Back
Neonatal Infectious Diseases/Immunology
Category: Abstract Submission
Neonatal Infectious Diseases/Immunology: Sepsis
571 - Stool and Urine Biomarkers For Sepsis Prediction in Preterm Infants Undergoing Continuous Heart Rate Characteristics Monitoring
Monday, April 25, 2022
3:30 PM – 6:00 PM US MT
Poster Number: 571
Publication Number: 571.427
Publication Number: 571.427
Karen D. Fairchild, University of Virginia School of Medicine, Charlottesville, VA, United States; Brynne Sullivan, University of Virginia School of Medicine, KESWICK, VA, United States; Brett Moreau, University of Virginia School of Medicine, Charlottesville, VA, United States; Megan R. Elliott, University of Virginia Health, Charlottesville, VA, United States

Karen D. Fairchild, MD
Professor of Pediatrics
University of Virginia School of Medicine
Charlottesville, Virginia, United States
Presenting Author(s)
Background: Biomarkers for sepsis prediction in preterm infants could facilitate earlier detection and treatment. Continuous monitoring for abnormal heart rate characteristics (HeRO score) can alert clinicians to a systemic inflammatory response and risk for imminent sepsis. Stool microbiome and urine metabolome have been proposed as additional biomarkers to assess sepsis risk.
Objective: Conduct a pilot feasibility study of adding serial stool microbiome and targeted urine metabolome analyses (prostaglandin E2 and serotonin, 5-HT) to HeRO score monitoring for assessment of sepsis risk in preterm infants.
Design/Methods: With parental consent, infants < 32 weeks’ gestation were enrolled and stool and urine collected around 2 weeks and 5 weeks of age. HeRO score was continuously calculated and displayed as the fold increased risk of sepsis in the next 24 hours. Stool was processed by 16s rRNA sequencing using Illumina MiSeq and analyzed in R using the DADA2 pipeline. Community diversity (Pielou’s Evenness Index) and composition (relative abundance of taxonomic families) were calculated. Urine samples were extracted and analyzed using liquid chromatography mass spectrometry (LC-MS/MS). Infants were classified as “sepsis” if they had culture-positive or clinical sepsis or necrotizing enterocolitis treated with at least 5 days of antibiotics.
Results: Twenty-six infants (mean GA 27 weeks) had stool and urine collected at mean 13 days and 39 days of age, and 14 infants had sepsis (4 culture-positive, 9 clinical, 1 NEC). There was no significant difference in relative abundance of bacterial families in stool of infants with and without sepsis (Figure 1A), but evenness of bacterial families measured by Pielou’s Evenness Index was significantly lower in infants with sepsis at the 5 week timepoint (Figure 1B). Urine PGE2 was not significantly different but urine 5-HT was significantly lower in infants with sepsis at the 2 week timepoint (Figure 2). There was no significant correlation between maximum HeRO score and urine PGE2 or 5-HT.Conclusion(s): Preterm infants with sepsis had a more uneven stool microbiome, and lower urine serotonin levels.
Figure 1: Stool microbiome in infants with and without sepsis.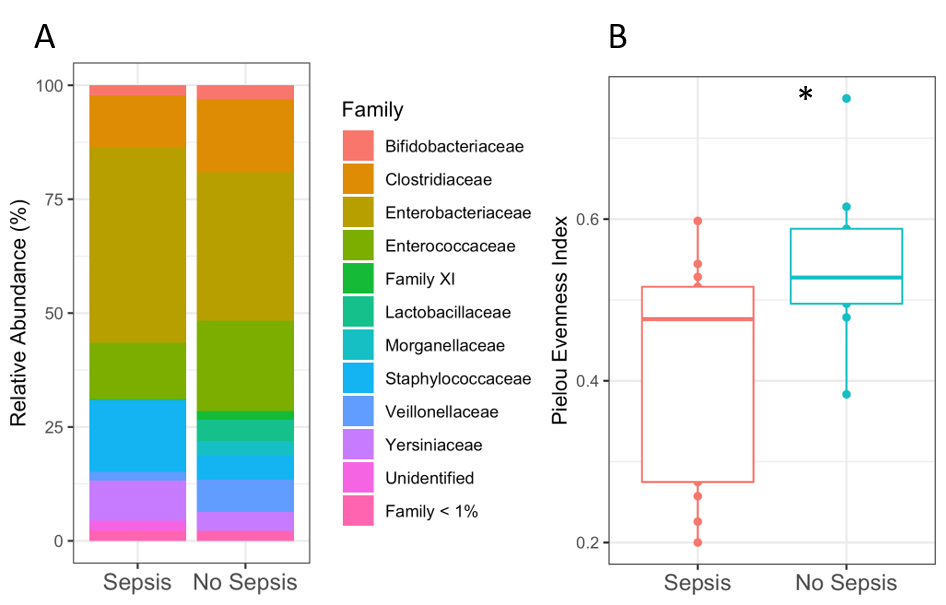 Data are shown for the second timepoint. A) Relative abundance of bacterial families was not significantly different. B) Evenness of bacterial families (Pielou units) was significantly lower in infants with sepsis (*p=0.03)
