Back
Telemedicine/EHR/Medical Informatics
Category: Abstract Submission
Telemedicine/EHR/Medical Informatics II
306 - Telehealth utilization among transgender and gender diverse adolescents: Assessment of Seattle Children’s Gender Clinic telehealth visits
Sunday, April 24, 2022
3:30 PM – 6:00 PM US MT
Poster Number: 306
Publication Number: 306.347
Publication Number: 306.347
Ruby A. Lucas, University of Washington, Seattle, WA, United States; Nicole F. Kahn, Seattle Children's Research Institute, Seattle, WA, United States; Kevin Bocek, Seattle Children's Hospital, Seattle, WA, United States; Diana M. Tordoff, University of Washington, Seattle, WA, United States; Baer karrington, University of Washington School of Medicine, Seattle, WA, United States; Laura Richardson, University of Washington School of Medicine, Seattle, WA, United States; Gina Sequeira, Seattle Children's, Seattle, WA, United States

Ruby A. Lucas, BA
MPH Candidate in Epidemiology
University of Washington
Seattle, Washington, United States
Presenting Author(s)
Background: The expansion of telehealth services during the COVID-19 pandemic has allowed for continued access to care for many patients, but little is known about whether it has removed or exacerbated existing barriers in access to gender-affirming care for transgender and gender diverse (TGD) youth.
Objective: To understand whether demographic characteristics of TGD patients receiving care in the Seattle Children’s Gender Clinic (SCGC) changed with the availability of telehealth services for gender-affirming care in March 2020.
Design/Methods: We used electronic health record data to identify all patients who had an ICD-10 diagnosis of gender dysphoria and completed a medical visit at SCGC, either in-person or through telehealth, between March 2019-February 2021. Chi-squared tests were used to assess differences in demographic characteristics and care utilization between 1) telehealth and non-telehealth users in the post-telehealth period and 2) those receiving care between March 2019-February 2020 (pre-telehealth) and March 2020-February 2021 (post-telehealth).
Results: Of 1,061 unique patients during the study period (mean age: 15.6 years) 61.8% identified as transmasculine/male, 67.7% identified as non-Hispanic White and 63.8% were commercially insured. A majority (91.6%) resided in an urban area and 66.8% were located within 35 miles of SCGC. At least 1 patient was seen from most Washington counties, however the percent change in the number of patients seen in each county from the pre- vs post telehealth periods varied across counties (Figures 1 & 2). In the post-telehealth period, 48.6% of all visits were conducted via telehealth (Figure 3); however, there were no significant differences in telehealth utilization by demographic characteristics. In comparison to the pre-telehealth period, a larger proportion of patients in the post-telehealth period had self-pay/charity care insurance (6.2% vs 1.8%; p< 0.001) and used they/them, he/they, or she/they pronouns (17.6% vs 11.9%; p=0.007). Conclusion(s): Findings indicate that demographic characteristics of SCGC patients remained relatively consistent with the introduction of telehealth services. Although this suggests that telehealth has not introduced new disparities in access to gender-affirming care, youth of color and rural youth are still disproportionately underrepresented. Overall, these findings improve our understanding of how telehealth has affected access to gender-affirming care and can be used to advocate for evidence-based policies to improve care delivery and reduce health inequities among TGD youth.
