Back
Neonatal Pulmonology
Category: Abstract Submission
Neonatal Pulmonology II: Therapies and Emerging Therapies for BPD
436 - Effects of Early CPAP on Infant Lung Structure and Function on the Developing Lung and in an Experimental Model of BPD due to Antenatal Chorioamnionitis
Monday, April 25, 2022
3:30 PM – 6:00 PM US MT
Poster Number: 436
Publication Number: 436.430
Publication Number: 436.430
Elisa Bye, University of Colorado School of Medicine, Aurora, CO, United States; Tania Gonzalez, University of Colorado School of Medicine, Aurora, CO, United States; Gregory J. Seedorf, University of Colorado School of Medicine, Aurora, CO, United States; Bradford J. Smith, Department of Bioengineering, University of Colorado Denver | Anschutz Medical Campus, Aurora, CO, United States; Nicholas W. Galambos, University of Colorado School of Medicine, Boulder, CO, United States; Steven Abman, University of Colorado School of Medicine, denver, CO, United States; Erica Mandell, University of Colorado School of Medicine, Aurora, CO, United States
- EB
Elisa Bye, BS
Professional Research Assistant
University of Colorado School of Medicine
Aurora, Colorado, United States
Presenting Author(s)
Background: Bronchopulmonary dysplasia (BPD), the chronic lung disease of prematurity, is characterized by an arrest in alveolar development. Continuous positive airway pressure (CPAP) is an increasingly common method of non-invasive respiratory support for premature infants at-risk of developing BPD to avoid more invasive and potentially injurious ventilation strategies. However, the long-term effects of CPAP on the developing lung in infants at risk for BPD are poorly understood.
Objective: We seek to understand the effect of daily CPAP on the structure and mechanical function of the developing lung in an established neonatal rat model of BPD due to antenatal inflammation from intra-amniotic endotoxin (ETX).
Design/Methods: We used a custom CPAP device to deliver constant airflow with or without positive pressure of 6 cm H2O. Pups from control (CTL) or intra-amniotic endotoxin (ETX) exposed rats were divided into three groups: no CPAP, CPAP 0 cmH2O (CTL-0 or ETX-0), and CPAP 6 cmH2O (CTL-6 or ETX-6). CPAP was delivered for 3 hrs each day from postnatal day 1 to 14 days. At day 14, we measured lung mechanics by flexiVent, and assessed lung structure by mean linear intercepts (MLI) and pulmonary vessel density (PVD).
Results: At 2 weeks of age, body weight was not different between study groups except for decreased growth in the ETX-6 group (p < 0.01 vs. other groups). Analysis of lung mechanics showed that CTL-6 rats had decreased total respiratory system resistance (Rrs) (p < 0.05) in comparison with CTL-0, and increased compliance (Crs) compared to CTL and CTL-0 (p < 0.05). In comparison with CTL-6 rats, ETX-6 rats had higher Rrs and lower Crs (p < 0.01). There were no differences in Rrs or Crs between ETX, ETX-0, and ETX-6 rats. Analysis of lung histology showed increased MLI and decreased PVD in ETX groups compared to pressure-matched controls (p < 0.05). CTL-6 rats had increased MLI (p < 0.05) and decreased PVD (p < 0.01) compared to CTL. ETX-6 rats had increased MLI (p < 0.01) compared to ETX.Conclusion(s): We found that early and prolonged CPAP decreased alveolar and vascular growth and altered lung mechanics in infant rats. Daily CPAP decreased alveolar growth after antenatal ETX but had no effects on lung mechanics or vascular growth. We speculate that although less invasive than other ventilation strategies, prolonged non-invasive respiratory support can potentially have negative effects on the normal and injured developing lung.
