Back
Telemedicine/EHR/Medical Informatics
Category: Abstract Submission
Telemedicine/EHR/Medical Informatics II
307 - The Empty SmartLink Solution: A QI Initiative to Improve H&P Documentation Using Clinical Decision Support
Sunday, April 24, 2022
3:30 PM – 6:00 PM US MT
Poster Number: 307
Publication Number: 307.347
Publication Number: 307.347
Sabrina E. Carro, Medical College of Wisconsin Affiliated Hosp., Milwaukee, WI, United States; Sarah Milota, Medical College of Wisconsin, Milwaukee, WI, United States; Danita Hahn, Medical College of Wisconsin, Milwaukee, WI, United States; Amanda Rogers, Medical College of Wisconsin, Milwaukee, WI, United States; Sarah Bauer, Medical College of Wisconsin, Milwaukee, WI, United States

Amanda Rogers, MD
Assistant Professor Pediatric Hospital Medicine
Medical College of Wisconsin
Milwaukee, Wisconsin, United States
Presenting Author(s)
Background: The electronic health record allows documentation of patient history to make it available for future encounters. When past medical history (PMH), surgical history (PSH), and family history (FH) is documented in the History tab, it can be hyperlinked into History and Physical (H&P) notes via SmartLinks. However, if no history is ever entered, the SmartLinks will be empty and default as “no history on file” (Figure 1a). These empty SmartLinks highlight missed opportunities for complete H&P documentation, an important component of patient care.
Objective: Baseline data at our institution showed high rates of incomplete documentation of PMH/PSH/FH. The aim of our project was to decrease the incidence of “no PMH/PSH/FH on file” documented in pediatric hospital medicine (PHM) H&Ps to less than 5% over 4 months.
Design/Methods: Using quality improvement methodology, we analyzed 1129 patient encounters admitted to PHM resident teams 3/1/21-6/30/21. Interventions included implementing a clinical decision support (CDS) tool (Figure 2) into PHM H&P templates to display SmartLinks with a wildcard (***), or hard stop, if no history was documented in the History tab (Figure 1b). This prevented providers from signing notes until the wildcard was addressed. The CDS tool included hyperlinks to the History tab, encouraging proper documentation. Subsequent interventions included resident reminders to use the PHM templates with the CDS tool. Our outcome measure was the percent of H&Ps with “no PMH/PSH/FH on file”. Our process measure was the percentage of H&Ps that used PHM H&P templates containing our CDS tool. Our balancing measure was the percent of notes with “none” for FH rather than documenting pertinent positives or negatives. This workaround allowed providers to sign H&Ps with incomplete documentation while avoiding “no FH on file”.
Results: Baseline data showed an incidence of “no PMH/PSH/FH on file” as 7.9%, 18.7%, and 8.3% respectively. After interventions, special cause variation was seen with improvement to 1.2%, 2.2%, and 2.9% respectively (Figure 3). Utilization of PHM H&P templates remained high at 87.2% without special cause variation. No changes in the balancing measure noted.Conclusion(s): The creation of a simple CDS tool in PHM H&P templates decreased the incidence of “no PMH/PSH/FH on file”, surpassing our goal of < 5%. Future interventions include emphasizing the use of the PHM H&P templates with incoming residents to further culture change and incorporating this CDS tool into templates outside of PHM.
