Back
Neonatal Infectious Diseases/Immunology
Category: Abstract Submission
Neonatal Infectious Diseases/Immunology: Sepsis
572 - T-Cell Expression of Foxp3+ and Sepsis in Human Preterm Newborns
Monday, April 25, 2022
3:30 PM – 6:00 PM US MT
Poster Number: 572
Publication Number: 572.427
Publication Number: 572.427
Kimberly N. Baran, Loyola University Chicago Stritch School of Medicine, Wood Dale, IL, United States; Makio Iwashima, Loyola University Chicago, Maywood,, IL, United States; Phillip J. DeChristopher, Loyola University Chicago Stritch School of Medicine, Maywood, IL, United States; Michaela O'Neill, Loyola University Chicago Stritch School of Medicine, Chicago, IL, United States; Aleksandra Vuchkovska, Loyola University Chicago Stritch School of Medicine, Chicago, IL, United States; Yi Wei Lim, Loyola University Chicago Stritch School of Medicine, Chicago, IL, United States; Anya Nikolai, IIT Research Institute, Brookfield, IL, United States; Jonathan Muraskas, Loyola University Medical Center, maywood, IL, United States

Kimberly N. Baran, DO
Neonatal Fellow
Loyola University Chicago Stritch School of Medicine
Wood Dale, Illinois, United States
Presenting Author(s)
Background: The newborn immune system is functionally unique as it is highly tolerogenic to benign antigens such as food, maternal antigens, and commensal bacteria. One of the factors impacting this tolerant nature is the elevated propensity of newborn T-cells to differentiate into Foxp3+ regulatory T-cells (Tregs) upon activation. Foxp3+ is a transcription factor in Treg development, which function as specialized T-cells that prevent aberrant inflammation, playing central roles in the regulation of immune responses to self-antigens, allergens, and commensal microbiota and keeping the immune responses in check. Preterm newborns are also especially susceptible to life-threatening infections as their restricted immunologic reactivity contributes to reduced pathogen clearance. Excessive Treg-mediated immunosuppression could potentially cause tolerance against infecting microbes and further increase the risk of sepsis.
Objective: Identify if T-cell expression of Foxp3+ is elevated in preterm newborns with sepsis.
Design/Methods: Peripheral blood nucleated cells from 16 preterm newborns ( < 32 weeks gestational age) (obtained weekly from day 0 to week 6 after birth) were isolated using Ficoll gradient. CD4 and CD8 T-cells were labeled with an antibody against Foxp3+. Degree of labeling was determined by flow cytometry (FACS Fortessa) and analyzed by FlowJo software to determine the expression of Foxp3+ by CD4 and CD8 T-cells.
Results: Out of 16 preterm newborns, 8 developed sepsis, onset ranging from 3-48 days of life. Among the 8 with sepsis, 5 showed significantly elevated Foxp3+ expression among CD4 T-cells (>30%) compared to the 8 preterm newborns without sepsis (p < 0.05, Fisher exact test). Four of these 5 preterm infants with sepsis did not have elevated levels of Foxp3+ at birth, rather the increases were observed a few days before the diagnosis of sepsis.Conclusion(s): These data suggest that peripheral blood CD4 T-cells expression of Foxp3+ may be an early indicator of sepsis in preterm newborns and could be utilized as a tool to monitor the preterm newborn immune system in their neonatal course. Additionally, because the elevated levels are not typically seen immediately at birth, this suggests the expansion of Foxp3+ T-cells is likely induced, possibly signaling an early stage of infection. Future studies could reveal how these T-cell subsets function and how they change during the course of sepsis in the preterm newborn.
Table 1. Preterm Newborns with Sepsis and Foxp3+ Expression Levels.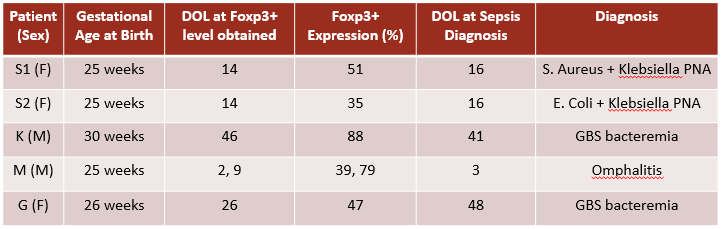 DOL = day of life. PNA = pneumonia.
DOL = day of life. PNA = pneumonia.
Table 2. Fisher Exact Analysis of Foxp3+ Expression in Preterm Newborns With and Without Sepsis.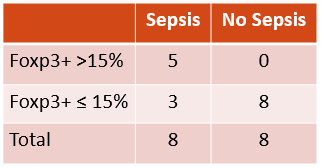 P < 0.05.
P < 0.05.
Objective: Identify if T-cell expression of Foxp3+ is elevated in preterm newborns with sepsis.
Design/Methods: Peripheral blood nucleated cells from 16 preterm newborns ( < 32 weeks gestational age) (obtained weekly from day 0 to week 6 after birth) were isolated using Ficoll gradient. CD4 and CD8 T-cells were labeled with an antibody against Foxp3+. Degree of labeling was determined by flow cytometry (FACS Fortessa) and analyzed by FlowJo software to determine the expression of Foxp3+ by CD4 and CD8 T-cells.
Results: Out of 16 preterm newborns, 8 developed sepsis, onset ranging from 3-48 days of life. Among the 8 with sepsis, 5 showed significantly elevated Foxp3+ expression among CD4 T-cells (>30%) compared to the 8 preterm newborns without sepsis (p < 0.05, Fisher exact test). Four of these 5 preterm infants with sepsis did not have elevated levels of Foxp3+ at birth, rather the increases were observed a few days before the diagnosis of sepsis.Conclusion(s): These data suggest that peripheral blood CD4 T-cells expression of Foxp3+ may be an early indicator of sepsis in preterm newborns and could be utilized as a tool to monitor the preterm newborn immune system in their neonatal course. Additionally, because the elevated levels are not typically seen immediately at birth, this suggests the expansion of Foxp3+ T-cells is likely induced, possibly signaling an early stage of infection. Future studies could reveal how these T-cell subsets function and how they change during the course of sepsis in the preterm newborn.
Table 1. Preterm Newborns with Sepsis and Foxp3+ Expression Levels.
 DOL = day of life. PNA = pneumonia.
DOL = day of life. PNA = pneumonia.Table 2. Fisher Exact Analysis of Foxp3+ Expression in Preterm Newborns With and Without Sepsis.
 P < 0.05.
P < 0.05.