Back
Neonatal Pulmonology
Category: Abstract Submission
Neonatal Pulmonology IV: Lung Cellular Molecular Biology and Biomarkers
460 - Extracellular Vesicles as nanoparticle mediators in bronchopulmonary dysplasia in extremely preterm infants.
Monday, April 25, 2022
3:30 PM – 6:00 PM US MT
Poster Number: 460
Publication Number: 460.432
Publication Number: 460.432
Shaili Amatya, Penn State College of Medicine, Hershey, PA, United States; Roopa Siddaiah, Penn State Children's Hospital, Hershey, PA, United States; Han Chen, Penn State College of Medicine, Hershey, PA, United States; Mi Zhou, Pennsylvania State University College of Medicine, Hershey, PA, United States; Yuanjun Zhao, Pennsylvania State University College of Medicine, Hershey, PA, United States; Zissis C. Chroneos, Pennsylvania State University College of Medicine, Hershey, PA, United States

Shaili Amatya, MD, FAAP
Assistant Professor
Penn State College of Medicine
Hershey, Pennsylvania, United States
Presenting Author(s)
Background: Extremely preterm infants are at risk of developing pulmonary disease of prematurity as respiratory distress syndrome (RDS) and chronic disease as bronchopulmonary dysplasia (BPD). Meanwhile, there are no sensitive biomarkers available to identify the transition from RDS to BPD, predict prognosis and monitor therapy. A promising biomarker may be present in circulating extracellular vesicles (EV). Secreted by cells into biological fluids, EVs are nanoparticles that play an important role in local and systemic cell-to-cell communication by transporting genetic (microRNA, DNA) and protein cargo to distal recipient cells. As a suitable liquid biopsy, EVs encapsulate molecular information in a bilayer lipid membrane that is stable to freezing and thawing and protects from degradation. However, EVs are not well characterized in extremely preterm infants.
Objective: To investigate the proteomic profile of EVs from preterm infants at risk for BPD.
Design/Methods: Preterm infants born under 28-week gestation and 1500-gram birth weight at Penn State Children's Hospital NICU are consented and included in the study. Infants with chromosomal abnormalities, congenital heart disease, or multisystem organ failure were excluded. Blood and tracheal aspirates were collected from the infants within 7 days of life. EVs were isolated using the pureEXO precipitation kit (101Bio, CA, USA). The isolated EVs were confirmed by transmission electron microscopy (TEM) and Western blot analysis of EV markers CD63, HSP70, and Flotillin. EV size distribution and concentration were quantified by nanoparticle tracking analysis (NTA). The EV proteomic profile was investigated by mass spectrometry analysis and identification tools. Venn diagrams and protein ontology classifications analysis was performed using the functional enrichment analysis tool (FunRich). This ongoing study is approved by the IRB at Penn State College of Medicine
Results: EVs were successfully isolated from extremely preterm infants' biofluids collected from blood and tracheal aspirates as indicated by morphological, biophysical (Figure 1), and biochemical criteria. In addition, protein comparison and ontology analysis of mass spectrometry data revealed unique proteins and enrichment of proteins involved in the immune response in BPD samples compared to EV proteins in Exocarta and Vesiclepedia databases (Figure 2, 3).Conclusion(s): We report successful isolation of EVs from biofluids of extremely preterm infants. BPD EVs are a promising approach to identify biomarkers and mechanistic understanding of disease related to prematurity and the development of BPD.