Sabrina E Caro, MD Curriculum VitaeSEC CV 12.27.21.pdf
Figure 2: The CDS wildcard tool build in the template.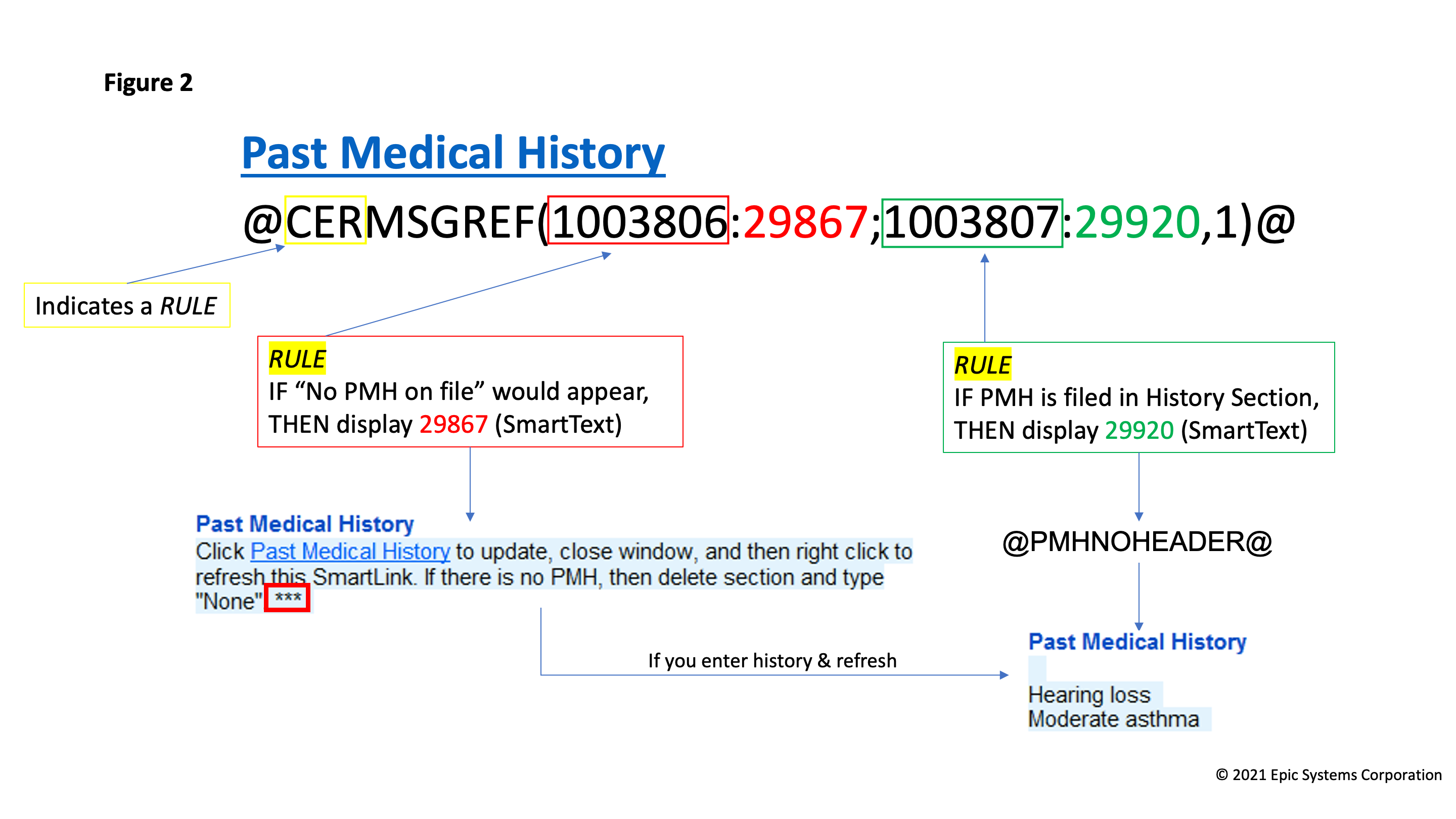
Objective: Baseline data at our institution showed high rates of incomplete documentation of PMH/PSH/FH. The aim of our project was to decrease the incidence of “no PMH/PSH/FH on file” documented in pediatric hospital medicine (PHM) H&Ps to less than 5% over 4 months.
Design/Methods: Using quality improvement methodology, we analyzed 1129 patient encounters admitted to PHM resident teams 3/1/21-6/30/21. Interventions included implementing a clinical decision support (CDS) tool (Figure 2) into PHM H&P templates to display SmartLinks with a wildcard (***), or hard stop, if no history was documented in the History tab (Figure 1b). This prevented providers from signing notes until the wildcard was addressed. The CDS tool included hyperlinks to the History tab, encouraging proper documentation. Subsequent interventions included resident reminders to use the PHM templates with the CDS tool. Our outcome measure was the percent of H&Ps with “no PMH/PSH/FH on file”. Our process measure was the percentage of H&Ps that used PHM H&P templates containing our CDS tool. Our balancing measure was the percent of notes with “none” for FH rather than documenting pertinent positives or negatives. This workaround allowed providers to sign H&Ps with incomplete documentation while avoiding “no FH on file”.
Results: Baseline data showed an incidence of “no PMH/PSH/FH on file” as 7.9%, 18.7%, and 8.3% respectively. After interventions, special cause variation was seen with improvement to 1.2%, 2.2%, and 2.9% respectively (Figure 3). Utilization of PHM H&P templates remained high at 87.2% without special cause variation. No changes in the balancing measure noted.Conclusion(s): The creation of a simple CDS tool in PHM H&P templates decreased the incidence of “no PMH/PSH/FH on file”, surpassing our goal of < 5%. Future interventions include emphasizing the use of the PHM H&P templates with incoming residents to further culture change and incorporating this CDS tool into templates outside of PHM.
Sabrina E Caro, MD Curriculum VitaeSEC CV 12.27.21.pdf
Figure 2: The CDS wildcard tool build in the template.