Lung Structure Quantification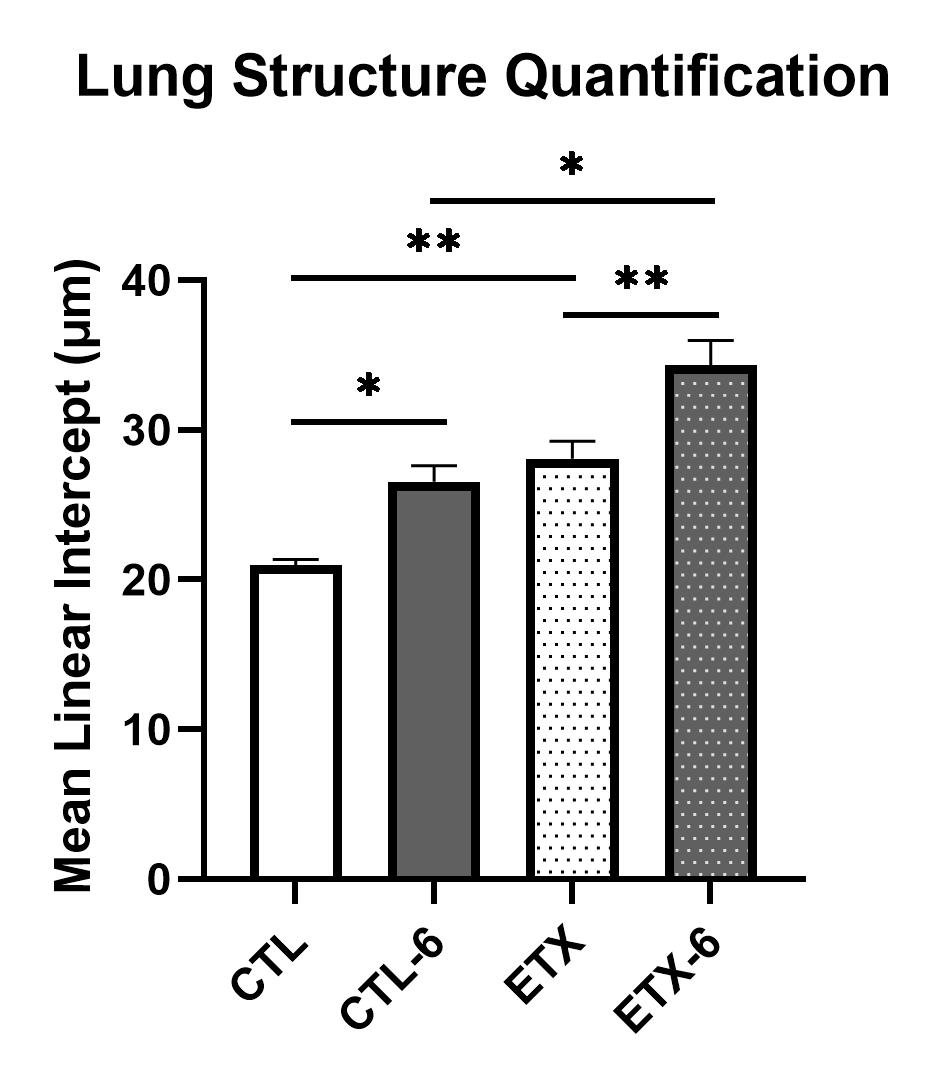
Objective: We seek to understand the effect of daily CPAP on the structure and mechanical function of the developing lung in an established neonatal rat model of BPD due to antenatal inflammation from intra-amniotic endotoxin (ETX).
Design/Methods: We used a custom CPAP device to deliver constant airflow with or without positive pressure of 6 cm H2O. Pups from control (CTL) or intra-amniotic endotoxin (ETX) exposed rats were divided into three groups: no CPAP, CPAP 0 cmH2O (CTL-0 or ETX-0), and CPAP 6 cmH2O (CTL-6 or ETX-6). CPAP was delivered for 3 hrs each day from postnatal day 1 to 14 days. At day 14, we measured lung mechanics by flexiVent, and assessed lung structure by mean linear intercepts (MLI) and pulmonary vessel density (PVD).
Results: At 2 weeks of age, body weight was not different between study groups except for decreased growth in the ETX-6 group (p < 0.01 vs. other groups). Analysis of lung mechanics showed that CTL-6 rats had decreased total respiratory system resistance (Rrs) (p < 0.05) in comparison with CTL-0, and increased compliance (Crs) compared to CTL and CTL-0 (p < 0.05). In comparison with CTL-6 rats, ETX-6 rats had higher Rrs and lower Crs (p < 0.01). There were no differences in Rrs or Crs between ETX, ETX-0, and ETX-6 rats. Analysis of lung histology showed increased MLI and decreased PVD in ETX groups compared to pressure-matched controls (p < 0.05). CTL-6 rats had increased MLI (p < 0.05) and decreased PVD (p < 0.01) compared to CTL. ETX-6 rats had increased MLI (p < 0.01) compared to ETX.Conclusion(s): We found that early and prolonged CPAP decreased alveolar and vascular growth and altered lung mechanics in infant rats. Daily CPAP decreased alveolar growth after antenatal ETX but had no effects on lung mechanics or vascular growth. We speculate that although less invasive than other ventilation strategies, prolonged non-invasive respiratory support can potentially have negative effects on the normal and injured developing lung.
Lung Structure Quantification

