Back
Telemedicine/EHR/Medical Informatics
Category: Abstract Submission
Telemedicine/EHR/Medical Informatics I
293 - Using Inpatient Telehealth for Family Engagement: Perceptions from Patients, Families, and Care Team Providers
Sunday, April 24, 2022
3:30 PM – 6:00 PM US MT
Poster Number: 293
Publication Number: 293.346
Publication Number: 293.346
Jennifer Rosenthal, University of California Davis, Sacramento, CA, United States; Jacob T. Williams, University of California, Davis, School of Medicine, Sacramento, CA, United States; Keegan F. Bowers, Kaiser Permanente - Oakland Medical Center, Berkley, CA, United States; Lori K. Madden, UC Davis Health, Sacramento, CA, United States

Jennifer Rosenthal, MD, MAS
Associate Professor
University of California Davis
Sacramento, California, United States
Presenting Author(s)
Background: Telehealth permits family members to virtually transmit into the hospital and communicate with the patient and health care team through secure, live video. Although the use of telehealth for hospitalized patients was rapidly adopted across the nation in the setting of the COVID-19 pandemic, research is needed to evaluate these clinical interventions.
Objective: To understand the experiences of using telehealth for family engagement of hospitalized patients from the perspectives of patients, families, and care team providers.
Design/Methods: We conducted a qualitative study using interviews and thematic analysis. Participants included patients, family members, and providers. We used convenience sampling to recruit participants who had used, or facilitated the use of, Inpatient Telehealth. We subsequently recruited participants with no experienced using or facilitating Inpatient Telehealth. Sampling continued until we reached thematic saturation. Interviews were audio recorded and transcribed. Data were examined iteratively using a framework analysis of concepts pertaining to the Medical Research Council process evaluation framework. Three researchers independently performed memo-writing and coding. We met to discuss the relevance and definitions of the coding structure and new topics from inductive coding. This iterative process was repeated with every 1-3 transcripts. We developed hypotheses about relationships among categories, revisited prior transcripts, and identified analytic themes. We used the themes to create a logic model of the relationships among the Inpatient Telehealth Program’s activities and its outcomes.
Results: We interviewed 21 total participants, including 1 patient, 4 family members, 10 nurses, 3 physicians, and 3 hospital clerks. Table 1 shows interviewee characteristics. Three themes emerged from the data: (1) Inpatient Telehealth enhanced the patient and family experience through strengthened relationships and increased support; (2) Inpatient Telehealth enhanced patient care through improved information sharing and engagement; (3) Care team providers established policies and procedures as unanticipated consequences emerged; (4) Adoption of Inpatient Telehealth remained limited despite the ubiquitous perception of its benefits. The logic model is shown in Figure 1.Conclusion(s): The use of Inpatient Telehealth for family engagement was perceived to improved family-centeredness of care. Future work is needed to overcome implementation challenges in order to support care team providers and to increase awareness of this resource among patients and families.
