Back
Global Neonatal & Children's Health
Category: Abstract Submission
Global Child and Adolescent Health I
134 - A scoring system derived from objective criteria assists in identifying neonates with perinatal asphyxia in rural central Uganda
Friday, April 22, 2022
6:15 PM – 8:45 PM US MT
Poster Number: 134
Publication Number: 134.111
Publication Number: 134.111
Ulrike Mietzsch, University of Washington School of Medicine, Seattle, WA, United States; Krystle M. Perez, University of Washington School of Medicine, Snohomish, WA, United States; Anna B. Hedstrom, University of Washington/ Seattle Children's Hospital, Seattle, WA, United States; Rebecca Jones, Kiwoko Hospital, Kiwoko Hospital, Nakaseke, Uganda; James M. Nyonyintono, Kiwoko hospital, Kiwoko, Nakaseke, Uganda; Maneesh Batra, University of Washington School of Medicine, Seattle, WA, United States; Sara Berkelhamer, University of Washington School of Medicine, Seattle, WA, United States; Tommy Wood, University of Washington School of Medicine, Seattle, WA, United States

Ulrike Mietzsch, MD
Associate Professor of Clinical Pediatrics
University of Washington School of Medicine
Seattle, Washington, United States
Presenting Author(s)
Background: Perinatal asphyxia (PA) and infections are leading causes of neonatal death, with the majority of cases occurring in low resource settings (LRS). While therapeutic hypothermia (TH) improves outcomes after PA in high resource settings, this could not be demonstrated in LRS, potentially due to challenges identifying neonates most likely to benefit. TH provided to neonates with infection may be harmful, thus identifying neonates at such risk is important. Better tools for identifying PA soon after delivery and distinguishing neonates with other causes, particularly infections in LRS are greatly needed.
Objective: To develop a clinical score using five objective parameters associated with PA (cry at birth, need for any respiratory support, oxygen saturation, core temperature, and blood glucose level on admission) to identify neonates with PA and those with infection.
Design/Methods: Of the 1,388 admitted neonates, 1,042 had a death/discharge diagnosis of either PA (n=507) or infection (n=535). Prenatal characteristics were similar. Presentation upon admission was significantly different in all five criteria (see Table 1). Cut-offs for predicting PA are shown in Table 2. Three predictive models showed similar levels of accuracy ( >75% sensitivity and specificity): 1) using the predictors as continuous variables, 2) dichotomizing variables based on cut-offs, and 3) using a score of ³3 of the five criteria for high risk of PA (Table 3). Using an asphyxia score of ³3 in all 1,388 inborn infants regardless of final diagnosis (including training data) predicted PA with 69.9% sensitivity and 74.3% specificity (Table 3).
Results: Of the 1,388 admitted neonates, 1,042 had a death/discharge diagnosis of either PA (n=507) or infection (n=535). Prenatal characteristics were similar. Presentation upon admission was significantly different in all five criteria (see Table 1). Cut-offs for predicting PA are shown in Table 2. Three predictive models showed similar levels of accuracy ( >75% sensitivity and specificity): 1) using the predictors as continuous variables, 2) dichotomizing variables based on cut-offs, and 3) using a score of ³3 of the five criteria for high risk of PA (Table 3). Using an asphyxia score of ³3 in all 1,388 inborn infants regardless of final diagnosis (including training data) predicted PA with 69.9% sensitivity and 74.3% specificity (Table 3).Conclusion(s): Recognizing the limitations of the diagnoses used, a simple objective scoring system used during initial assessment may further improve identification of neonates compromised secondary PA and exclude those with infection.
Table 1.jpg) Admission characteristics of inborn infants admitted on the day of birth with a birth weight 2500 grams with a death or discharge diagnosis of asphyxia compared to a death or discharge diagnosis of infection.
Admission characteristics of inborn infants admitted on the day of birth with a birth weight 2500 grams with a death or discharge diagnosis of asphyxia compared to a death or discharge diagnosis of infection.
Table 2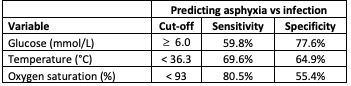 Optimal cut-offs for predicting asphyxia from individual admission variables, derived from 80% of infants with discharge or death diagnoses of infection or asphyxia.
Optimal cut-offs for predicting asphyxia from individual admission variables, derived from 80% of infants with discharge or death diagnoses of infection or asphyxia.
Objective: To develop a clinical score using five objective parameters associated with PA (cry at birth, need for any respiratory support, oxygen saturation, core temperature, and blood glucose level on admission) to identify neonates with PA and those with infection.
Design/Methods: Of the 1,388 admitted neonates, 1,042 had a death/discharge diagnosis of either PA (n=507) or infection (n=535). Prenatal characteristics were similar. Presentation upon admission was significantly different in all five criteria (see Table 1). Cut-offs for predicting PA are shown in Table 2. Three predictive models showed similar levels of accuracy ( >75% sensitivity and specificity): 1) using the predictors as continuous variables, 2) dichotomizing variables based on cut-offs, and 3) using a score of ³3 of the five criteria for high risk of PA (Table 3). Using an asphyxia score of ³3 in all 1,388 inborn infants regardless of final diagnosis (including training data) predicted PA with 69.9% sensitivity and 74.3% specificity (Table 3).
Results: Of the 1,388 admitted neonates, 1,042 had a death/discharge diagnosis of either PA (n=507) or infection (n=535). Prenatal characteristics were similar. Presentation upon admission was significantly different in all five criteria (see Table 1). Cut-offs for predicting PA are shown in Table 2. Three predictive models showed similar levels of accuracy ( >75% sensitivity and specificity): 1) using the predictors as continuous variables, 2) dichotomizing variables based on cut-offs, and 3) using a score of ³3 of the five criteria for high risk of PA (Table 3). Using an asphyxia score of ³3 in all 1,388 inborn infants regardless of final diagnosis (including training data) predicted PA with 69.9% sensitivity and 74.3% specificity (Table 3).Conclusion(s): Recognizing the limitations of the diagnoses used, a simple objective scoring system used during initial assessment may further improve identification of neonates compromised secondary PA and exclude those with infection.
Table 1
.jpg) Admission characteristics of inborn infants admitted on the day of birth with a birth weight 2500 grams with a death or discharge diagnosis of asphyxia compared to a death or discharge diagnosis of infection.
Admission characteristics of inborn infants admitted on the day of birth with a birth weight 2500 grams with a death or discharge diagnosis of asphyxia compared to a death or discharge diagnosis of infection.Table 2
 Optimal cut-offs for predicting asphyxia from individual admission variables, derived from 80% of infants with discharge or death diagnoses of infection or asphyxia.
Optimal cut-offs for predicting asphyxia from individual admission variables, derived from 80% of infants with discharge or death diagnoses of infection or asphyxia.