Neonatal Quality Improvement
Category: Abstract Submission
Neonatal Quality Improvement I
210 - Improving red reflex screening in a level III NICU through a quality improvement-based approach
Friday, April 22, 2022
6:15 PM - 8:45 PM US MT
Poster Number: 210
Publication Number: 210.126
Publication Number: 210.126
Rishika P. Sakaria, UTHSC, Memphis, TN, United States; Jennifer M. Davidson, University of Tennessee Health Science Center College of Medicine, Memphis, TN, United States; Nakia Coleman, Regional One Health, Olive Branch, MS, United States; Anna Wilcox, Regional One Health, Arlington, TN, United States; Ajay Talati, University of Tennessee Health Science Center College of Medicine, Memphis, TN, United States
- RS
Rishika P. Sakaria, MD (she/her/hers)
Assistant Professor
University of Tennessee Health Science Center College of Medicine
The University of Tennessee Health Science Center
Memphis, Tennessee, United States
Presenting Author(s)
Background: Red reflex is a routine part of newborn examination in most high-income countries. It is an inexpensive, non-invasive method of detecting serious ocular abnormalities like cataract, retinoblastoma, vitreous masses, etc. The American Academy of Pediatrics recommends red reflex examination prior to discharge from newborn nursery. However, the current rate of red reflex examination in the neonatal intensive care units (NICUs) in the US is unknown. We noted a low rate of documentation (19%) in our level III NICU, prompting us to initiate this quality improvement (QI) project to improve this rate.
Objective: Our aim was to increase the documentation rate of red reflex to >80% in our NICU by January 2021
Design/Methods: We created a key-driver diagram and summarized possible interventions to achieve our aim. We implemented various interventions over four plan-do-study-act (PDSA) cycles. Over 13 months, we educated the nurses and the providers regarding the importance of red reflex assessment, placed visual reminders to check red reflex, implemented discharge checklist for the residents and improved the accessibility to ophthalmoscope.
Results: 900 infants who did not receive a formal ophthalmology exam were discharged from our NICU during a 19-month period. The rate of red reflex documentation improved significantly from 19% in the first six month before the 1st PDSA cycle to 86% during 13-month intervention period (4 PDSA cycles). No abnormal red reflexes were detected during this study.Conclusion(s): Implementation of this project has led to a culture-change at our institution which will help prevent us from missing the diagnosis of serious visual abnormalities in the future.