Interview Participant Characteristics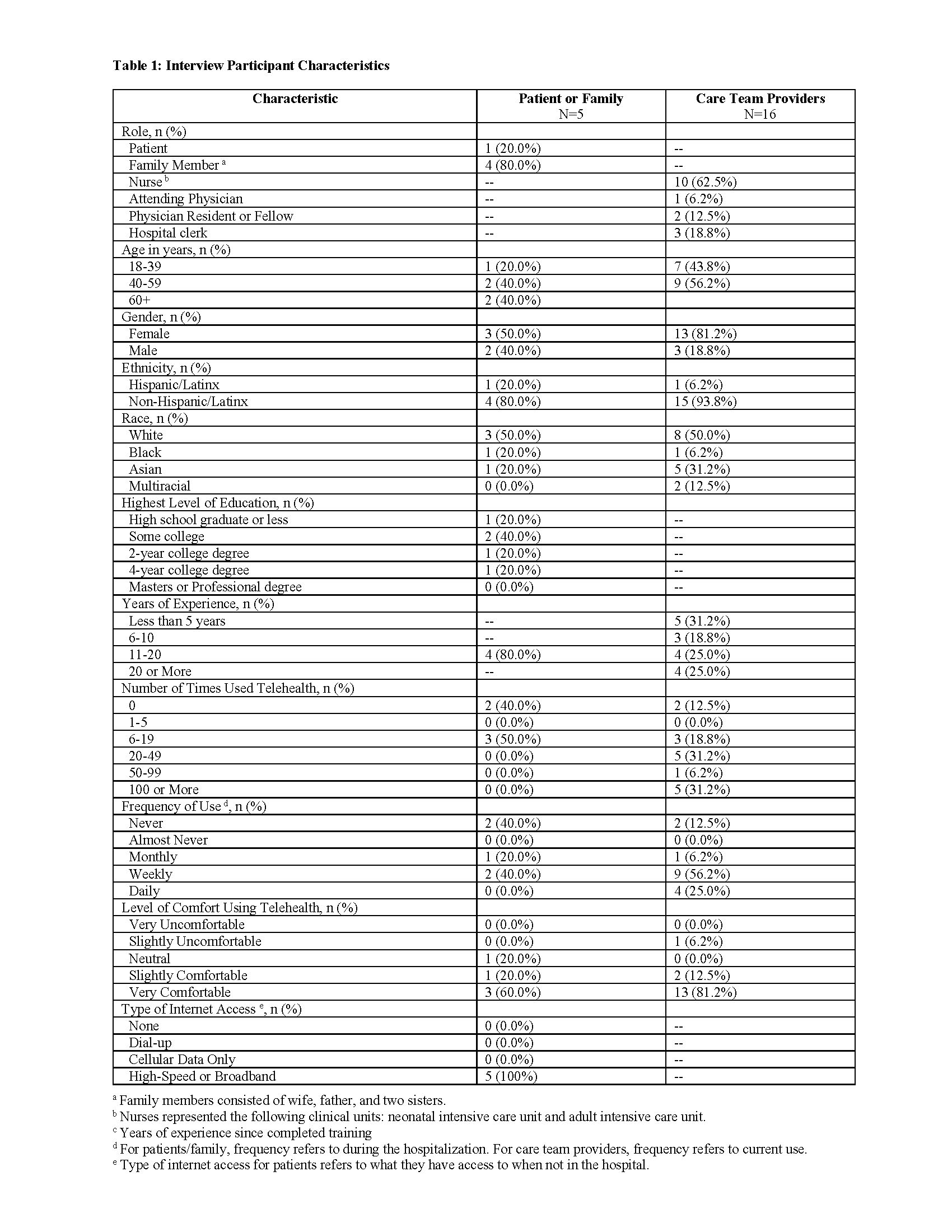
Logic Model of how the Inpatient Telehealth Program Produces its Outcomes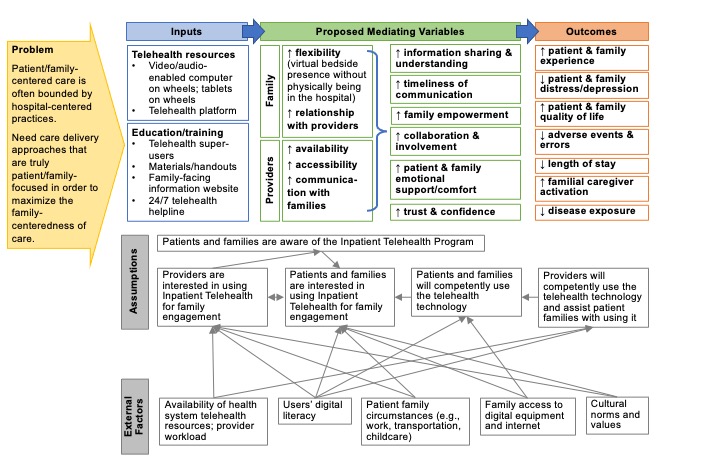
Objective: To understand the experiences of using telehealth for family engagement of hospitalized patients from the perspectives of patients, families, and care team providers.
Design/Methods: We conducted a qualitative study using interviews and thematic analysis. Participants included patients, family members, and providers. We used convenience sampling to recruit participants who had used, or facilitated the use of, Inpatient Telehealth. We subsequently recruited participants with no experienced using or facilitating Inpatient Telehealth. Sampling continued until we reached thematic saturation. Interviews were audio recorded and transcribed. Data were examined iteratively using a framework analysis of concepts pertaining to the Medical Research Council process evaluation framework. Three researchers independently performed memo-writing and coding. We met to discuss the relevance and definitions of the coding structure and new topics from inductive coding. This iterative process was repeated with every 1-3 transcripts. We developed hypotheses about relationships among categories, revisited prior transcripts, and identified analytic themes. We used the themes to create a logic model of the relationships among the Inpatient Telehealth Program’s activities and its outcomes.
Results: We interviewed 21 total participants, including 1 patient, 4 family members, 10 nurses, 3 physicians, and 3 hospital clerks. Table 1 shows interviewee characteristics. Three themes emerged from the data: (1) Inpatient Telehealth enhanced the patient and family experience through strengthened relationships and increased support; (2) Inpatient Telehealth enhanced patient care through improved information sharing and engagement; (3) Care team providers established policies and procedures as unanticipated consequences emerged; (4) Adoption of Inpatient Telehealth remained limited despite the ubiquitous perception of its benefits. The logic model is shown in Figure 1.Conclusion(s): The use of Inpatient Telehealth for family engagement was perceived to improved family-centeredness of care. Future work is needed to overcome implementation challenges in order to support care team providers and to increase awareness of this resource among patients and families.
Interview Participant Characteristics

Logic Model of how the Inpatient Telehealth Program Produces its Outcomes

