Back
Neonatal Infectious Diseases/Immunology
Category: Abstract Submission
Neonatal Infectious Diseases/Immunology: Sepsis & Antimicrobials
548 - Early Antibiotic Exposure in VLBW Infants and Risk of Late-Onset Infection
Monday, April 25, 2022
3:30 PM – 6:00 PM US MT
Poster Number: 548
Publication Number: 548.428
Publication Number: 548.428
Sarah A. Coggins, Childrens Hospital of Philadelphia, Philadelphia, PA, United States; Zachary I. Willis, University of North Carolina at Chapel Hill School of Medicine, Chapel Hill, NC, United States; Daniel Benjamin, Clemson University, Lottsburg, VA, United States; Sagori Mukhopadhyay, Childrens Hospital of Philadelphia, Philadelphia, PA, United States; Matthew Laughon, University of North Carolina at Chapel Hill School of Medicine, Chapel Hill, NC, United States; Rachel G. Greenberg, Duke Clinical Research Institute, Durham, NC, United States; Reese H. Clark, MEDNAX, Myrtle Beach, SC, United States; Karen M. Puopolo, Childrens Hospital of Philadelphia, Philadelphia, PA, United States

Sarah A. Coggins, MD
Neonatologist
Childrens Hospital of Philadelphia
Philadelphia, Pennsylvania, United States
Presenting Author(s)
Background: Very-low birth weight (VLBW) infants are commonly exposed to empiric antibiotics after birth due to increased risk of early-onset sepsis (EOS). Antibiotic stewardship efforts in EOS may be limited by concerns for delayed recognition of infection if early antibiotic regimens are deferred or shortened. However, there are minimal data quantifying the relationship between early antibiotic exposure and late-onset infection (LOI) risk during days 3-7 after birth.
Objective: To estimate risk of LOI occurring on days 3-7 after birth among preterm VLBW infants based on antibiotic exposure during days 0-2.
Design/Methods: Cohort study of infants born < 1500 grams and 22-30 weeks gestational age (GA) from 2005-2018 at 292 NICUs managed by the Pediatrix Medical Group. We excluded infants with EOS, and those who were outborn, transferred, or died during days 0-2. The exposure was any antibiotic administration during days 0-2. The outcome was LOI, defined as bloodstream infections or meningitis due to bacterial or fungal organisms, occurring during days 3-7.
Results: The cohort included 88,574 infants, of whom 75,353 (85%) were exposed to antibiotics during days 0-2. Infants administered early antibiotics had lower GA, were less likely to be small for GA and born via c-section, and more likely to receive mechanical ventilation and vasopressors during days 0-2 (Table 1). Crude LOI rates in days 3-7 were low, occurring in 1.5% of antibiotic-exposed and 2.1% of unexposed infants, with distribution of LOI day of onset shown in Table 2. Organisms causing LOI were most frequently coagulase-negative Staphylococcus (CoNS) (32%) and E. coli (19%) among antibiotic-exposed infants, and S. aureus (36%) and CoNS (21%) among unexposed infants (Table 3). Almost all fungal LOI (123 of 124, all Candida) occurred among antibiotic-exposed infants, comprising 10.6% of all LOI in that group.Conclusion(s): The rate of LOI at postnatal days 3-7 after birth was very low among preterm VLBW infants, but slightly higher among infants not exposed to antibiotics during postnatal days 0-2. LOI microbiology differed by antibiotic exposure status; Gram-negative and fungal organisms were more common among antibiotic-exposed infants, while S. aureus predominated in unexposed infants, potentially representing maternal vs. nosocomial impacts on the developing infant microbiome. Strategies to better assess patient-level infection risk in days 0-7 are needed to inform early antibiotic prescribing practices in preterm infants.
