Back
Neonatal Quality Improvement
Category: Abstract Submission
Neonatal Quality Improvement II: Neurology and Infection
217 - A Late-Onset Sepsis Screening Tool Quality Improvement Initiative in a Level IV Newborn Intensive Care Unit: A Three-Year Test of Sustainment and Opportunities for Improvement
Friday, April 22, 2022
6:15 PM – 8:45 PM US MT
Poster Number: 217
Publication Number: 217.127
Publication Number: 217.127
Kelsey Simek, University of Utah School of Medicine, Salt Lake City, UT, United States; Elizabeth Elliott, Primary Children's Hospital, Salt Lake City, UT, United States; Leslie Ruybal, SCL Health - St. Vincent Healthcare, Billings, MT, United States; Laurel G. Luna, Primary Children's Hospital, Riverton, UT, United States; Peter H. Grubb, University of Utah School of Medicine, Salt Lake City, UT, United States; Con Yee Ling, University of Utah, Salt Lake City, UT, United States
.jpeg.jpg)
Kelsey A. Simek, MD
Neonatal-Perinatal Medicine Fellow
University of Utah School of Medicine
Salt Lake City, Utah, United States
Presenting Author(s)
Background: Sepsis screening tools identify at-risk patients in intensive care units (ICU) and are associated with decreased mortality. The Improving Pediatric Sepsis Outcomes collaborative recommends use of a sepsis screening tool and/or sepsis huddle. In July 2017, our newborn ICU (NICU) started a quality improvement (QI) initiative to improve recognition and management of late-onset neonatal sepsis with a paper-based NICU sepsis screening tool (NSST). Other units in our academic children’s hospital use an electronic health record (EHR)-based pediatric sepsis screening tool.
Objective: Our overall aim is to improve reliability of sepsis screening in our level IV NICU by auditing the current performance of the NSST to guide our next steps.
Design/Methods: We completed a retrospective review of NSST use from August 2–October 10, 2021 to evaluate tool performance and changes in reliability of implementation since the last follow-up sustainment audit of the original QI project 3 years ago. A Laney corrected p-chart was used to analyze the fraction of completed screening opportunities over time (Figure 1). We reviewed all NICU cases with positive blood cultures in 2021 to explore using the EHR-based pediatric sepsis screening tool with NICU patients. Prospective NSST use was also audited. Both the pediatric and NICU tools were retrospectively applied to cases and their performance compared using Fisher’s exact test. Only the first in a series of positive cultures was evaluated. We drafted a provisional key driver diagram (KDD) to suggest future directions (Figure 2).
Results: NSST completion rate ranged from 40-81% in the initial intervention and follow-up phases. Improvements occurred after targeted education, initiation of nurse champions, and weekly reporting of tool completion rates. The fraction of completed screenings during the 2021 sustainment evaluation period was steadily around 63% (Figure 1). With this level of operational reliability of implementation, the NICU tool prospectively identified 14/37 (38%) of blood culture positive cases. Applied retrospectively, the EHR-based pediatric sepsis tool identified fewer culture positive cases than the NSST (19% vs 73%, p < 0.001). Drivers for improved system reliability were identified and proposed interventions outlined during provisional KDD development (Figure 2).Conclusion(s): Our sustainment evaluation revealed a system in reasonable control, though not delivering the desired results, and numerous opportunities for improvement as outlined in the provisional KDD. Our next steps will be designed to test an EHR-integrated, automated NICU sepsis screening tool.
Figure 1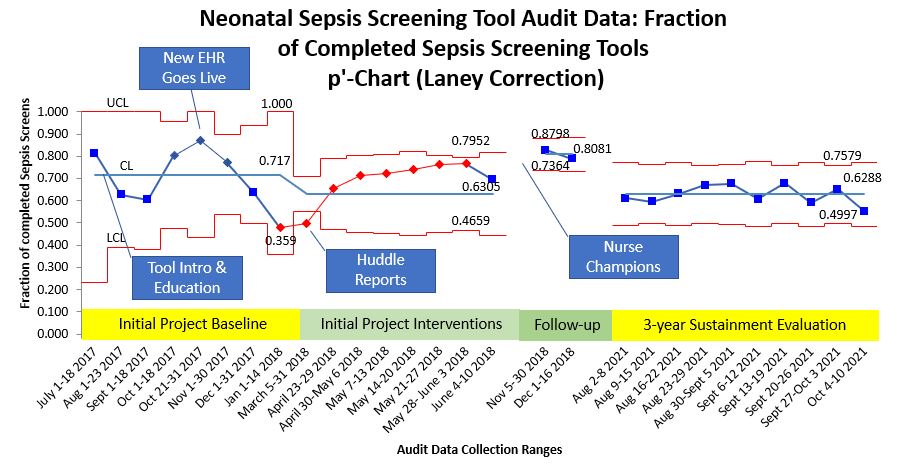
Figure 2.jpg)
Objective: Our overall aim is to improve reliability of sepsis screening in our level IV NICU by auditing the current performance of the NSST to guide our next steps.
Design/Methods: We completed a retrospective review of NSST use from August 2–October 10, 2021 to evaluate tool performance and changes in reliability of implementation since the last follow-up sustainment audit of the original QI project 3 years ago. A Laney corrected p-chart was used to analyze the fraction of completed screening opportunities over time (Figure 1). We reviewed all NICU cases with positive blood cultures in 2021 to explore using the EHR-based pediatric sepsis screening tool with NICU patients. Prospective NSST use was also audited. Both the pediatric and NICU tools were retrospectively applied to cases and their performance compared using Fisher’s exact test. Only the first in a series of positive cultures was evaluated. We drafted a provisional key driver diagram (KDD) to suggest future directions (Figure 2).
Results: NSST completion rate ranged from 40-81% in the initial intervention and follow-up phases. Improvements occurred after targeted education, initiation of nurse champions, and weekly reporting of tool completion rates. The fraction of completed screenings during the 2021 sustainment evaluation period was steadily around 63% (Figure 1). With this level of operational reliability of implementation, the NICU tool prospectively identified 14/37 (38%) of blood culture positive cases. Applied retrospectively, the EHR-based pediatric sepsis tool identified fewer culture positive cases than the NSST (19% vs 73%, p < 0.001). Drivers for improved system reliability were identified and proposed interventions outlined during provisional KDD development (Figure 2).Conclusion(s): Our sustainment evaluation revealed a system in reasonable control, though not delivering the desired results, and numerous opportunities for improvement as outlined in the provisional KDD. Our next steps will be designed to test an EHR-integrated, automated NICU sepsis screening tool.
Figure 1

Figure 2
.jpg)
