Back
Neonatal Infectious Diseases/Immunology
Category: Abstract Submission
Neonatal Infectious Diseases/Immunology: Sepsis & Antimicrobials
559 - Sepsis Recognition and Severity Assessment Via Standardized NICU Sepsis Huddle Notes
Monday, April 25, 2022
3:30 PM – 6:00 PM US MT
Poster Number: 559
Publication Number: 559.428
Publication Number: 559.428
Sarah A. Coggins, Childrens Hospital of Philadelphia, Philadelphia, PA, United States; Lakshmi Srinivasan, Children's Hospital of Philadelphia, Philadelphia, PA, United States

Sarah A. Coggins, MD
Neonatologist
Childrens Hospital of Philadelphia
Philadelphia, Pennsylvania, United States
Presenting Author(s)
Background: Sepsis is a challenging diagnosis in the NICU given nonspecific presenting signs, leading to frequent sepsis evaluations and antibiotic exposures among ultimately uninfected infants. As part of a QI initiative to improve sepsis care delivery in our level IV NICU, we implemented sepsis huddles with documentation in standardized notes.
Objective: To analyze relationships between provider-documented signs prompting sepsis evaluations and illness severity assessments with infectious outcomes.
Design/Methods: We analyzed all huddle notes documented in the electronic medical record between 9/2018 – 05/2021. Templated notes describe clinical signs prompting sepsis evaluation, illness severity (from least to most severe: green, yellow, and red), and management plans (Figure 1). We calculated descriptive statistics and test characteristics for clinical signs associated with infection presence.
Results: We analyzed 1353 huddle notes among 687 infants. There were 120 confirmed infections (9% of all huddles), of which 57 (48%) were bloodstream infections (BSI) and 57 (48%) were urinary tract infections (UTI). Clinical signs poorly distinguished patients with and without infection, with low sensitivity (ranging 1.7 – 37.1%, Table 1). The odds of infection increased significantly with higher assigned illness severity (p=0.001). Some clinical signs were associated with higher assigned illness severity (e.g., hypotension, p< 0.001); however, 85% of huddles citing hypotension as a presenting sign were classified as having no organ dysfunction (“green” or “yellow”, Table 2). There was no difference in assigned illness severity among patients with confirmed BSI vs UTI, though a higher proportion of BSI were identified to have severe sepsis (“red”, 9% BSIs vs 2% UTIs). BSIs most frequently presented with fever (40%) and worsened respiratory status (31%), while UTIs most commonly presented with respiratory signs (45%) and fever (24%).Conclusion(s): Standardized sepsis huddle notes are useful tools to measure reasoning for antibiotic initiation and clinical perceptions of illness severity. Clinical signs prompting sepsis huddles were non-specific. While illness severity assessments were often inaccurate, higher assigned illness severity was associated with presence of infection. In level IV NICUs, antimicrobial stewardship through antibiotic non-initiation may be difficult, as presenting signs are similar among infants with and without infection. QI efforts should continue to focus on early antibiotic discontinuation when cultures are negative.
