Back
Nephrology: CKD
Category: Abstract Submission
Nephrology III: General Nephrology and Dialysis
47 - Characterization of CKD and Dialysis in Children with Sickle Cell Kidney Disease in the NAPRTCS registry
Sunday, April 24, 2022
3:30 PM – 6:00 PM US MT
Poster Number: 47
Publication Number: 47.340
Publication Number: 47.340
Rima Zahr, University of Tennessee Health Science Center College of Medicine, Memphis, TN, United States; Annabelle Chua, Duke Children's Hospital, Durham, NC, United States; Jing Zhang, Emmes LLC, Rockville, MD, United States; Shirley Galbiati, Emmes, Washington, DC, United States; Sushil Gupta, Riley Hospital for Children at Indiana University Health, Indianapolis, IN, United States
- RZ
Rima Zahr, DO (she/her/hers)
Assistant Professor
University of Tennessee Health Science Center College of Medicine
memphis, Tennessee, United States
Presenting Author(s)
Background:
Kidney damage in children with sickle cell disease (SCD), an inherited hematological disorder, occurs early in life. While the overall prevalence of chronic kidney disease (CKD) and end stage kidney disease (ESKD) in children and adults due to SCD is less than other disease etiologies, ESKD in this population results in premature death. Our current understanding on the natural progression of children with CKD and ESKD secondary to SCD is lacking.
Objective: Characterize children with CKD and ESKD within the North American Pediatric Renal Trials and Collaborative studies (NAPRTCS) registry.
Design/Methods: Utilizing the NAPRTCS registries we performed a retrospective study to characterize children with CKD or on dialysis that have SCD-associated kidney disease. Demographics and baseline characteristics were described in SCD vs. Non-SCD group. Medication usage and other clinical characteristics were compared between the two groups, and time to ESKD for CKD patients was analyzed by plotting cumulative incidence curves.
Results: The CKD registry identified 16 children with SCD-associated kidney disease. Of these participants, 75% were adolescents, were more likely to be male (62%) and were more likely to be placed on dialysis than receive a preemptive transplant as their disease progressed (Figure 1). Children with SCD required more blood transfusions at enrollment 25% vs 6% non-SCD at enrollment and treatment for hypertension was common. In the dialysis registry, 33 dialysis courses from 22 SCD children were analyzed. Children with SCD were more likely to be initiated on peritoneal dialysis (60.6%) vs. hemodialysis (HD) (39.4%). HD catheters and arteriovenous (AV) fistulas were more likely to be used when compared to AV grafts (Table 1). Antihypertensive medications were commonly used in children with SCD, 68.2% on dialysis at enrollment.
Conclusion(s):
Children with SCD associated kidney disease represent a smaller proportion of children in the CKD and Dialysis NAPRTCS registry. These children are older when enrolled and are more likely to be male. Treatment for anemia and hypertension are commonly needed in these children with CKD and dialysis.