Figure 1 PDSA cycles implemented to achieve SMART aim
PDSA cycles implemented to achieve SMART aim
Figure 2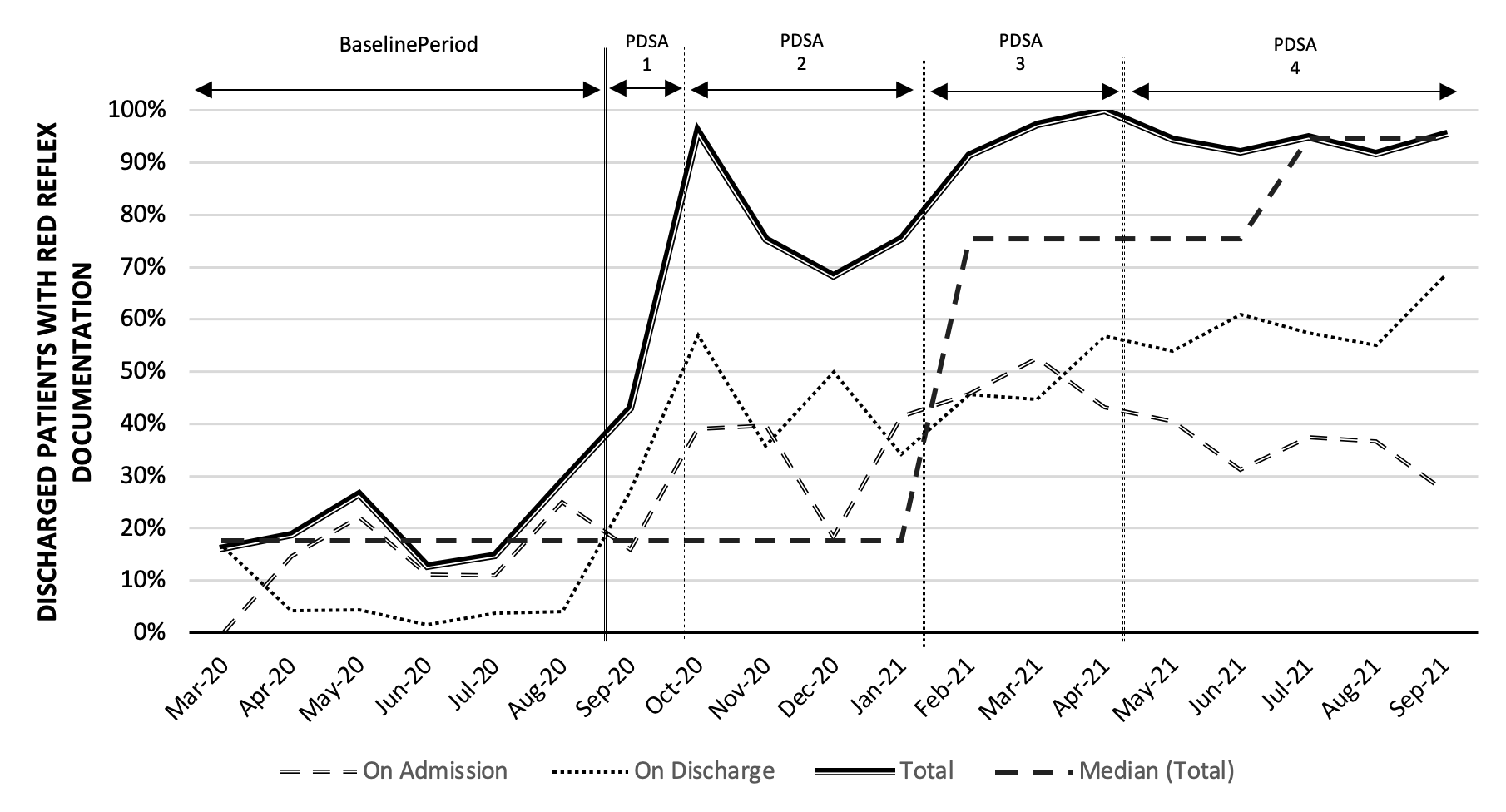 Overall trends in the red reflex documentation rate during the project period during various PDSA cycles. There was a significant positive shift in the median from 17.55% to 75.4% during the intervention period during PDSA cycle 3 and further to 94.5% during PDSA cycle 4.
Overall trends in the red reflex documentation rate during the project period during various PDSA cycles. There was a significant positive shift in the median from 17.55% to 75.4% during the intervention period during PDSA cycle 3 and further to 94.5% during PDSA cycle 4.
Objective: Our aim was to increase the documentation rate of red reflex to >80% in our NICU by January 2021
Design/Methods: We created a key-driver diagram and summarized possible interventions to achieve our aim. We implemented various interventions over four plan-do-study-act (PDSA) cycles. Over 13 months, we educated the nurses and the providers regarding the importance of red reflex assessment, placed visual reminders to check red reflex, implemented discharge checklist for the residents and improved the accessibility to ophthalmoscope.
Results: 900 infants who did not receive a formal ophthalmology exam were discharged from our NICU during a 19-month period. The rate of red reflex documentation improved significantly from 19% in the first six month before the 1st PDSA cycle to 86% during 13-month intervention period (4 PDSA cycles). No abnormal red reflexes were detected during this study.Conclusion(s): Implementation of this project has led to a culture-change at our institution which will help prevent us from missing the diagnosis of serious visual abnormalities in the future.
Figure 1
 PDSA cycles implemented to achieve SMART aim
PDSA cycles implemented to achieve SMART aimFigure 2
 Overall trends in the red reflex documentation rate during the project period during various PDSA cycles. There was a significant positive shift in the median from 17.55% to 75.4% during the intervention period during PDSA cycle 3 and further to 94.5% during PDSA cycle 4.
Overall trends in the red reflex documentation rate during the project period during various PDSA cycles. There was a significant positive shift in the median from 17.55% to 75.4% during the intervention period during PDSA cycle 3 and further to 94.5% during PDSA cycle 4.