Neonatal Infectious Diseases/Immunology
Category: Abstract Submission
Neonatal Infectious Diseases/Immunology: Sepsis
574 - Utility of the Neonatal Early-Onset Sepsis Calculator in a Low Risk Population
Monday, April 25, 2022
3:30 PM - 6:00 PM US MT
Poster Number: 574
Publication Number: 574.427
Publication Number: 574.427
kelley sonney, Brooke Army Medical Center, converse, TX, United States; Dakota Tomasini, SAUSHEC, San Antonio, TX, United States; Caitlin Drumm, Uniformed Services University of the Health Sciences F. Edward Hebert School of Medicine, San Antonio, TX, United States

kelley sonney, DO (she/her/hers)
Neonatology fellow
Uniformed Services University of the Health Sciences F. Edward Hebert School of Medicine
CONVERSE, Texas, United States
Presenting Author(s)
Background: Recent efforts have been made to better target infants at risk for early onset sepsis (EOS) using multivariate risk assessment via the Neonatal Early-Onset Sepsis Calculator. Infants born via cesarean section (C/S) with rupture of membranes (ROM) at time of delivery lack many traditional risk factors associated with EOS. However, these patients are at increased risk for respiratory symptoms, which can trigger sepsis evaluation and treatment when using any of the 3 currently recommended approaches to infant risk assessment. We hypothesize that the Neonatal Early-Onset Sepsis Calculator will often lead to sepsis evaluation and empiric treatment in this presumably low-risk population.
Objective: Study the utility of the Neonatal Early-Onset Sepsis Calculator in late preterm and term infants born via C/S with ROM < 10 minutes.
Design/Methods: Retrospective chart review of late preterm (≥35 + 0/7 – 36 6/7) and term (≥37) infants born at Brooke Army Medical Center (BAMC) between January 1, 2012-August 29, 2019. Inclusion: born via C/S with ROM < 10 minutes. Exclusions: born to mothers diagnosed with chorioamnionitis, transferred prior to 4 days of life, congenital anomalies.
Results: We identified 1,187 infants who met inclusion and exclusion criteria, demographic data listed in table 1. An early blood culture was drawn on 234 (19.7%) infants and 170 (14.3%) received antibiotics when using categorical risk assessment. Respiratory distress was the most common indication for sepsis work-up and occurred in 173 (14.6%) of patients. After applying the calculator to the 234 infants who underwent sepsis evaluation, clinical recommendation was to strongly consider starting empiric antibiotics on 151 (64.5%), to obtain an early blood culture on 2 (.01%) and no culture or antibiotics on 81 (34.6%). Calculator use would have eliminated antibiotic exposure in 48 infants, most of whom underwent evaluation due to hypoglycemia. Conversely, the calculator recommended strong consideration for antibiotics in 27 infants who did not receive antibiotics, mainly due to respiratory status deemed clinical illness. Within the cohort, one patient had a blood culture positive for Micrococcus luteus, deemed a contaminant. There were no cases of culture proven EOS.Conclusion(s): This population is low risk for development of EOS, but nearly 20% underwent a sepsis work-up and 15% received antibiotics. If the calculator had been used in these infants only 13% would have undergone a sepsis work up. While this 7% reduction is significant, room for improvement remains as there were no cases of blood culture proven sepsis in this population.
