Back
Nephrology: Transplant
Category: Abstract Submission
Nephrology II: Transplant
38 - Metabolic Acidosis in Pediatric Transplant Recipients: Prevalence and Clinical Characteristics
Saturday, April 23, 2022
3:30 PM – 6:00 PM US MT
Poster Number: 38
Publication Number: 38.235
Publication Number: 38.235
Stella Kilduff, The Children's Hospital at Montefiore, Bronx, NY, United States; Matthew Abramowitz, Albert Einstein College of Medicine, New York, NY, United States; Nicole Hayde, Albert Einstein College of Medicine, Bronx, NY, United States

Stella Kilduff, MD
Pediatric Nephrology Fellow
The Children's Hospital at Montefiore
Bronx, New York, United States
Presenting Author(s)
Background: Adult transplant studies have revealed variable prevalence of metabolic acidosis ranging from 12-58% and have identified it be a risk factor for graft failure and patient mortality. To date, no study has assessed the prevalence of metabolic acidosis and characteristics in pediatric kidney transplant recipients.
Objective: To determine the prevalence of metabolic acidosis and examine donor/recipient characteristics in pediatric transplant patients with metabolic acidosis. We hypothesized the prevalence of acidosis would be higher in children as compared to adult transplant populations.
Design/Methods: All pediatric patients ( < 18 years) who received a kidney transplant at Montefiore Medical Center from January 1, 2010-December 31, 2018, were available for inclusion unless they underwent multi-organ transplant, experienced graft loss by 3 months, or had an estimated glomerular filtration rate (eGFR) < 30 ml/min/1.73m2 at 6 months. A total of 65 patients were identified and followed for 12 months after transplantation. Descriptive analysis of the study sample was analyzed by categories of baseline serum bicarbonate (total CO2) at 3 months post-transplant. Metabolic acidosis was defined as a serum bicarbonate < 22 meq/L or requiring the use of alkali therapy (sodium bicarbonate/citrate/citric acid).
Results: At baseline, mean serum bicarbonate was 21.7±2.4 meq/L, serum bicarbonate < 22meq/L was present in 28 (45%), and 52% of patients were receiving alkali therapy. Overall, baseline serum bicarbonate was not significantly associated with patient characteristics or transplant factors such as pre-transplant dialysis, deceased donor kidney transplant status, cold ischemia time, and eGFR (Table 1). Patients with high baseline serum bicarbonate appeared less likely to have congenital anomalies of the kidneys and urinary tract (CAKUT) as the cause of end stage renal disease (ESRD). The mean serum bicarbonate remained between 22-22.5 meq/L for the remainder of follow-up (Figure 1). The prevalence of metabolic acidosis at baseline was 68% and remained over 50% during follow-up (Figure 2). The proportion of patients with serum bicarbonate < 22 meq/L who were not receiving alkali varied from 9-14%. Of those receiving alkali therapy, 44-54% had a serum bicarbonate < 22 meq/L.Conclusion(s): Metabolic acidosis was highly prevalent within the first year post kidney transplantation in our single-center pediatric transplant cohort. Subsequent studies will look at the effect of treating metabolic acidosis on modification of outcomes as well as factors associated with non-treatment.
Table 1. Baseline characteristics of 65 pediatric kidney transplant recipients according to serum bicarbonate levels obtained at 3-months post-transplantation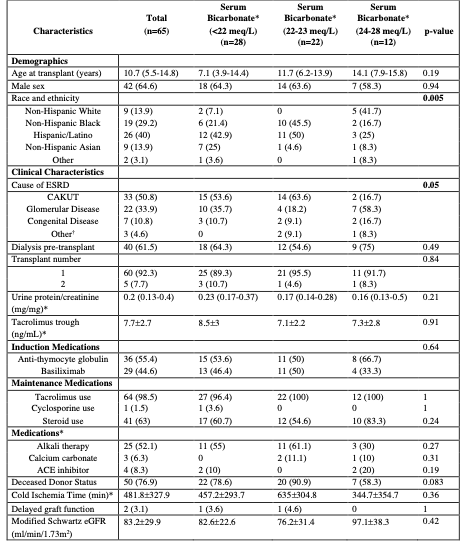 Abbreviations: ESRD=End Stage Renal Disease, CAKUT=Congenital Anomalies of the Kidneys & Urinary Tract, Alkali therapy= sodium bicarbonate/citrate/citric acid, ACE= Angiotensin-converting enzyme (ACE) inhibitors, eGFR= estimated Glomerular Filtration Rate.