Data are shown for the second timepoint. A) Relative abundance of bacterial families was not significantly different. B) Evenness of bacterial families (Pielou units) was significantly lower in infants with sepsis (*p=0.03)
Figure 2: Urine PGE2 and 5-HT in infants with and without sepsis.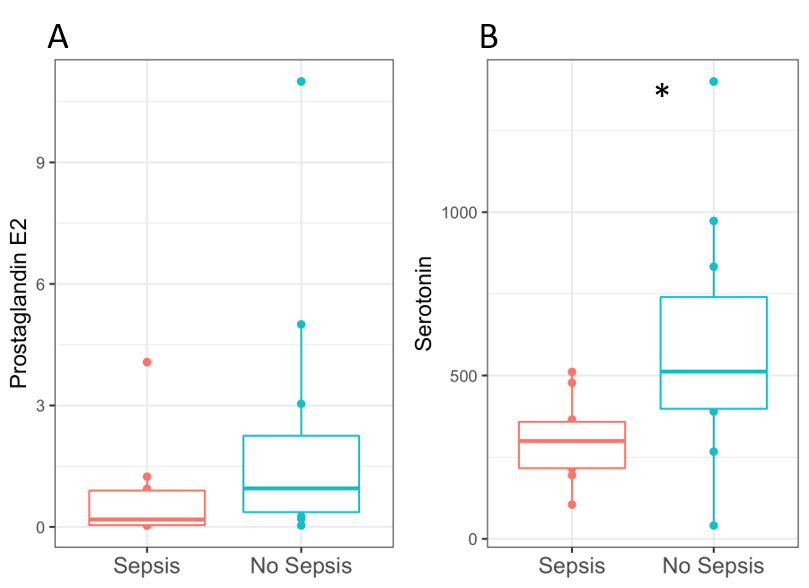 Data are shown for the first timepoint. A) Urine PGE2 was not significantly different. B) Urine serotonin was significantly lower in infants with sepsis (*p=0.028)
Data are shown for the first timepoint. A) Urine PGE2 was not significantly different. B) Urine serotonin was significantly lower in infants with sepsis (*p=0.028)
Objective: Conduct a pilot feasibility study of adding serial stool microbiome and targeted urine metabolome analyses (prostaglandin E2 and serotonin, 5-HT) to HeRO score monitoring for assessment of sepsis risk in preterm infants.
Design/Methods: With parental consent, infants < 32 weeks’ gestation were enrolled and stool and urine collected around 2 weeks and 5 weeks of age. HeRO score was continuously calculated and displayed as the fold increased risk of sepsis in the next 24 hours. Stool was processed by 16s rRNA sequencing using Illumina MiSeq and analyzed in R using the DADA2 pipeline. Community diversity (Pielou’s Evenness Index) and composition (relative abundance of taxonomic families) were calculated. Urine samples were extracted and analyzed using liquid chromatography mass spectrometry (LC-MS/MS). Infants were classified as “sepsis” if they had culture-positive or clinical sepsis or necrotizing enterocolitis treated with at least 5 days of antibiotics.
Results: Twenty-six infants (mean GA 27 weeks) had stool and urine collected at mean 13 days and 39 days of age, and 14 infants had sepsis (4 culture-positive, 9 clinical, 1 NEC). There was no significant difference in relative abundance of bacterial families in stool of infants with and without sepsis (Figure 1A), but evenness of bacterial families measured by Pielou’s Evenness Index was significantly lower in infants with sepsis at the 5 week timepoint (Figure 1B). Urine PGE2 was not significantly different but urine 5-HT was significantly lower in infants with sepsis at the 2 week timepoint (Figure 2). There was no significant correlation between maximum HeRO score and urine PGE2 or 5-HT.Conclusion(s): Preterm infants with sepsis had a more uneven stool microbiome, and lower urine serotonin levels.
Figure 1: Stool microbiome in infants with and without sepsis.
 Data are shown for the second timepoint. A) Relative abundance of bacterial families was not significantly different. B) Evenness of bacterial families (Pielou units) was significantly lower in infants with sepsis (*p=0.03)
Data are shown for the second timepoint. A) Relative abundance of bacterial families was not significantly different. B) Evenness of bacterial families (Pielou units) was significantly lower in infants with sepsis (*p=0.03)Figure 2: Urine PGE2 and 5-HT in infants with and without sepsis.
 Data are shown for the first timepoint. A) Urine PGE2 was not significantly different. B) Urine serotonin was significantly lower in infants with sepsis (*p=0.028)
Data are shown for the first timepoint. A) Urine PGE2 was not significantly different. B) Urine serotonin was significantly lower in infants with sepsis (*p=0.028)