Table 1. Population characteristics.jpg)
Actual Vs. Recommended Antibiotic and Blood Culture Use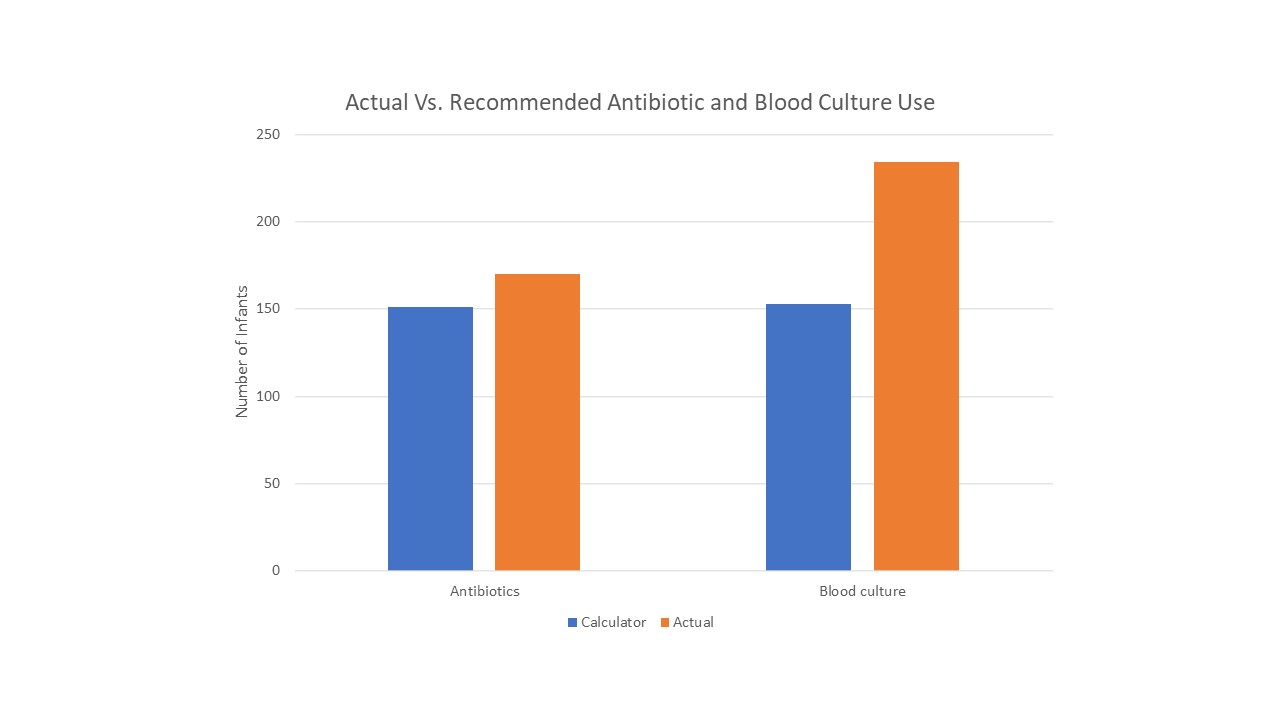
Objective: Study the utility of the Neonatal Early-Onset Sepsis Calculator in late preterm and term infants born via C/S with ROM < 10 minutes.
Design/Methods: Retrospective chart review of late preterm (≥35 + 0/7 – 36 6/7) and term (≥37) infants born at Brooke Army Medical Center (BAMC) between January 1, 2012-August 29, 2019. Inclusion: born via C/S with ROM < 10 minutes. Exclusions: born to mothers diagnosed with chorioamnionitis, transferred prior to 4 days of life, congenital anomalies.
Results: We identified 1,187 infants who met inclusion and exclusion criteria, demographic data listed in table 1. An early blood culture was drawn on 234 (19.7%) infants and 170 (14.3%) received antibiotics when using categorical risk assessment. Respiratory distress was the most common indication for sepsis work-up and occurred in 173 (14.6%) of patients. After applying the calculator to the 234 infants who underwent sepsis evaluation, clinical recommendation was to strongly consider starting empiric antibiotics on 151 (64.5%), to obtain an early blood culture on 2 (.01%) and no culture or antibiotics on 81 (34.6%). Calculator use would have eliminated antibiotic exposure in 48 infants, most of whom underwent evaluation due to hypoglycemia. Conversely, the calculator recommended strong consideration for antibiotics in 27 infants who did not receive antibiotics, mainly due to respiratory status deemed clinical illness. Within the cohort, one patient had a blood culture positive for Micrococcus luteus, deemed a contaminant. There were no cases of culture proven EOS.Conclusion(s): This population is low risk for development of EOS, but nearly 20% underwent a sepsis work-up and 15% received antibiotics. If the calculator had been used in these infants only 13% would have undergone a sepsis work up. While this 7% reduction is significant, room for improvement remains as there were no cases of blood culture proven sepsis in this population.
Table 1. Population characteristics
.jpg)
Actual Vs. Recommended Antibiotic and Blood Culture Use