Abbreviations: ESRD=End Stage Renal Disease, CAKUT=Congenital Anomalies of the Kidneys & Urinary Tract, Alkali therapy= sodium bicarbonate/citrate/citric acid, ACE= Angiotensin-converting enzyme (ACE) inhibitors, eGFR= estimated Glomerular Filtration Rate.
Categorical variables reported as n (%) and continuous variables reported as meanstandard deviation, unless otherwise noted as median (Interquartile range, IQR).
*Missing data from EMR (undergoing paper chart review to extract) include serum bicarbonate at 3 months (total CO2): n=62, total urine protein/creatine: n=54, tacrolimus trough: n=61, Medications: n=48, CIT: n=58, eGFR: n= 55
† Other category includes 2 patients with ESRD of unknown etiology and 1 patient with ESRD secondary to neoplasm.
Figure 1. Serum bicarbonate levels during the first year post-transplantation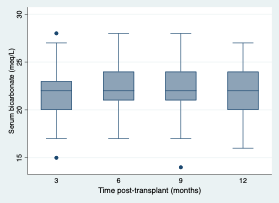
Objective: To determine the prevalence of metabolic acidosis and examine donor/recipient characteristics in pediatric transplant patients with metabolic acidosis. We hypothesized the prevalence of acidosis would be higher in children as compared to adult transplant populations.
Design/Methods: All pediatric patients ( < 18 years) who received a kidney transplant at Montefiore Medical Center from January 1, 2010-December 31, 2018, were available for inclusion unless they underwent multi-organ transplant, experienced graft loss by 3 months, or had an estimated glomerular filtration rate (eGFR) < 30 ml/min/1.73m2 at 6 months. A total of 65 patients were identified and followed for 12 months after transplantation. Descriptive analysis of the study sample was analyzed by categories of baseline serum bicarbonate (total CO2) at 3 months post-transplant. Metabolic acidosis was defined as a serum bicarbonate < 22 meq/L or requiring the use of alkali therapy (sodium bicarbonate/citrate/citric acid).
Results: At baseline, mean serum bicarbonate was 21.7±2.4 meq/L, serum bicarbonate < 22meq/L was present in 28 (45%), and 52% of patients were receiving alkali therapy. Overall, baseline serum bicarbonate was not significantly associated with patient characteristics or transplant factors such as pre-transplant dialysis, deceased donor kidney transplant status, cold ischemia time, and eGFR (Table 1). Patients with high baseline serum bicarbonate appeared less likely to have congenital anomalies of the kidneys and urinary tract (CAKUT) as the cause of end stage renal disease (ESRD). The mean serum bicarbonate remained between 22-22.5 meq/L for the remainder of follow-up (Figure 1). The prevalence of metabolic acidosis at baseline was 68% and remained over 50% during follow-up (Figure 2). The proportion of patients with serum bicarbonate < 22 meq/L who were not receiving alkali varied from 9-14%. Of those receiving alkali therapy, 44-54% had a serum bicarbonate < 22 meq/L.Conclusion(s): Metabolic acidosis was highly prevalent within the first year post kidney transplantation in our single-center pediatric transplant cohort. Subsequent studies will look at the effect of treating metabolic acidosis on modification of outcomes as well as factors associated with non-treatment.
Table 1. Baseline characteristics of 65 pediatric kidney transplant recipients according to serum bicarbonate levels obtained at 3-months post-transplantation
 Abbreviations: ESRD=End Stage Renal Disease, CAKUT=Congenital Anomalies of the Kidneys & Urinary Tract, Alkali therapy= sodium bicarbonate/citrate/citric acid, ACE= Angiotensin-converting enzyme (ACE) inhibitors, eGFR= estimated Glomerular Filtration Rate.
Abbreviations: ESRD=End Stage Renal Disease, CAKUT=Congenital Anomalies of the Kidneys & Urinary Tract, Alkali therapy= sodium bicarbonate/citrate/citric acid, ACE= Angiotensin-converting enzyme (ACE) inhibitors, eGFR= estimated Glomerular Filtration Rate.Categorical variables reported as n (%) and continuous variables reported as meanstandard deviation, unless otherwise noted as median (Interquartile range, IQR).
*Missing data from EMR (undergoing paper chart review to extract) include serum bicarbonate at 3 months (total CO2): n=62, total urine protein/creatine: n=54, tacrolimus trough: n=61, Medications: n=48, CIT: n=58, eGFR: n= 55
† Other category includes 2 patients with ESRD of unknown etiology and 1 patient with ESRD secondary to neoplasm.
Figure 1. Serum bicarbonate levels during the first year post-transplantation