Table 1: Cohort Demographics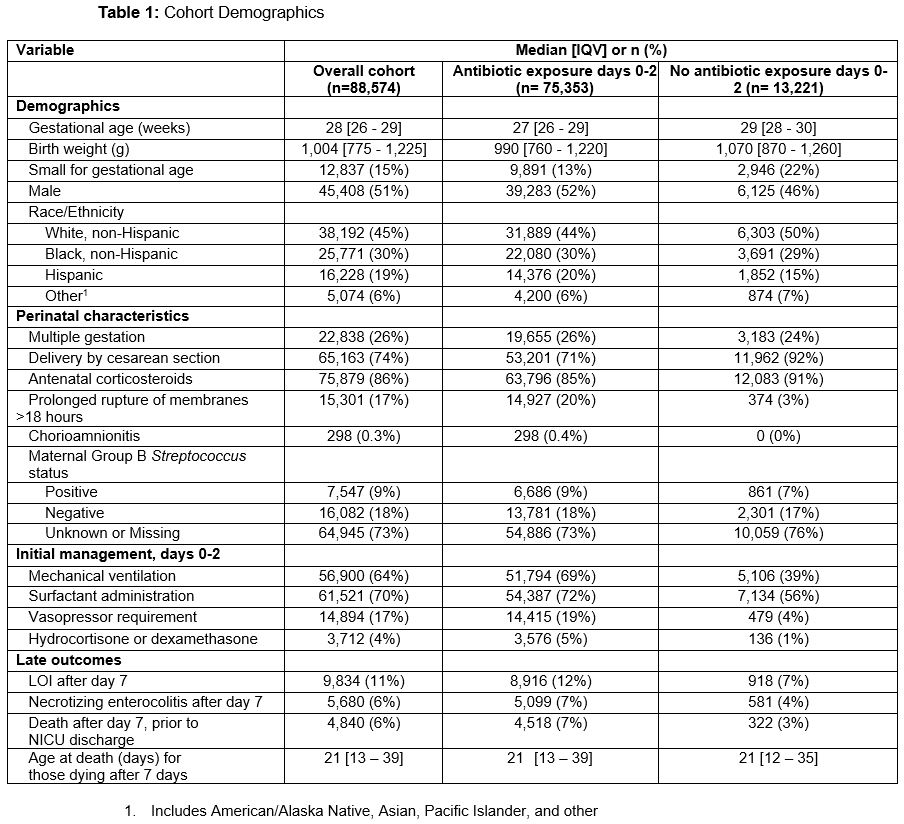
Table 2: Early Antibiotic Exposure and Rates of LOI and Death in Days 3-7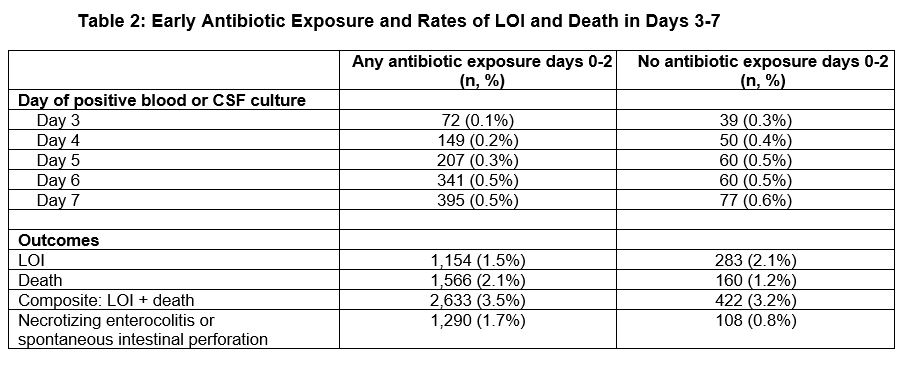
Objective: To estimate risk of LOI occurring on days 3-7 after birth among preterm VLBW infants based on antibiotic exposure during days 0-2.
Design/Methods: Cohort study of infants born < 1500 grams and 22-30 weeks gestational age (GA) from 2005-2018 at 292 NICUs managed by the Pediatrix Medical Group. We excluded infants with EOS, and those who were outborn, transferred, or died during days 0-2. The exposure was any antibiotic administration during days 0-2. The outcome was LOI, defined as bloodstream infections or meningitis due to bacterial or fungal organisms, occurring during days 3-7.
Results: The cohort included 88,574 infants, of whom 75,353 (85%) were exposed to antibiotics during days 0-2. Infants administered early antibiotics had lower GA, were less likely to be small for GA and born via c-section, and more likely to receive mechanical ventilation and vasopressors during days 0-2 (Table 1). Crude LOI rates in days 3-7 were low, occurring in 1.5% of antibiotic-exposed and 2.1% of unexposed infants, with distribution of LOI day of onset shown in Table 2. Organisms causing LOI were most frequently coagulase-negative Staphylococcus (CoNS) (32%) and E. coli (19%) among antibiotic-exposed infants, and S. aureus (36%) and CoNS (21%) among unexposed infants (Table 3). Almost all fungal LOI (123 of 124, all Candida) occurred among antibiotic-exposed infants, comprising 10.6% of all LOI in that group.Conclusion(s): The rate of LOI at postnatal days 3-7 after birth was very low among preterm VLBW infants, but slightly higher among infants not exposed to antibiotics during postnatal days 0-2. LOI microbiology differed by antibiotic exposure status; Gram-negative and fungal organisms were more common among antibiotic-exposed infants, while S. aureus predominated in unexposed infants, potentially representing maternal vs. nosocomial impacts on the developing infant microbiome. Strategies to better assess patient-level infection risk in days 0-7 are needed to inform early antibiotic prescribing practices in preterm infants.
Table 1: Cohort Demographics

Table 2: Early Antibiotic Exposure and Rates of LOI and Death in Days 3-7