Table 1. Clinical and Demographic Characteristics of children with and without SCD- kidney disease in the CKD and Dialysis Registry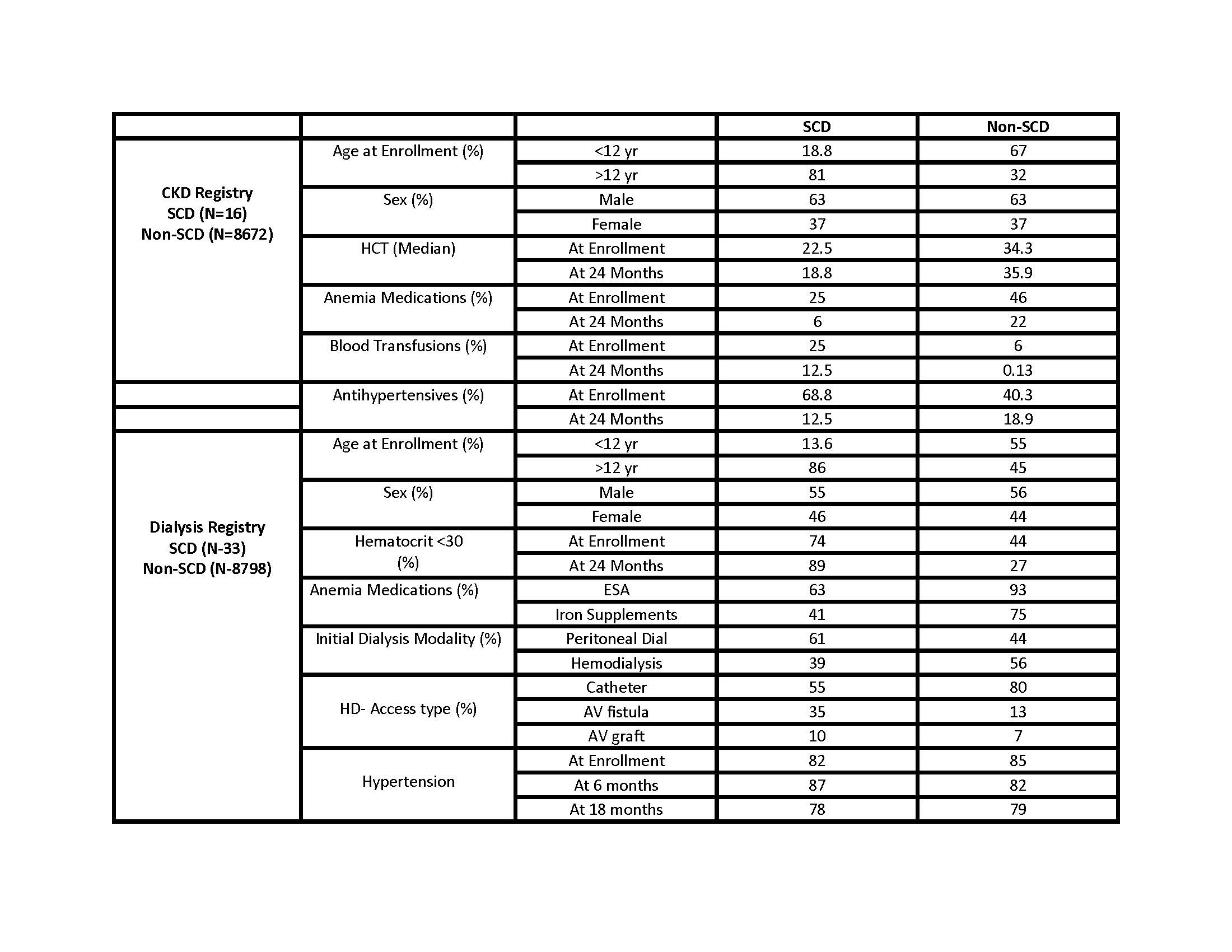
Figure 1. Comparison between CKD patients with SCD and non-SCD kidney disease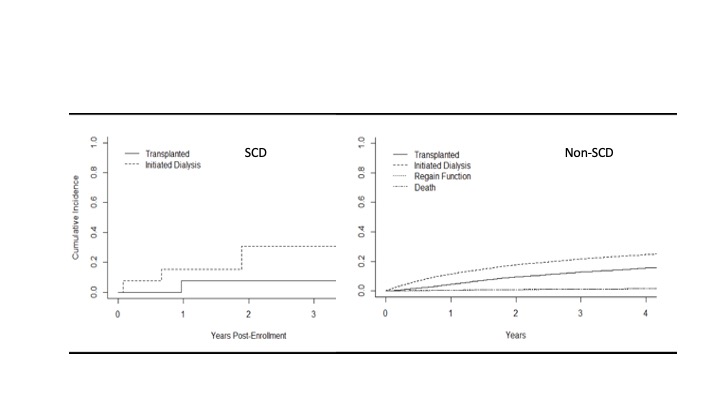 Cumulative Incidence curves, time to dialysis initiation and transplantation post enrollment in CKD Registry
Cumulative Incidence curves, time to dialysis initiation and transplantation post enrollment in CKD Registry
Kidney damage in children with sickle cell disease (SCD), an inherited hematological disorder, occurs early in life. While the overall prevalence of chronic kidney disease (CKD) and end stage kidney disease (ESKD) in children and adults due to SCD is less than other disease etiologies, ESKD in this population results in premature death. Our current understanding on the natural progression of children with CKD and ESKD secondary to SCD is lacking.
Objective: Characterize children with CKD and ESKD within the North American Pediatric Renal Trials and Collaborative studies (NAPRTCS) registry.
Design/Methods: Utilizing the NAPRTCS registries we performed a retrospective study to characterize children with CKD or on dialysis that have SCD-associated kidney disease. Demographics and baseline characteristics were described in SCD vs. Non-SCD group. Medication usage and other clinical characteristics were compared between the two groups, and time to ESKD for CKD patients was analyzed by plotting cumulative incidence curves.
Results: The CKD registry identified 16 children with SCD-associated kidney disease. Of these participants, 75% were adolescents, were more likely to be male (62%) and were more likely to be placed on dialysis than receive a preemptive transplant as their disease progressed (Figure 1). Children with SCD required more blood transfusions at enrollment 25% vs 6% non-SCD at enrollment and treatment for hypertension was common. In the dialysis registry, 33 dialysis courses from 22 SCD children were analyzed. Children with SCD were more likely to be initiated on peritoneal dialysis (60.6%) vs. hemodialysis (HD) (39.4%). HD catheters and arteriovenous (AV) fistulas were more likely to be used when compared to AV grafts (Table 1). Antihypertensive medications were commonly used in children with SCD, 68.2% on dialysis at enrollment.
Conclusion(s):
Children with SCD associated kidney disease represent a smaller proportion of children in the CKD and Dialysis NAPRTCS registry. These children are older when enrolled and are more likely to be male. Treatment for anemia and hypertension are commonly needed in these children with CKD and dialysis.
Table 1. Clinical and Demographic Characteristics of children with and without SCD- kidney disease in the CKD and Dialysis Registry

Figure 1. Comparison between CKD patients with SCD and non-SCD kidney disease
 Cumulative Incidence curves, time to dialysis initiation and transplantation post enrollment in CKD Registry
Cumulative Incidence curves, time to dialysis initiation and transplantation post enrollment in CKD Registry