Back
Nephrology: Clinical
Category: Abstract Submission
Nephrology III: General Nephrology and Dialysis
54 - Serum Renin Levels Refine Acute Kidney Injury Prediction in Critically Ill Children
Sunday, April 24, 2022
3:30 PM – 6:00 PM US MT
Poster Number: 54
Publication Number: 54.340
Publication Number: 54.340
Naomi Pode Shakked, Cincinnati Children's Hospital Medical Center, Cincinnati, OH, United States; Natalja L. Stanski, Cincinnati Children's Hospital Medical Center, Cincinnati, OH, United States; Stuart L. Goldstein, Cincinnati Children's Hospital, Cincinnati, OH, United States
- NP
Naomi Pode Shakked, MD, PhD
Fellow
Cincinnati Children's Hospital Medical Center
Cincinnati, Ohio, United States
Presenting Author(s)
Background: Acute kidney injury (AKI) is common in the pediatric intensive care unit (PICU) and portends an increased risk for poor outcomes, including death. Unfortunately, treatments are limited, and thus early risk stratification of children for severe AKI (sAKI) is important, as it could facilitate targeted, renal protective interventions. Recent adult studies have demonstrated a correlation between early elevation in serum renin level and development of sAKI.
Objective: We sought to assess whether serum renin levels, early in the disease course are associated with development of sAKI in children.
Design/Methods: We performed a prospective pilot study of children admitted to the PICU and enrolled in the Trial in AKI using NGAL and Fluid Overload to Optimize CRRT Use (TAKING FOCUS 2, NCT03541785; Figure 1). All patients enrolled had a Renal Angina Index (RAI) calculated at 12 hours of PICU admission and urine neutrophil gelatinase-associated lipocalin (uNGAL) measured if RAI≥8 (high risk sAKI= RAI≥8 and uNGAL ≥150 ng/ml). 43 patients were enrolled in our study. We assessed for associations between renin levels (both alone and in concert with the RAI/uNGAL paradigm) and our primary outcomes of Day2-4 sAKI (≥KDIGO stage 2) and receipt of renal replacement therapy (RRT). Response to a furosemide stress test (FST) was a secondary outcome.
Results: 21/43 (49%) patients had Day2-4 sAKI and 8/43 (19%) received RRT. Median Day1 renin level was 59.6 pg/ml (IQR 21,128), and there were no differences between patients with and without either primary outcome. An optimal cutoff for Day1 renin of 100 pg/ml was identified to discriminate between patients with and without Day2-4 sAKI (Youden Index 0.2). Although Day1 renin alone was poorly correlated with both primary outcomes, patients with RAI≥8 had higher Day1 renin levels compared to those with RAI < 8 (median 72.3 vs. 21.6 pg/ml, p < 0.05). When Day1 renin ≥100 pg/ml was added to the RAI/uNGAL sAKI prediction paradigm (Figure 1), specificity of Day2-4 sAKI (82% vs. 59%) and RRT use (74% vs. 44%) prediction improved. Finally, 12 patients underwent FST, and median Day1 renin levels discriminated between responders (n=8) (101 pg/ml, IQR 32,485) and non-responders (n=4) (537 pg/ml, IQR 95,2182).Conclusion(s): Elevated Day1 renin level may refine sAKI risk stratification when integrated with the RAI and uNGAL. Elevated renin levels also appear to identify FST non-responders who may benefit from earlier RRT. Further study is warranted to validate these findings.
