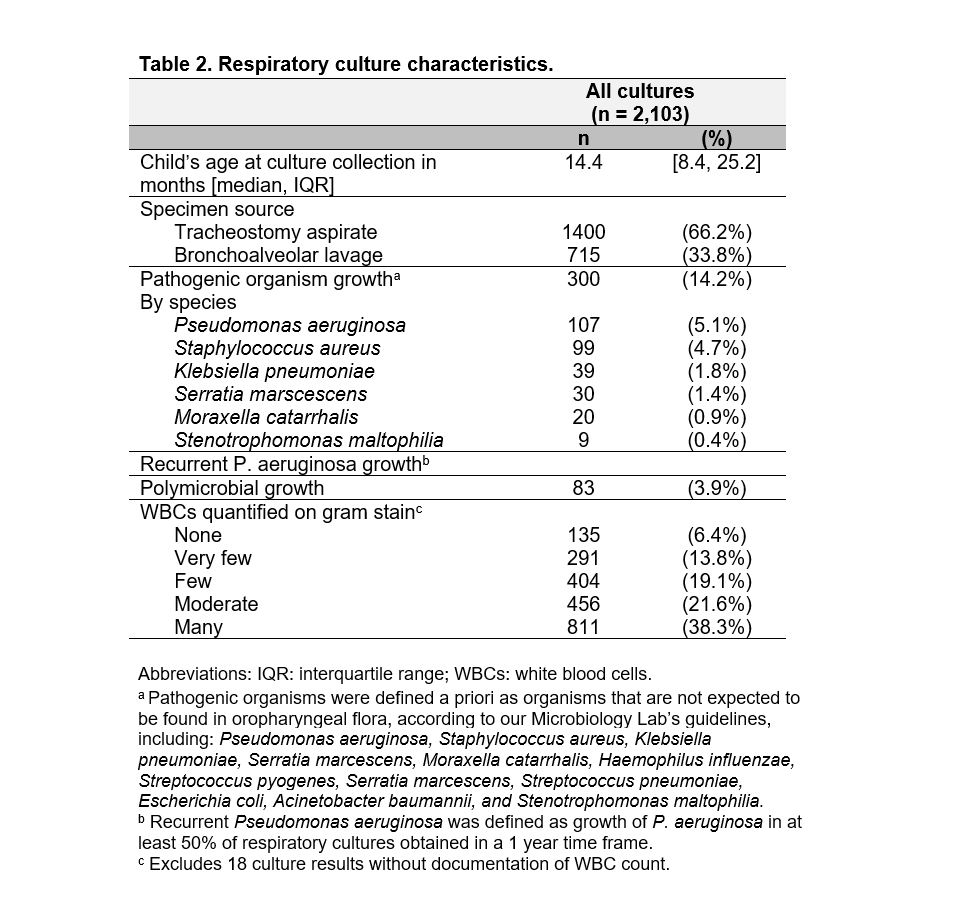
Objective: To determine if respiratory culture growth of pathogenic organisms is associated with ongoing need for respiratory support 3 years post-tracheostomy placement in children with BPD and tracheostomies.
Design/Methods: This single center, retrospective cohort study included respiratory culture results of children with BPD and new tracheostomies who had >1 respiratory culture obtained in the 3 years (i.e., 36 months) post-tracheostomy placement between 2010-2018. The primary exposure was growth of a pathogen on respiratory culture, defined a priori as an organism not expected in oropharyngeal flora, including: Pseudomonas aeruginosa, Staphylococcus aureus, and Klebsiella pneumoniae. The primary outcome was the alive child’s continued use of respiratory support (oxygen, positive pressure) at 3 years post-tracheostomy placement; secondary outcomes were decannulation and death at 3 years post-placement. Mixed-effects logistic regression models controlling for patient- and culture-level covariates and within-patient clustering were used to examine the relationship between respiratory culture growth and outcomes.
Results: Among the 2,103 respiratory cultures obtained from 182 children, 297 (14.2%) had isolation of pathogenic respiratory organisms (Table 1), most frequently P. aeruginosa (Table 2). Compared with negative cultures, cultures with pathogens were more likely in children with 4+ complex chronic conditions and newer tracheostomies, but less likely in children with chronic ventilator use. In adjusted analysis, pathogenic organism growth was not associated with ongoing use of respiratory support at 3 years post-tracheostomy (adjusted odds ratio 1.14, [95% confidence interval 0.22 – 6.00], Table 3) or death (aOR 1.39, [95% CI 0.14-13.99]), but pathogen growth was associated with failure to decannulate by 3 years (aOR 0.531, [95% CI 0.530-0.532]). No differences in respiratory support, decannulation, or mortality outcomes were identified for cultures with P. aeruginosa or recurrent P. aeruginosa growth specifically in unadjusted analysis.Conclusion(s): Among children with BPD and tracheostomies, respiratory culture growth of pathogenic organisms is associated with failure to decannulate by 3 years post-tracheostomy, but does not predict continued need for respiratory support or mortality.
Table 1. Respiratory culture cohort clinical characteristics.
.jpg)
Table 2. Respiratory culture characteristics.