TEM and NTA images of isolated EVs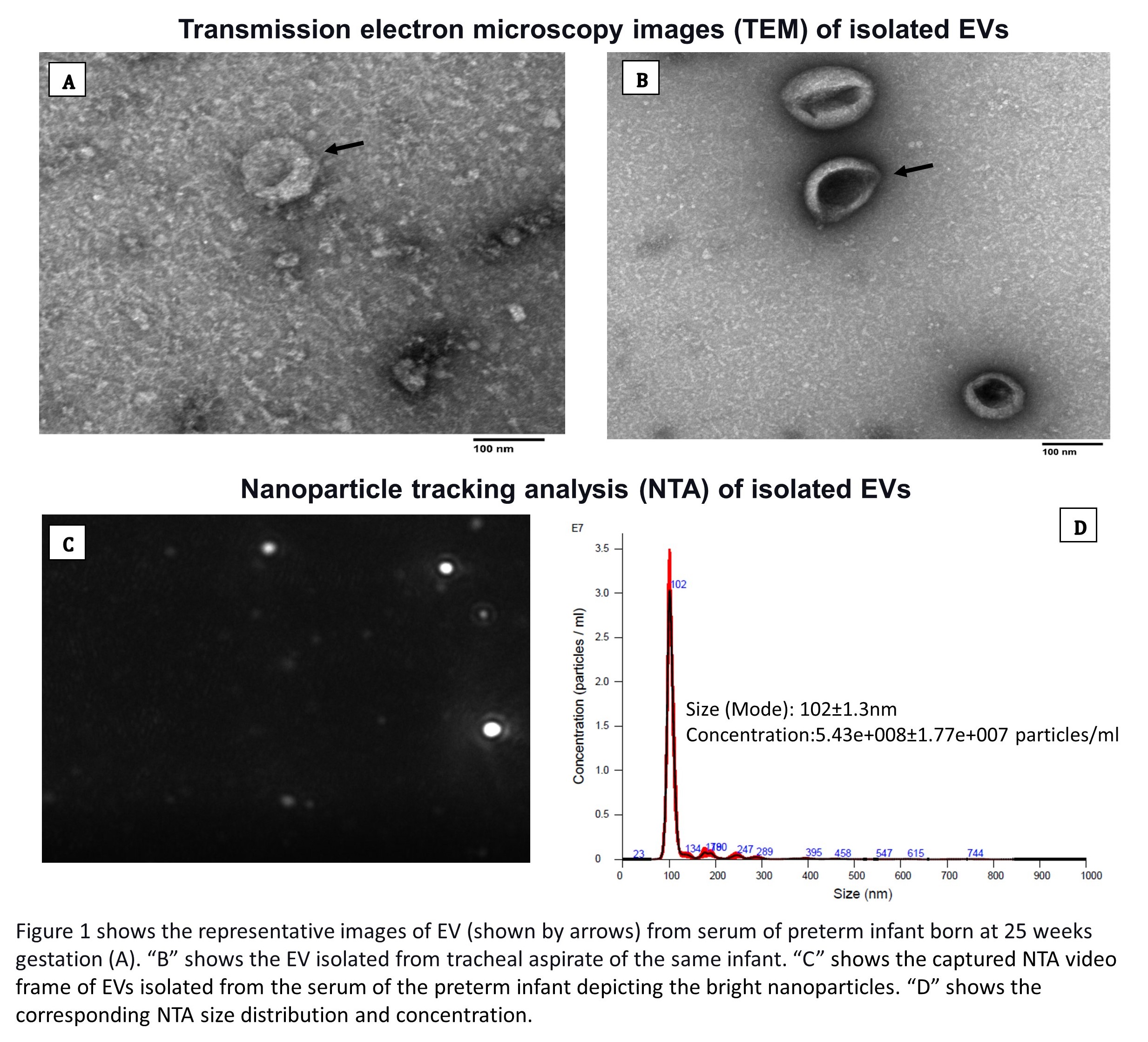
Venn diagram and cellular component of serum derived extracellular vesicles (EV) proteomic profile at 7 days of life in extremely preterm infants with and without BPD compared to EV database- Vesiclepedia and Exocarta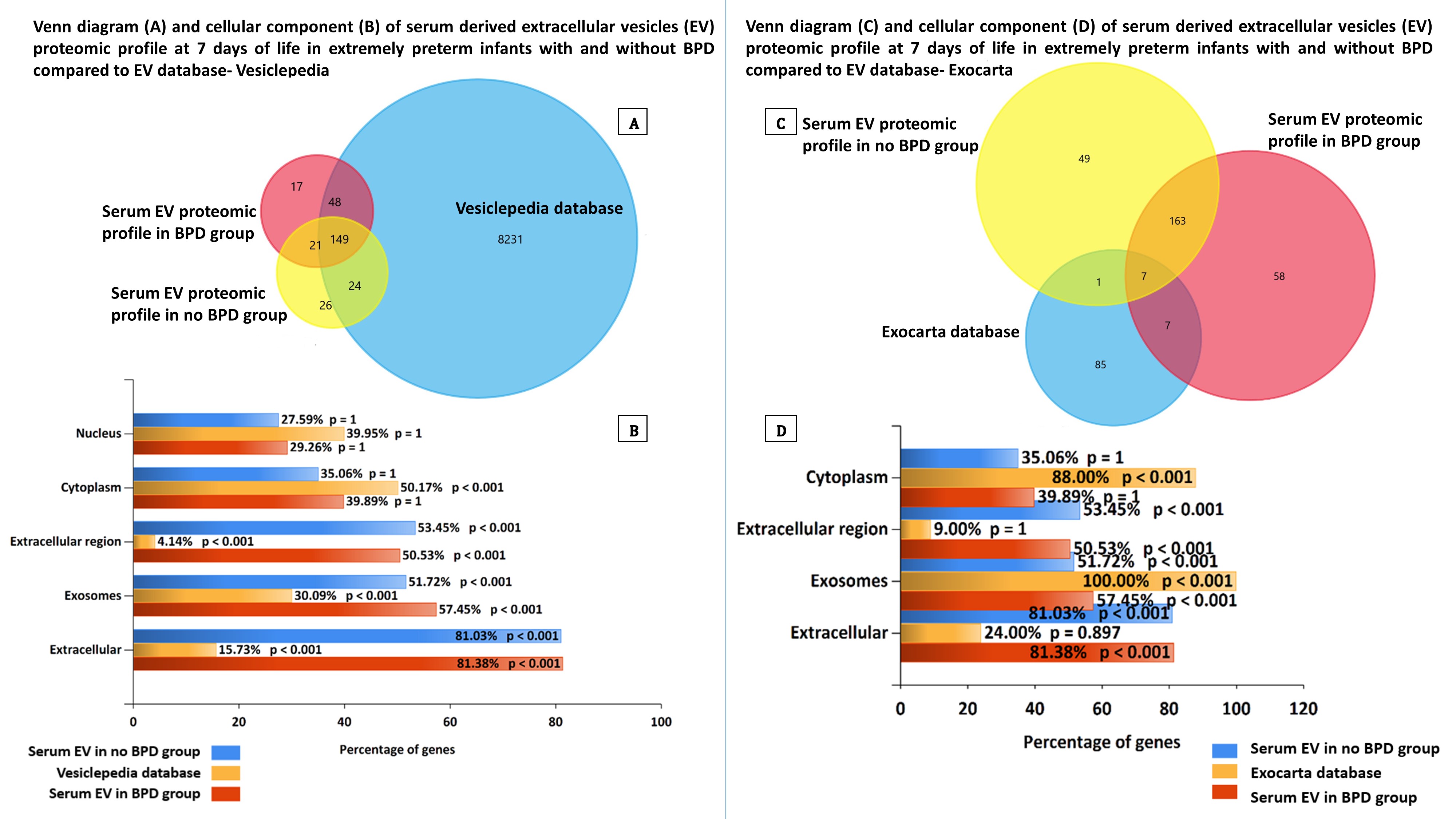
Objective: To investigate the proteomic profile of EVs from preterm infants at risk for BPD.
Design/Methods: Preterm infants born under 28-week gestation and 1500-gram birth weight at Penn State Children's Hospital NICU are consented and included in the study. Infants with chromosomal abnormalities, congenital heart disease, or multisystem organ failure were excluded. Blood and tracheal aspirates were collected from the infants within 7 days of life. EVs were isolated using the pureEXO precipitation kit (101Bio, CA, USA). The isolated EVs were confirmed by transmission electron microscopy (TEM) and Western blot analysis of EV markers CD63, HSP70, and Flotillin. EV size distribution and concentration were quantified by nanoparticle tracking analysis (NTA). The EV proteomic profile was investigated by mass spectrometry analysis and identification tools. Venn diagrams and protein ontology classifications analysis was performed using the functional enrichment analysis tool (FunRich). This ongoing study is approved by the IRB at Penn State College of Medicine
Results: EVs were successfully isolated from extremely preterm infants' biofluids collected from blood and tracheal aspirates as indicated by morphological, biophysical (Figure 1), and biochemical criteria. In addition, protein comparison and ontology analysis of mass spectrometry data revealed unique proteins and enrichment of proteins involved in the immune response in BPD samples compared to EV proteins in Exocarta and Vesiclepedia databases (Figure 2, 3).Conclusion(s): We report successful isolation of EVs from biofluids of extremely preterm infants. BPD EVs are a promising approach to identify biomarkers and mechanistic understanding of disease related to prematurity and the development of BPD.
TEM and NTA images of isolated EVs

Venn diagram and cellular component of serum derived extracellular vesicles (EV) proteomic profile at 7 days of life in extremely preterm infants with and without BPD compared to EV database- Vesiclepedia and Exocarta