Figure 1. Number of Patients Seen During Study Period (2019-2021) by County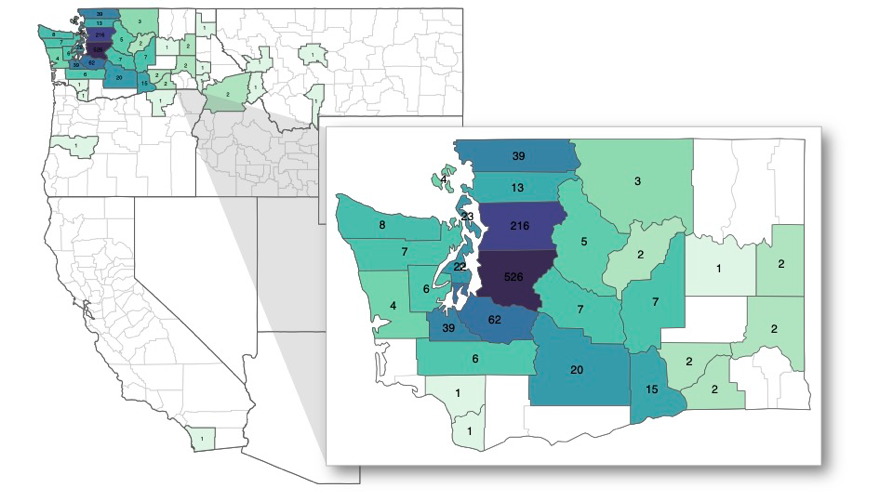
Figure 2. Percent Change in the Number of Patients Seen Between Pre- and Post-Telehealth Periods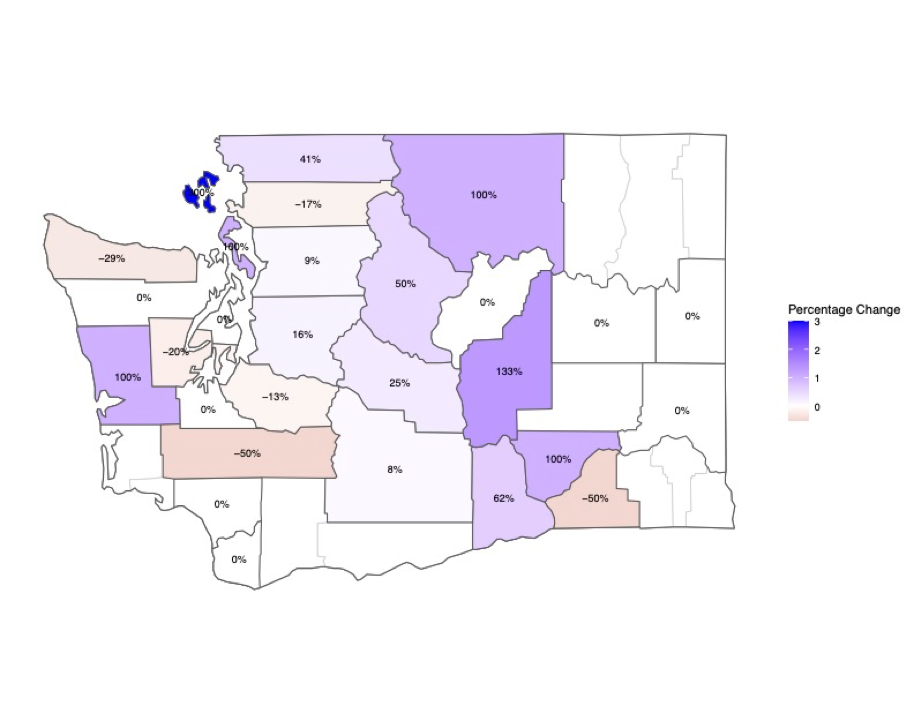
Objective: To understand whether demographic characteristics of TGD patients receiving care in the Seattle Children’s Gender Clinic (SCGC) changed with the availability of telehealth services for gender-affirming care in March 2020.
Design/Methods: We used electronic health record data to identify all patients who had an ICD-10 diagnosis of gender dysphoria and completed a medical visit at SCGC, either in-person or through telehealth, between March 2019-February 2021. Chi-squared tests were used to assess differences in demographic characteristics and care utilization between 1) telehealth and non-telehealth users in the post-telehealth period and 2) those receiving care between March 2019-February 2020 (pre-telehealth) and March 2020-February 2021 (post-telehealth).
Results: Of 1,061 unique patients during the study period (mean age: 15.6 years) 61.8% identified as transmasculine/male, 67.7% identified as non-Hispanic White and 63.8% were commercially insured. A majority (91.6%) resided in an urban area and 66.8% were located within 35 miles of SCGC. At least 1 patient was seen from most Washington counties, however the percent change in the number of patients seen in each county from the pre- vs post telehealth periods varied across counties (Figures 1 & 2). In the post-telehealth period, 48.6% of all visits were conducted via telehealth (Figure 3); however, there were no significant differences in telehealth utilization by demographic characteristics. In comparison to the pre-telehealth period, a larger proportion of patients in the post-telehealth period had self-pay/charity care insurance (6.2% vs 1.8%; p< 0.001) and used they/them, he/they, or she/they pronouns (17.6% vs 11.9%; p=0.007). Conclusion(s): Findings indicate that demographic characteristics of SCGC patients remained relatively consistent with the introduction of telehealth services. Although this suggests that telehealth has not introduced new disparities in access to gender-affirming care, youth of color and rural youth are still disproportionately underrepresented. Overall, these findings improve our understanding of how telehealth has affected access to gender-affirming care and can be used to advocate for evidence-based policies to improve care delivery and reduce health inequities among TGD youth.
Figure 1. Number of Patients Seen During Study Period (2019-2021) by County

Figure 2. Percent Change in the Number of Patients Seen Between Pre- and Post-Telehealth Periods