Figure 1: Sepsis Huddle Note Template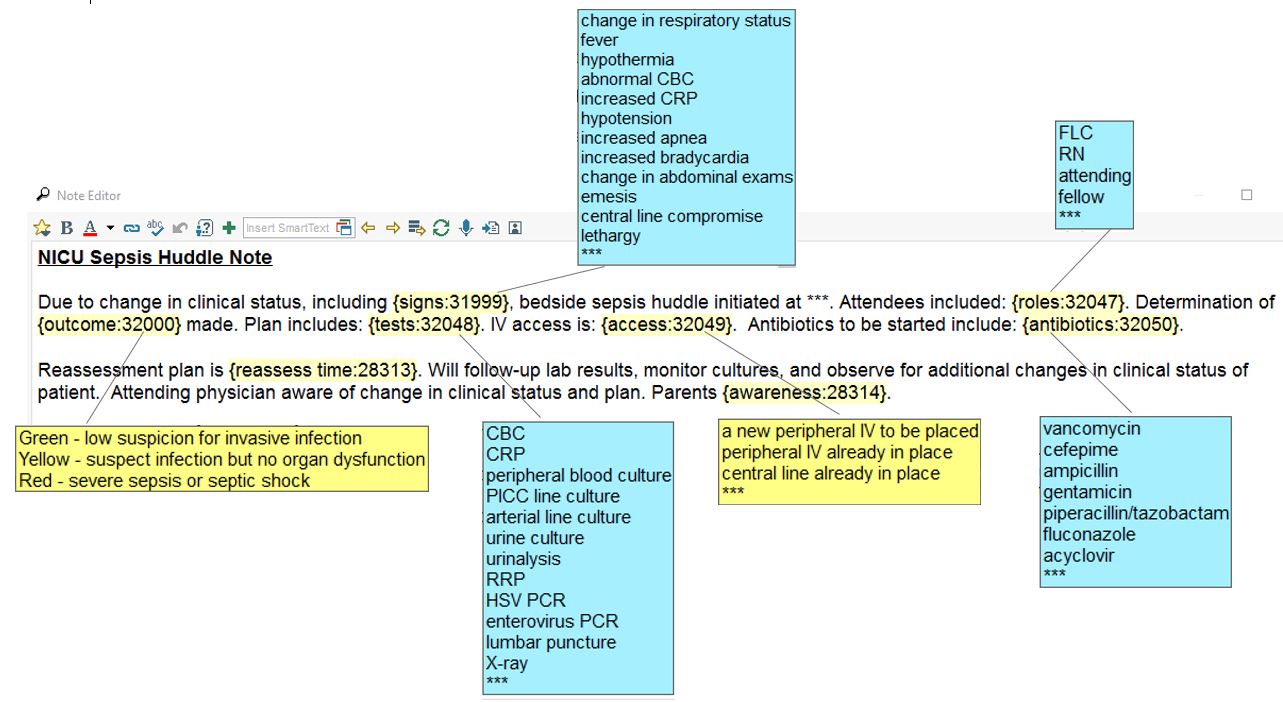
Table 1: Presenting Clinical Signs Prompting Sepsis Huddles in the NICU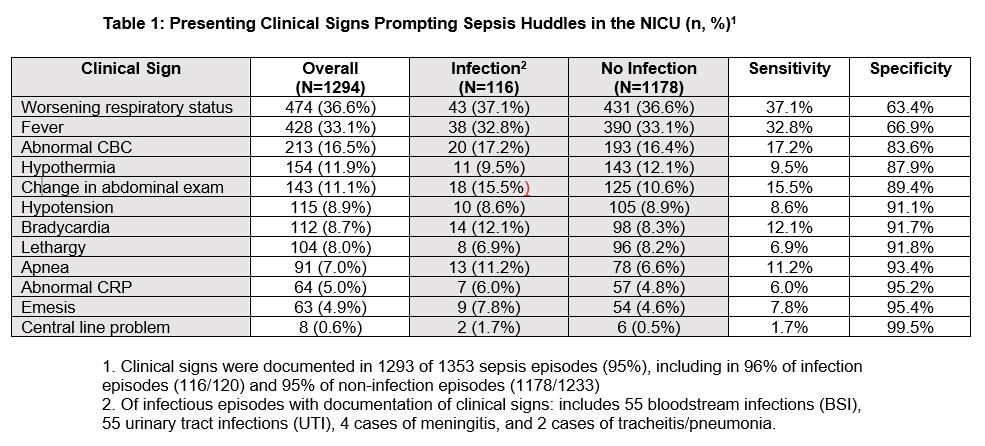
Objective: To analyze relationships between provider-documented signs prompting sepsis evaluations and illness severity assessments with infectious outcomes.
Design/Methods: We analyzed all huddle notes documented in the electronic medical record between 9/2018 – 05/2021. Templated notes describe clinical signs prompting sepsis evaluation, illness severity (from least to most severe: green, yellow, and red), and management plans (Figure 1). We calculated descriptive statistics and test characteristics for clinical signs associated with infection presence.
Results: We analyzed 1353 huddle notes among 687 infants. There were 120 confirmed infections (9% of all huddles), of which 57 (48%) were bloodstream infections (BSI) and 57 (48%) were urinary tract infections (UTI). Clinical signs poorly distinguished patients with and without infection, with low sensitivity (ranging 1.7 – 37.1%, Table 1). The odds of infection increased significantly with higher assigned illness severity (p=0.001). Some clinical signs were associated with higher assigned illness severity (e.g., hypotension, p< 0.001); however, 85% of huddles citing hypotension as a presenting sign were classified as having no organ dysfunction (“green” or “yellow”, Table 2). There was no difference in assigned illness severity among patients with confirmed BSI vs UTI, though a higher proportion of BSI were identified to have severe sepsis (“red”, 9% BSIs vs 2% UTIs). BSIs most frequently presented with fever (40%) and worsened respiratory status (31%), while UTIs most commonly presented with respiratory signs (45%) and fever (24%).Conclusion(s): Standardized sepsis huddle notes are useful tools to measure reasoning for antibiotic initiation and clinical perceptions of illness severity. Clinical signs prompting sepsis huddles were non-specific. While illness severity assessments were often inaccurate, higher assigned illness severity was associated with presence of infection. In level IV NICUs, antimicrobial stewardship through antibiotic non-initiation may be difficult, as presenting signs are similar among infants with and without infection. QI efforts should continue to focus on early antibiotic discontinuation when cultures are negative.
Figure 1: Sepsis Huddle Note Template

Table 1: Presenting Clinical Signs Prompting Sepsis Huddles in the NICU

