Back
Emergency Medicine: Quality Improvement
Category: Abstract Submission
Emergency Medicine XIV
45 - Characterizing Diagnostic Error Rate In The Pediatric Emergency Department Population Using The Safer DX Tool.
Monday, April 25, 2022
3:30 PM – 6:00 PM US MT
Poster Number: 45
Publication Number: 45.407
Publication Number: 45.407
Meagan Ladell, Medical College of Wisconsin, Wauwatosa, WI, United States; Jesse White, Medical College of Wisconsin, Milwaukee, WI, United States; Joseph Bartoletti, Medical College of Wisconsin, Milwaukee, WI, United States; Mark Nimmer, Medical College of Wisconsin, Milwaukee, WI, United States; Matthew C. Scanlon, Medical College of Wisconsin, Milwaukee, WI, United States; Brett J. Bordini, Medical College of Wisconsin, Milwaukee, WI, United States; Danny G. Thomas, Medical College of Wisconsin, Milwaukee, WI, United States; Abigail Schuh, Medical College of Wisconsin, Menomonee Falls, WI, United States

Meagan Ladell, MD
Pediatric Emergency Medicine Fellow
Medical College of Wisconsin
Medical College of Wisconsin
Wauwatosa, Wisconsin, United States
Presenting Author(s)
Background: Diagnostic errors occur in up to 15% of all medical encounters; however, published data on diagnostic error within pediatrics are lacking. The rapid pace of patient-physician interactions make the Emergency Department (ED) a natural laboratory to study diagnostic error. Patients with 10-day ED revisits were identified as a population at risk for diagnostic error warranting further characterization.
Objective: We conducted a retrospective chart review of 10-day revisits to characterize the rate of diagnostic errors and evaluate for secondary characteristics associated with diagnostic safety.
Design/Methods: A retrospective chart review from 1/1/2019 to 12/31/19 identified 3,684 index ED visits, resulting in 10-day revisits among 3,292 distinct patients. We compared ED clinical impressions between the index visit and 10-day revisits; if the diagnoses were incongruent, the chart was labeled at risk for diagnostic error. A structured chart review was completed using the Safer DX tool for the at-risk charts. Two independent reviewers analyzed each chart, and discrepant responses were reviewed by a third reviewer to designate which encounters involved a diagnostic error.
Results: Of the revisits, 456 charts were identified at-risk for diagnostic error, 81 (17.8%) were deemed to involve a diagnostic error. Patients with ESI (Emergency Severity Index) triage level of 3 were at the highest risk for diagnostic error and comprised 50% of the population with diagnostic error (p < 0.05), as seen in table 1. Even though revisits are more common in patients less than two years old, this group did not have a higher incidence of diagnostic error as would be expected (Figure 1). Index encounters with lab work were associated with a lower rate of diagnostic error (12.7% if no blood work ordered vs. 20.1% of encounters without blood work (p-value < 0.05)). Language, staffing with a trainee, or the ordering of radiologic studies did not affect diagnostic error rates.Conclusion(s): We identified diagnostic errors in 17.8% of surveyed pediatric ED encounters, similar to rates within adult populations. While revisits are more prevalent in younger age groups, they are less likely to occur due to diagnostic error. Patients triaged as ESI level 3, and those who did not have labs ordered were at higher risk for diagnostic error. Further research is needed to identify the sources of diagnostic error to develop quality improvement strategies.
ML CV April 21.pdf
Figure 1. Ten Day Revisits by Age, With Diagnostic Error Classification.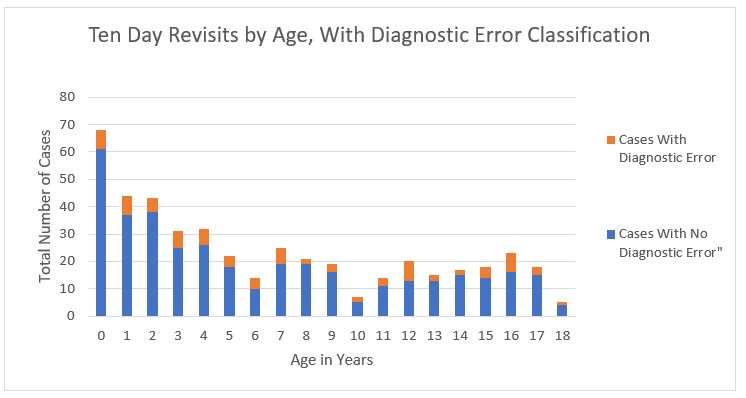
Objective: We conducted a retrospective chart review of 10-day revisits to characterize the rate of diagnostic errors and evaluate for secondary characteristics associated with diagnostic safety.
Design/Methods: A retrospective chart review from 1/1/2019 to 12/31/19 identified 3,684 index ED visits, resulting in 10-day revisits among 3,292 distinct patients. We compared ED clinical impressions between the index visit and 10-day revisits; if the diagnoses were incongruent, the chart was labeled at risk for diagnostic error. A structured chart review was completed using the Safer DX tool for the at-risk charts. Two independent reviewers analyzed each chart, and discrepant responses were reviewed by a third reviewer to designate which encounters involved a diagnostic error.
Results: Of the revisits, 456 charts were identified at-risk for diagnostic error, 81 (17.8%) were deemed to involve a diagnostic error. Patients with ESI (Emergency Severity Index) triage level of 3 were at the highest risk for diagnostic error and comprised 50% of the population with diagnostic error (p < 0.05), as seen in table 1. Even though revisits are more common in patients less than two years old, this group did not have a higher incidence of diagnostic error as would be expected (Figure 1). Index encounters with lab work were associated with a lower rate of diagnostic error (12.7% if no blood work ordered vs. 20.1% of encounters without blood work (p-value < 0.05)). Language, staffing with a trainee, or the ordering of radiologic studies did not affect diagnostic error rates.Conclusion(s): We identified diagnostic errors in 17.8% of surveyed pediatric ED encounters, similar to rates within adult populations. While revisits are more prevalent in younger age groups, they are less likely to occur due to diagnostic error. Patients triaged as ESI level 3, and those who did not have labs ordered were at higher risk for diagnostic error. Further research is needed to identify the sources of diagnostic error to develop quality improvement strategies.
ML CV April 21.pdf
Figure 1. Ten Day Revisits by Age, With Diagnostic Error Classification.