Naomi Pode Shakked Biosketch November 2021 new format.pdf
Figure 2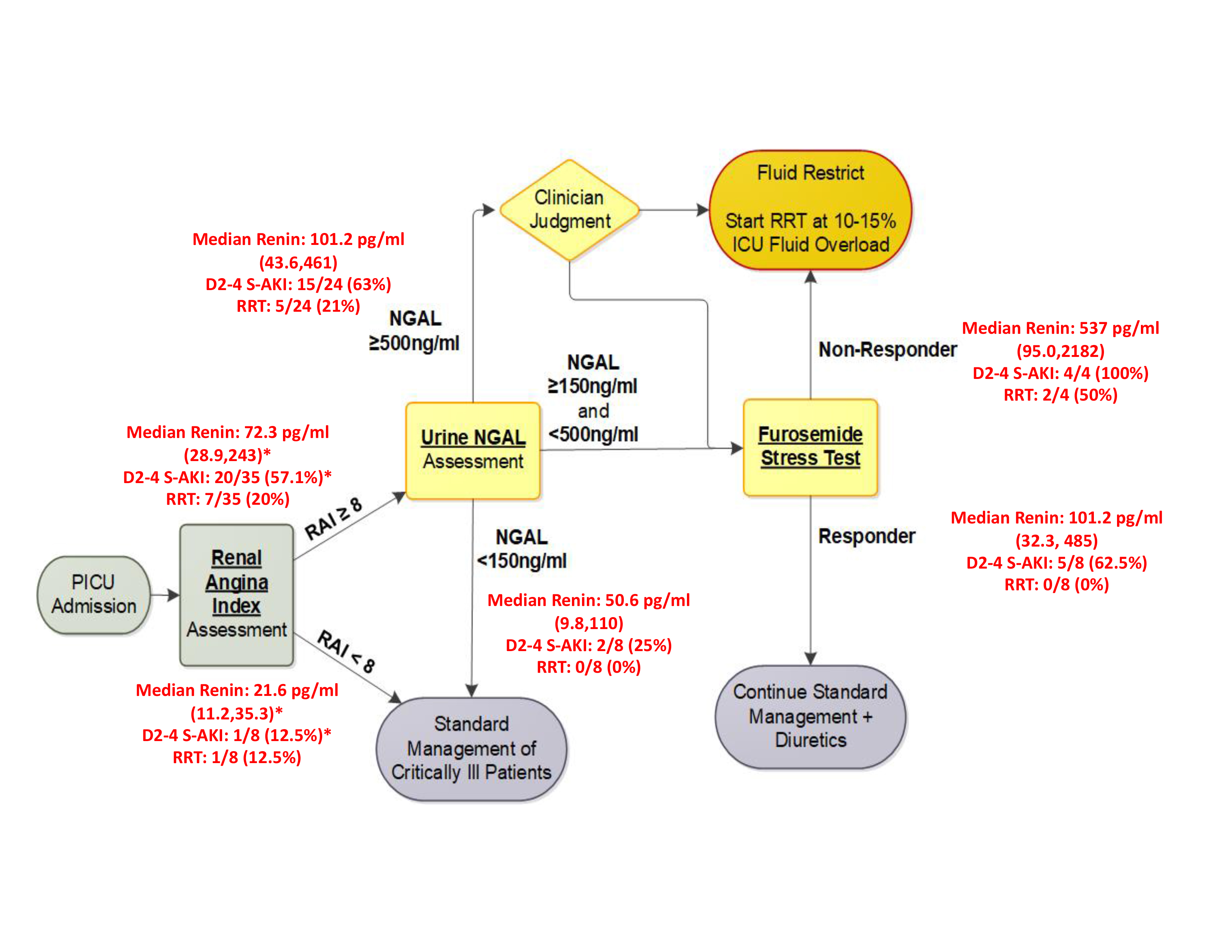 Presented in red are median, 25th and 75th percentile of serum renin levels as well as percentages of D2-4 sAKI and need for RRT in each branch point of the TAKING FOCUS 2 algorithm for risk stratification of sAKI in pediatric patients admitted to the ICU.
Presented in red are median, 25th and 75th percentile of serum renin levels as well as percentages of D2-4 sAKI and need for RRT in each branch point of the TAKING FOCUS 2 algorithm for risk stratification of sAKI in pediatric patients admitted to the ICU.
Objective: We sought to assess whether serum renin levels, early in the disease course are associated with development of sAKI in children.
Design/Methods: We performed a prospective pilot study of children admitted to the PICU and enrolled in the Trial in AKI using NGAL and Fluid Overload to Optimize CRRT Use (TAKING FOCUS 2, NCT03541785; Figure 1). All patients enrolled had a Renal Angina Index (RAI) calculated at 12 hours of PICU admission and urine neutrophil gelatinase-associated lipocalin (uNGAL) measured if RAI≥8 (high risk sAKI= RAI≥8 and uNGAL ≥150 ng/ml). 43 patients were enrolled in our study. We assessed for associations between renin levels (both alone and in concert with the RAI/uNGAL paradigm) and our primary outcomes of Day2-4 sAKI (≥KDIGO stage 2) and receipt of renal replacement therapy (RRT). Response to a furosemide stress test (FST) was a secondary outcome.
Results: 21/43 (49%) patients had Day2-4 sAKI and 8/43 (19%) received RRT. Median Day1 renin level was 59.6 pg/ml (IQR 21,128), and there were no differences between patients with and without either primary outcome. An optimal cutoff for Day1 renin of 100 pg/ml was identified to discriminate between patients with and without Day2-4 sAKI (Youden Index 0.2). Although Day1 renin alone was poorly correlated with both primary outcomes, patients with RAI≥8 had higher Day1 renin levels compared to those with RAI < 8 (median 72.3 vs. 21.6 pg/ml, p < 0.05). When Day1 renin ≥100 pg/ml was added to the RAI/uNGAL sAKI prediction paradigm (Figure 1), specificity of Day2-4 sAKI (82% vs. 59%) and RRT use (74% vs. 44%) prediction improved. Finally, 12 patients underwent FST, and median Day1 renin levels discriminated between responders (n=8) (101 pg/ml, IQR 32,485) and non-responders (n=4) (537 pg/ml, IQR 95,2182).Conclusion(s): Elevated Day1 renin level may refine sAKI risk stratification when integrated with the RAI and uNGAL. Elevated renin levels also appear to identify FST non-responders who may benefit from earlier RRT. Further study is warranted to validate these findings.
Naomi Pode Shakked Biosketch November 2021 new format.pdf
Figure 2
 Presented in red are median, 25th and 75th percentile of serum renin levels as well as percentages of D2-4 sAKI and need for RRT in each branch point of the TAKING FOCUS 2 algorithm for risk stratification of sAKI in pediatric patients admitted to the ICU.
Presented in red are median, 25th and 75th percentile of serum renin levels as well as percentages of D2-4 sAKI and need for RRT in each branch point of the TAKING FOCUS 2 algorithm for risk stratification of sAKI in pediatric patients admitted to the ICU.