Back
Medical Education: Resident
Category: Abstract Submission
Medical Education 14 - Medical Education: Resident V
275 - Evaluating the Effectiveness of Educational Interventions in Improving Recognition and Diagnosis of Pediatric Hypertension
Monday, April 25, 2022
3:30 PM – 6:00 PM US MT
Poster Number: 275
Publication Number: 275.420
Publication Number: 275.420
Camille Carre, University of South Florida Pediatric Residency, Saint Petersburg, FL, United States; Brandy M. Compton, University of South Florida, Tampa, FL, United States; Lana Soylu, University of South Florida Morsani College of Medicine, Tampa, FL, United States; Diane Straub, University of Colorado School of Medicine, Denver, CO, United States; Michelle A. Blanco, USF Health Morsani College of Medicine, Tampa, FL, United States
- CC
Camille Carre, MD
Resident
University of South Florida Pediatric Residency
Saint Petersburg, Florida, United States
Presenting Author(s)
Background: Pediatric Hypertension (HTN) is frequently underrecognized by providers and subsequently underdiagnosed and mismanaged. The 2017 AAP guidelines on Screening and Management of High Blood Pressure (BP) provide updated recommendations to improve HTN identification, classification, and management. Our ambulatory clinic has an AAP-based clinical protocol for obtainment and recognition of abnormal BP as well as diagnosis and management clinical pathways.
Objective: The objectives of this study were to use these standardized practices to 1) assess and enhance nursing and pediatric resident BP obtainment technique and 2) improve provider knowledge of the current HTN guidelines.
Design/Methods: There were two phases. Intervention during phase 1 included lectures reviewing the protocol and pathway for pediatric residents and nursing staff. Phase 2 intervention added in-person objective structured clinical examinations (OSCEs) for BP obtainment and expansion of nursing education to our satellite clinic. OSCEs included a stepwise checklist to demonstrate proper technique. Resident knowledge of protocol and pathway was assessed with pre- and post-intervention multiple choice surveys. Nursing staff knowledge of protocol was assessed with pre- and post- intervention true/false quizzes. A one-tailed paired T-test was used for statistical analysis.
Results: Surveys were completed by 32 and 29 residents pre- and post-intervention, respectively, during phase one, and 21 and 19 residents in during phase two, out of 56 residents in our Pediatrics program. Resident knowledge of process of BP verification, BP classification, and recognition of special populations, increased from 34% to 95% (p < 0.001), 44% to 47% (p=0.4), and 32% to 95% (p < 0.001) in the post-intervention period. 19 residents completed OSCEs, with score improvement from 76% to 98% post-intervention (p < 0.001). Quizzes were completed by 12 nursing staff during phase one and 21 (with OSCEs) during phase two across the two pediatric clinics. Nursing protocol comprehension was 92% pre- and 90% post-intervention (p=0.32). Nursing OSCE scores were 99% post-intervention.Conclusion(s): Resident and nursing staff AAP-based protocol comprehension and BP obtainment technique improved with education and individual skill assessment sessions. Nursing staff already had a high level of protocol comprehension, which explains why their results were not statistically significant. Next steps include chart review to evaluate if better guideline understanding and BP obtainment correlates with improved diagnosis and management of pediatric HTN.
Camille Carre CVCarre_CV_January2022.pdf
Assessment and OSCE scores Per Resident Class Pre- and Post- Intervention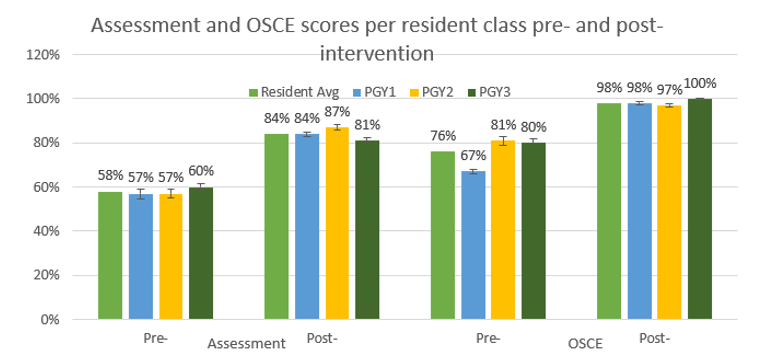 Figure 2. Scores on MCQ assessment and OSCE both pre- and post-intervention divided by resident class. Standard deviation noted.
Figure 2. Scores on MCQ assessment and OSCE both pre- and post-intervention divided by resident class. Standard deviation noted.
Objective: The objectives of this study were to use these standardized practices to 1) assess and enhance nursing and pediatric resident BP obtainment technique and 2) improve provider knowledge of the current HTN guidelines.
Design/Methods: There were two phases. Intervention during phase 1 included lectures reviewing the protocol and pathway for pediatric residents and nursing staff. Phase 2 intervention added in-person objective structured clinical examinations (OSCEs) for BP obtainment and expansion of nursing education to our satellite clinic. OSCEs included a stepwise checklist to demonstrate proper technique. Resident knowledge of protocol and pathway was assessed with pre- and post-intervention multiple choice surveys. Nursing staff knowledge of protocol was assessed with pre- and post- intervention true/false quizzes. A one-tailed paired T-test was used for statistical analysis.
Results: Surveys were completed by 32 and 29 residents pre- and post-intervention, respectively, during phase one, and 21 and 19 residents in during phase two, out of 56 residents in our Pediatrics program. Resident knowledge of process of BP verification, BP classification, and recognition of special populations, increased from 34% to 95% (p < 0.001), 44% to 47% (p=0.4), and 32% to 95% (p < 0.001) in the post-intervention period. 19 residents completed OSCEs, with score improvement from 76% to 98% post-intervention (p < 0.001). Quizzes were completed by 12 nursing staff during phase one and 21 (with OSCEs) during phase two across the two pediatric clinics. Nursing protocol comprehension was 92% pre- and 90% post-intervention (p=0.32). Nursing OSCE scores were 99% post-intervention.Conclusion(s): Resident and nursing staff AAP-based protocol comprehension and BP obtainment technique improved with education and individual skill assessment sessions. Nursing staff already had a high level of protocol comprehension, which explains why their results were not statistically significant. Next steps include chart review to evaluate if better guideline understanding and BP obtainment correlates with improved diagnosis and management of pediatric HTN.
Camille Carre CVCarre_CV_January2022.pdf
Assessment and OSCE scores Per Resident Class Pre- and Post- Intervention
 Figure 2. Scores on MCQ assessment and OSCE both pre- and post-intervention divided by resident class. Standard deviation noted.
Figure 2. Scores on MCQ assessment and OSCE both pre- and post-intervention divided by resident class. Standard deviation noted.